Patient specific respiratory motion modeling using a 3D patient's external surface
- PMID: 22755719
- PMCID: PMC4032399
- DOI: 10.1118/1.4718578
Patient specific respiratory motion modeling using a 3D patient's external surface
Abstract
Purpose: Respiratory motion modeling of both tumor and surrounding tissues is a key element in minimizing errors and uncertainties in radiation therapy. Different continuous motion models have been previously developed. However, most of these models are based on the use of parameters such as amplitude and phase extracted from 1D external respiratory signal. A potentially reduced correlation between the internal structures (tumor and healthy organs) and the corresponding external surrogates obtained from such 1D respiratory signal is a limitation of these models. The objective of this work is to describe a continuous patient specific respiratory motion model, accounting for the irregular nature of respiratory signals, using patient external surface information as surrogate measures rather than a 1D respiratory signal.
Methods: Ten patients were used in this study having each one 4D CT series, a synchronized RPM signal and patient surfaces extracted from the 4D CT volumes using a threshold based segmentation algorithm. A patient specific model based on the use of principal component analysis was subsequently constructed. This model relates the internal motion described by deformation matrices and the external motion characterized by the amplitude and the phase of the respiratory signal in the case of the RPM or using specific regions of interest (ROI) in the case of the patients' external surface utilization. The capability of the different models considered to handle the irregular nature of respiration was assessed using two repeated 4D CT acquisitions (in two patients) and static CT images acquired at extreme respiration conditions (end of inspiration and expiration) for one patient.
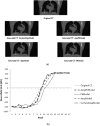
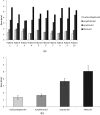
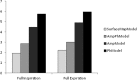
Results: Both quantitative and qualitative parameters covering local and global measures, including an expert observer study, were used to assess and compare the performance of the different motion estimation models considered. Results indicate that using surface information [correlation coefficient (CC): 0.998 ± 0.0006 and model error (ME): 1.35 ± 0.21 mm] is superior to the use of both motion phase and amplitude extracted from a 1D respiratory signal (CC and ME of 0.971 ± 0.02 and 1.64 ± 0.28 mm). The difference in performance was more substantial compared to the use of only one parameter (phase or amplitude) used in the motion model construction. Similarly, the patient surface based model was better in estimating the motion in the repeated 4D CT acquisitions and those CT images acquired at the full inspiration (FI) and the full expiration (FE). Once more, within this context the use of both amplitude and phase in the model building was substantially more robust than the use of phase or amplitude only.
Conclusions: The present study demonstrates the potential of using external patient surfaces for the construction of patient specific respiratory motion models. Such information can be obtained using different devices currently available. The use of external surface information led to the best performance in estimating internal structure motion. On the other hand, the use of both amplitude and phase parameters derived from an 1D respiration signal led to largely superior model performance relative to the use of only one of these two parameters in the model building process.
© 2012 American Association of Physicists in Medicine.
Figures


Similar articles
-
A 4D global respiratory motion model of the thorax based on CT images: A proof of concept.Med Phys. 2018 Jul;45(7):3043-3051. doi: 10.1002/mp.12982. Epub 2018 Jun 3. Med Phys. 2018. PMID: 29772057
-
Technical note: Correlation of respiratory motion between external patient surface and internal anatomical landmarks.Med Phys. 2011 Jun;38(6):3157-64. doi: 10.1118/1.3589131. Med Phys. 2011. PMID: 21815390 Free PMC article.
-
The effect of an inconsistent breathing amplitude on the relationship between an external marker and internal lung deformation in a porcine model.Med Phys. 2010 Nov;37(11):5951-60. doi: 10.1118/1.3496325. Med Phys. 2010. PMID: 21158308
-
Tumor tracking method based on a deformable 4D CT breathing motion model driven by an external surface surrogate.Int J Radiat Oncol Biol Phys. 2014 Jan 1;88(1):182-8. doi: 10.1016/j.ijrobp.2013.09.026. Int J Radiat Oncol Biol Phys. 2014. PMID: 24331665
-
Motion Management in PET/CT: Technological Solutions.Curr Radiopharm. 2018;11(2):79-85. doi: 10.2174/1874471011666180419150440. Curr Radiopharm. 2018. PMID: 29676240 Review.
Cited by
-
A Mechanics-Based Nonrigid Registration Method for Liver Surgery Using Sparse Intraoperative Data.IEEE Trans Med Imaging. 2014 Jan;33(1):147-58. doi: 10.1109/TMI.2013.2283016. Epub 2013 Sep 20. IEEE Trans Med Imaging. 2014. PMID: 24107926 Free PMC article.
-
Artificial intelligence-based motion tracking in cancer radiotherapy: A review.J Appl Clin Med Phys. 2024 Nov;25(11):e14500. doi: 10.1002/acm2.14500. Epub 2024 Aug 28. J Appl Clin Med Phys. 2024. PMID: 39194360 Free PMC article. Review.
-
3D Measurement of Human Chest and Abdomen Surface Based on 3D Fourier Transform and Time Phase Unwrapping.Sensors (Basel). 2020 Feb 17;20(4):1091. doi: 10.3390/s20041091. Sensors (Basel). 2020. PMID: 32079334 Free PMC article.
-
Ultrasound-based sensors to monitor physiological motion.Med Phys. 2021 Jul;48(7):3614-3622. doi: 10.1002/mp.14949. Epub 2021 Jun 7. Med Phys. 2021. PMID: 33999423 Free PMC article.
-
Use of MRI to assess the prediction of heart motion with gross body motion in myocardial perfusion imaging by stereotracking of markers on the body surface.Med Phys. 2013 Nov;40(11):112504. doi: 10.1118/1.4824693. Med Phys. 2013. PMID: 24320463 Free PMC article.
References
-
- Keall P. J., Mageras G. S., Balter J. M., Emery R. S., Forster K. M., Jiang S. B., Kapatoes J. M., Low D. A., Murphy M. J., Murray B. R., Ramsey C. R., van Herk M. B., Vedam S. S., Wong J. W., and Yorke E., “The management of respiratory motion in radiation oncology report of AAPM Task Group No. 76,” Med. Phys. 33, 3874–900 (2006).10.1118/1.2349696 - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

