Risk of hypotony in noninfectious uveitis
- PMID: 22796306
- PMCID: PMC3475753
- DOI: 10.1016/j.ophtha.2012.05.032
Risk of hypotony in noninfectious uveitis
Abstract
Objective: We sought to describe the risk and risk factors for hypotony in a noninfectious uveitis cohort.
Design: Retrospective cohort study.
Participants: Patients with noninfectious uveitis seen between 1979 and 2007 at 4 academic ocular inflammation specialty clinics.
Methods: Data were collected from medical records by trained, certified, expert reviewers.
Main outcome measures: Hypotony (<5 mmHg) and low intraocular pressure (<8 mmHg), each sustained for ≥ 2 visits spanning ≥ 30 days.
Results: During follow-up, 126 of 6785 patients (1.86%) developed hypotony at the rate of 0.61% (95% confidence interval [CI], 0.50-0.75%) per eye-year. Cataract surgery was associated with a 7.5-fold risk (adjusted hazard ratio [aHR], 7.51; 95% CI, 3.97-14.23) of incident hypotony. Phacoemulsification, the type of cataract surgery associated with the least hypotony risk still was associated with nearly 5-fold higher hypotony incidence (aHR, 4.87; 95% CI, 2.25-10.55). Increased risk was observed in children (aHR, 2.92; 95% CI, 1.20-7.10) with respect to young adults, and duration of uveitis of >5 years (aHR, 3.08; 95% CI, 1.30-7.31) with respect to uveitis of <6 month duration. Band keratopathy, ≥ 3+ vitreous cells, exudative retinal detachment, posterior synechia, and a history of pars plana vitrectomy also were associated with greater hypotony incidence. With respect to anterior uveitis, intermediate uveitis (aHR, 0.17; 95% CI, 0.05-0.56) and posterior uveitis (aHR, 0.11; 95% CI, 0.03-0.45) were associated with lower hypotony risk, whereas panuveitis (aHR, 1.25; 95% CI, 0.67-2.35) was similar. Approximately five-sixths (84.1%) of eyes presenting with hypotony had a visual acuity of ≤ 20/200 (aOR for visual acuity ≤ 20/200, 13.85; 95% CI, 7.23-26.53). Risk factors for prevalent hypotony were similar.
Conclusions: The risk of hypotony is low among eyes with noninfectious uveitis, but is more frequently observed in cases with anterior segment inflammation. Signs of present or past inflammation were associated with greater risk, suggesting excellent inflammatory control may reduce the risk of hypotony. Prior ocular surgery also was associated with higher risk; cataract surgery in particular was associated with much higher risk of hypotony. Lower risk of hypotony with phacoemulsification than with alternative cataract surgery approaches suggests the phacoemulsification approach is preferable.
Copyright © 2012 American Academy of Ophthalmology. Published by Elsevier Inc. All rights reserved.
Figures



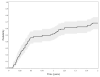
References
-
- Schubert HD. Postsurgical hypotony: relationship to fistulization, inflammation, chorioretinal lesions, and the vitreous. Surv Ophthalmol. 1996;41:97–125. - PubMed
-
- Rosenberg KD, Feuer WJ, Davis JL. Ocular complications of pediatric uveitis. Ophthalmology. 2004;111:2299–306. - PubMed
-
- Thorne JE, Woreta F, Kedhar SR, et al. Juvenile idiopathic arthritis-associated uveitis: incidence of ocular complications and visual acuity loss. Am J Ophthalmol. 2007;143:840–6. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

