Predictors of poor perinatal outcome following maternal perception of reduced fetal movements--a prospective cohort study
- PMID: 22808059
- PMCID: PMC3394759
- DOI: 10.1371/journal.pone.0039784
Predictors of poor perinatal outcome following maternal perception of reduced fetal movements--a prospective cohort study
Abstract
Background: Maternal perception of reduced fetal movement (RFM) is associated with increased risk of stillbirth and fetal growth restriction (FGR). RFM is thought to represent fetal compensation to conserve energy due to insufficient oxygen and nutrient transfer resulting from placental insufficiency.
Objective: To identify predictors of poor perinatal outcome after maternal perception of reduced fetal movements (RFM).
Design: Prospective cohort study.
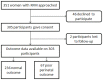
Methods: 305 women presenting with RFM after 28 weeks of gestation were recruited. Demographic factors and clinical history were recorded and ultrasound performed to assess fetal biometry, liquor volume and umbilical artery Doppler. A maternal serum sample was obtained for measurement of placentally-derived or modified proteins including: alpha fetoprotein (AFP), human chorionic gonadotrophin (hCG), human placental lactogen (hPL), ischaemia-modified albumin (IMA), pregnancy associated plasma protein A (PAPP-A) and progesterone. Factors related to poor perinatal outcome were determined by logistic regression.
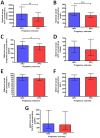
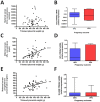
Results: 22.1% of pregnancies ended in a poor perinatal outcome after RFM. The most common complication was small-for-gestational age infants. Pregnancy outcome after maternal perception of RFM was related to amount of fetal activity while being monitored, abnormal fetal heart rate trace, diastolic blood pressure, estimated fetal weight, liquor volume, serum hCG and hPL. Following multiple logistic regression abnormal fetal heart rate trace (Odds ratio 7.08, 95% Confidence Interval 1.31-38.18), (OR) diastolic blood pressure (OR 1.04 (95% CI 1.01-1.09), estimated fetal weight centile (OR 0.95, 95% CI 0.94-0.97) and log maternal serum hPL (OR 0.13, 95% CI 0.02-0.99) were independently related to pregnancy outcome. hPL was related to placental mass.
Conclusion: Poor perinatal outcome after maternal perception of RFM is closely related to factors which are connected to placental dysfunction. Novel tests of placental function and associated fetal response may provide improved means to detect fetuses at greatest risk of poor perinatal outcome after RFM.
Conflict of interest statement
Figures
References
-
- Cousens S, Blencowe H, Stanton C, Chou D, Ahmed S, et al. National, regional, and worldwide estimates of stillbirth rates in 2009 with trends since 1995: a systematic analysis. Lancet. 2011;377:1319–1330. - PubMed
-
- Froen JF. A kick from within–fetal movement counting and the cancelled progress in antenatal care. J Perinat Med. 2004;32:13–24. - PubMed
-
- Sadovsky E, Yaffe H. Daily fetal movement recording and fetal prognosis. Obstet Gynecol. 1973;41:845–850. - PubMed
-
- Stacey T, Thompson JM, Mitchell EA, Ekeroma A, Zuccollo J, et al. Maternal Perception of Fetal Activity and Late Stillbirth Risk: Findings from the Auckland Stillbirth Study. Birth. 2011;38:311–316. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

