Risk factors of brain metastases in completely resected pathological stage IIIA-N2 non-small cell lung cancer
- PMID: 22846375
- PMCID: PMC3430600
- DOI: 10.1186/1748-717X-7-119
Risk factors of brain metastases in completely resected pathological stage IIIA-N2 non-small cell lung cancer
Abstract
Background: Brain metastases (BM) is one of the most common failures of locally advanced non-small cell lung cancer (LA-NSCLC) after combined-modality therapy. The outcome of trials on prophylactic cranial irradiation (PCI) has prompted us to identify the highest-risk subset most likely to benefit from PCI. Focusing on patients with completely resected pathological stage IIIA-N2 (pIIIA-N2) NSCLC, we aimed to assess risk factors of BM and to define the highest-risk subset.
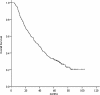
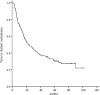
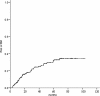
Methods: Between 2003 and 2005, the records of 217 consecutive patients with pIIIA-N2 NSCLC in our institution were reviewed. The cumulative incidence of BM was estimated using the Kaplan-Meier method, and differences between the groups were analyzed using log-rank test. Multivariate Cox regression analysis was applied to assess risk factors of BM.
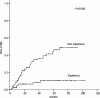
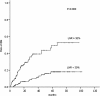
Results: Fifty-three (24.4 %) patients developed BM at some point during their clinical course. On multivariate analysis, non-squamous cell cancer (relative risk [RR]: 4.13, 95 % CI: 1.86-9.19; P = 0.001) and the ratio of metastatic to examined nodes or lymph node ratio (LNR) ≥ 30 % (RR: 3.33, 95 % CI: 1.79-6.18; P = 0.000) were found to be associated with an increased risk of BM. In patients with non-squamous cell cancer and LNR ≥ 30 %, the 5-year actuarial risk of BM was 57.3 %.
Conclusions: In NSCLC, patients with completely resected pIIIA-N2 non-squamous cell cancer and LNR ≥ 30 % are at the highest risk for BM, and are most likely to benefit from PCI. Further studies are warranted to investigate the effect of PCI on this subset of patients.
Figures



Similar articles
-
Risk factors for brain metastases in completely resected small cell lung cancer: a retrospective study to identify patients most likely to benefit from prophylactic cranial irradiation.Radiat Oncol. 2014 Sep 20;9:216. doi: 10.1186/1748-717X-9-216. Radiat Oncol. 2014. PMID: 25239373 Free PMC article.
-
Validation of pN2 sub-classifications in patients with pathological stage IIIA N2 non-small cell lung cancer.Interact Cardiovasc Thorac Surg. 2011 May;12(5):733-8. doi: 10.1510/icvts.2010.249896. Epub 2011 Feb 5. Interact Cardiovasc Thorac Surg. 2011. PMID: 21297135
-
Postoperative radiotherapy for patients with completely resected pathological stage IIIA-N2 non-small cell lung cancer: a preferential benefit for squamous cell carcinoma.Radiol Oncol. 2020 Dec 3;55(1):66-76. doi: 10.2478/raon-2020-0070. Radiol Oncol. 2020. PMID: 33885242 Free PMC article.
-
Risk factors for brain metastases in patients with non-small-cell lung cancer.Cancer Med. 2018 Dec;7(12):6357-6364. doi: 10.1002/cam4.1865. Epub 2018 Nov 8. Cancer Med. 2018. PMID: 30411543 Free PMC article. Review.
-
Treatment and toxic effects of prophylactic cranial irradiation in stage II-III non-small cell lung cancer: A meta-analysis.Asia Pac J Clin Oncol. 2021 Apr;17(2):e18-e26. doi: 10.1111/ajco.13359. Epub 2020 Aug 6. Asia Pac J Clin Oncol. 2021. PMID: 32761788 Review.
Cited by
-
Bevacizumab's Association With a Decreased Risk of Brain Metastases in ECOG-ACRIN E1505, a Phase 3 Randomized Trial of Adjuvant Chemotherapy With or Without Bevacizumab in Surgically Resected NSCLC.JTO Clin Res Rep. 2022 Jan 10;3(3):100274. doi: 10.1016/j.jtocrr.2021.100274. eCollection 2022 Mar. JTO Clin Res Rep. 2022. PMID: 35281954 Free PMC article.
-
Safety and efficacy of neoadjuvant cisplatin + S-1 combined with radiation therapy for locally advanced non-small cell lung cancer.Surg Today. 2025 Jul;55(7):886-899. doi: 10.1007/s00595-025-03019-9. Epub 2025 Feb 27. Surg Today. 2025. PMID: 40014076 Free PMC article.
-
The Positive Lymph Node Ratio Predicts Survival in T1-4N1-3M0 Non-Small Cell Lung Cancer: A Nomogram Using the SEER Database.Front Oncol. 2020 Aug 5;10:1356. doi: 10.3389/fonc.2020.01356. eCollection 2020. Front Oncol. 2020. PMID: 32903785 Free PMC article.
-
Natural history, clinical course and predictors of interval time from initial diagnosis to development of subsequent NSCLC brain metastases.J Neurooncol. 2019 May;143(1):145-155. doi: 10.1007/s11060-019-03149-4. Epub 2019 Mar 14. J Neurooncol. 2019. PMID: 30874953
-
Predictive value of metabolic parameters derived from preoperative 18F-FDG positron emission tomography/computed tomography for brain metastases in patients with surgically resected non-small cell lung cancer.Quant Imaging Med Surg. 2023 Dec 1;13(12):8545-8556. doi: 10.21037/qims-23-385. Epub 2023 Nov 22. Quant Imaging Med Surg. 2023. PMID: 38106281 Free PMC article.
References
-
- Sorensen JB, Hansen H, Hansen M, Dombernowsky P. Brain metastases in adenocarcinoma of the lung: frequency, risk groups, and prognosis. J Clin Oncol. 1988;6:1474–1480. - PubMed
-
- Komaki R, Scott CB, Sause WT, Johnson DH, Taylor SG. Induction cisplatin/vinblastine and irradiation vs. irradiation in unresectable squamous cell lung cancer: failure patterns by cell type in RTOG 88–08/ECOG 4588. Int J Radiat Oncol Biol Phys. 1997;39:537–544. doi: 10.1016/S0360-3016(97)00365-9. - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

