Randomized comparison of the i-gel™, the LMA Supreme™, and the Laryngeal Tube Suction-D using clinical and fibreoptic assessments in elective patients
- PMID: 22871204
- PMCID: PMC3434115
- DOI: 10.1186/1471-2253-12-18
Randomized comparison of the i-gel™, the LMA Supreme™, and the Laryngeal Tube Suction-D using clinical and fibreoptic assessments in elective patients
Abstract
Background: The i-gel™, LMA-Supreme (LMA-S) and Laryngeal Tube Suction-D (LTS-D) are single-use supraglottic airway devices with an inbuilt drainage channel. We compared them with regard to their position in situ as well as to clinical performance data during elective surgery.
Methods: Prospective, randomized, comparative study of three groups of 40 elective surgical patients each. Speed of insertion and success rates, leak pressures (LP) at different cuff pressures, dynamic airway compliance, and signs of postoperative airway morbidity were recorded. Fibreoptic evaluation was used to determine the devices' position in situ.
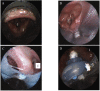
Results: Leak pressures were similar (i-gel™ 25.9, LMA-S 27.1, LTS-D 24.0 cmH2O; the latter two at 60 cmH2O cuff pressure) as were insertion times (i-gel™ 10, LMA-S 11, LTS-D 14 sec). LP of the LMA-S was higher than that of the LTS-D at lower cuff pressures (p <0.05). Insertion success rates differed significantly: i-gel™ 95%, LMA-S 95%, LTS-D 70% (p <0.05). The fibreoptically assessed position was more frequently suboptimal with the LTS-D but this was not associated with impaired ventilation. Dynamic airway compliance was highest with the i-gel™ and lowest with the LTS-D (p <0.05). Airway morbidity was more pronounced with the LTS-D (p <0.01).
Conclusion: All devices were suitable for ventilating the patients' lungs during elective surgery.
Trial registration: German Clinical Trial Register DRKS00000760.
Figures

Similar articles
-
Comparison of oropharyngeal leak pressure of air-Q™, i-gel™, and laryngeal mask airway supreme™ in adult patients during general anesthesia: A randomized controlled trial.Saudi J Anaesth. 2017 Oct-Dec;11(4):390-395. doi: 10.4103/sja.SJA_149_17. Saudi J Anaesth. 2017. PMID: 29033717 Free PMC article.
-
Randomized crossover study assessing oropharyngeal leak pressure and fiber optic positioning : Laryngeal Mask Airway Supreme™ versus Laryngeal Tube LTS II™ size 2 in non-paralyzed anesthetized children.Anaesthesist. 2016 Aug;65(8):585-9. doi: 10.1007/s00101-016-0192-1. Anaesthesist. 2016. PMID: 27380049 Clinical Trial. English.
-
Laryngeal mask airway protector generates higher oropharyngeal leak pressures compared to the laryngeal mask airway supreme: A randomized clinical trial in the ambulatory surgery unit.J Anaesthesiol Clin Pharmacol. 2021 Apr-Jun;37(2):221-225. doi: 10.4103/joacp.JOACP_416_19. Epub 2021 Jul 15. J Anaesthesiol Clin Pharmacol. 2021. PMID: 34349370 Free PMC article.
-
Brief review: The LMA Supreme™ supraglottic airway.Can J Anaesth. 2012 May;59(5):483-93. doi: 10.1007/s12630-012-9673-0. Epub 2012 Feb 9. Can J Anaesth. 2012. PMID: 22318376 Review.
-
Use of intubation introducers through a supraglottic airway to facilitate tracheal intubation: a brief review.Can J Anaesth. 2012 Jul;59(7):704-15. doi: 10.1007/s12630-012-9714-8. Epub 2012 Jun 1. Can J Anaesth. 2012. PMID: 22653838 Review.
Cited by
-
Feasibility of laryngeal mask anesthesia combined with nerve block in adult patients undergoing internal fixation of rib fractures: a prospective observational study.BMC Anesthesiol. 2020 Jul 15;20(1):170. doi: 10.1186/s12871-020-01082-y. BMC Anesthesiol. 2020. PMID: 32669087 Free PMC article.
-
Assessment of suitability of i-gel and laryngeal mask airway-supreme for controlled ventilation in anesthetized paralyzed patients: A prospective randomized trial.Anesth Essays Res. 2016 Jan-Apr;10(1):88-93. doi: 10.4103/0259-1162.167849. Anesth Essays Res. 2016. PMID: 26957697 Free PMC article.
-
Difficult Airway Society 2015 guidelines for management of unanticipated difficult intubation in adults.Br J Anaesth. 2015 Dec;115(6):827-48. doi: 10.1093/bja/aev371. Epub 2015 Nov 10. Br J Anaesth. 2015. PMID: 26556848 Free PMC article.
-
Comparison of I-gel for general anesthesia in obese and nonobese patients.Saudi J Anaesth. 2018 Oct-Dec;12(4):535-539. doi: 10.4103/sja.SJA_79_18. Saudi J Anaesth. 2018. PMID: 30429733 Free PMC article.
-
Prehospital airway management using the laryngeal tube. An emergency department point of view.Anaesthesist. 2014 Jul;63(7):589-96. doi: 10.1007/s00101-014-2348-1. Anaesthesist. 2014. PMID: 24981153
References
-
- Walsh EM. Time to dispose of nondisposable LMAs. Anesth Analg. 2005;100(3):896–897. author reply 897. - PubMed
-
- Thee C, Serocki G, Doerges V, Ilies C, Wallenius K, Bein B, Steinfath M, Cavus E. Laryngeal tube S II, laryngeal tube S disposable, Fastrach laryngeal mask and Fastrach laryngeal mask disposable during elective surgery: a randomized controlled comparison between reusable and disposable supraglottic airway devices. Eur J Anaesthesiol. 2007;27(5):468–472. - PubMed
LinkOut - more resources
Full Text Sources
Medical

