Effects of zero reference position on bladder pressure measurements: an observational study
- PMID: 22873414
- PMCID: PMC3390299
- DOI: 10.1186/2110-5820-2-S1-S13
Effects of zero reference position on bladder pressure measurements: an observational study
Abstract
Background: Although the World Society for Abdominal Compartment Syndrome in its guidelines recommends midaxillary line (MAL) as zero reference level in intra-abdominal pressure (IAP) measurements in aiming at standardizing the technique, evidence supporting this suggestion is scarce. The aim of this study is to study if the zero reference position influences bladder pressure measurements as estimate for IAP.
Methods: The IAP of 100 surgical patients was measured during the first 24 h of admission to the surgical intensive care unit of General Calixto Garcia Hospital in Havana (Cuba) following laparotomy. The period was January 2009 to January 2010. The IAP was measured twice with a six-hour interval using the transurethral technique with a priming volume of 25 ml. IAP was first measured with the zero reference level placed at MAL (IAPMAL), followed by a second measurement at the level of the symphysis pubis (SP) after 3 minutes (IAPSP). Correlations were made between IAP and body mass index (BMI), type of surgery, gender, and age.
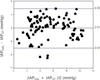
Results: Mean IAPMAL was 8.5 ± 2.8 mmHg vs. IAPSP 6.5 ± 2.8 mmHg (p < 0.0001). The bias between measurements was 2.0 ± 1.5, 95% confidence interval of 1.4 to 3.0, upper limit of 4.9, lower limit of -0.9, and a percentage error of 35.1%. IAPMAL was consistently higher than IAPSP regardless of the type of surgery. The BMI correlated with IAP values regardless of the zero reference level (R2 = 0.4 and 0.3 with IAPMAL and IAPSP respectively, p < 0.0001).
Conclusions: The zero reference level has an important impact on IAP measurement in surgical patients after laparotomy and can potentially lead to over or underestimation. Further anthropometric studies are needed with regard to the relative MAL and SP zero reference position in relation to the theoretical ideal reference level at midpoint of the abdomen. Until better evidence is available, MAL remains the recommended zero reference position due to its best anatomical localization at iliac crest.
Figures



References
-
- Soler C. Presión intra-abdominal¿ Parámetro útil? http://fcmfajardo.sld.cu/cev2002/conferencias/medicina_interna_caridad.htm (accessed 27 August 2011)
-
- Waele JJ, Cheatham ML, Malbrain MLNG, Kirkpatrick A, Sugrue M, Balogh Z, Ivatury R, De Keulenaer B, Kimball EJ. Recommendations for research from the International Conference of Experts on Intra-abdominal Hypertension and Abdominal Compartment Syndrome. Acta Clinica Belgica. 2009;64(3):203–209. - PubMed
-
- Malbrain M, Jones F. In: Abdominal compartment syndrome. Ivatury R, Cheatham M, Malbrain M, Sugrue M, editor. Georgetown: Landes Bioscience; 2006. Intra-abdominal pressure measurement techniques; pp. 19–68.
-
- Malbrain ML, Cheatham M, Kirkpatrick A, Sugrue M, Parr M, de Waele J, Balogh Z, Leppäniemi A, Olvera C, Ivatury R, D'Amours S, Wendon J, Hillman K, Johansson K, Kolkman K, Wilmer A. Results from the International Conference of Experts on Intra-abdominal Hypertension and Abdominal Compartment Syndrome. I Definitions. Intensive Care Med. 2006;32:1722–1732. doi: 10.1007/s00134-006-0349-5. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Research Materials

