Relaxation therapy for preventing and treating preterm labour
- PMID: 22895959
- PMCID: PMC11972839
- DOI: 10.1002/14651858.CD007426.pub2
Relaxation therapy for preventing and treating preterm labour
Abstract
Background: Preterm birth (PTB) is a leading cause of perinatal mortality and morbidity. Although the pathogenesis of preterm labour (PTL) is not well understood, there is evidence about the relationship between maternal psychological stress and adverse pregnancy outcomes. Relaxation or mind-body therapies cover a broad range of techniques, e.g. meditation, massage, etc. There is no systematic review investigating the effect of relaxation techniques on preventing PTL and PTB. This review does not cover hypnosis as this is the subject of a separate Cochrane review.
Objectives: To assess the effectiveness of relaxation therapies for preventing or treating PTL and preventing PTB.
Search methods: We searched the Cochrane Pregnancy and Childbirth Group's Trials Register (14 December 2011), CENTRAL (2011, Issue 4 of 4), CINAHL (1982 to 14 December 2011) and contacted study authors for additional information.
Selection criteria: Randomized controlled trials, cluster- and quasi-randomized trials comparing relaxation techniques with usual care, no treatment or sham interventions to prevent or treat PTL.
Data collection and analysis: Two review authors (B Khianman (BK) and P Pattanittum (PP)) independently assessed all search results for potential inclusion studies. Disagreements were resolved by discussion with a third review author (J Thinkhamrop (JT)). Data were independently extracted onto the standardized data collection form by BK and PP and checked for accuracy. Two review authors independently assessed the risk of bias of all included studies. All differences were resolved by discussion with JT. Mean difference (MD) and its 95% confidence intervals (CI) were calculated for continuous outcomes and risk ratio (RR) and 95% CI for dichotomous data.
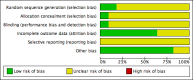
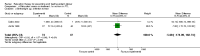
Main results: Eleven randomized controlled trials with a total of 833 women were included in this review. However, the results of this review are based on single studies with small numbers of participants.The majority of included studies reported insufficient information on sequence generation, allocation concealment as well as blinding. There were no included studies that assessed PTL or PTB as the primary outcome. The included studies were different in terms of intervention, practice, and time, and there were no clear coherent hypotheses.For women not in PTL, the benefits of relaxation was found in one study for maternal stress (Anxiety Stress Scale) at 26 to 29 weeks gestational age (mean difference (MD) -7.04; 95% confidence interval (CI) -13.91 to -0.17). In addition, there were some beneficial effects of relaxation including baby birthweight (MD 285.00 g; 95% CI 76.94 to 493.06); type of delivery; (vaginal delivery; risk ratio (RR) 1.52; 95% CI 1.13 to 2.04), (cesarean section; RR 0.38; 95% CI 0.19 to 0.78); maternal anxiety (MD -15.79; 95% CI -18.33 to -13.25); and stress (MD -13.08; 95% CI -15.29 to -10.87) when applying relaxation therapy together with standard treatment. For women in PTL, the results for the main outcome of PTB in the intervention and control groups from a single study were not different (RR 0.95; 95% CI 0.57 to 1.59). The MD of birthweight in grams from the fixed-effect model from two included studies was MD -5.68; (95% CI -174.09 to 162.74).
Authors' conclusions: According to the results of this review, there is some evidence that relaxation during pregnancy reduces stress and anxiety. However, there was no effect on PTL/PTB. These results should be interpreted with caution as they were drawn from included studies with limited quality.
Conflict of interest statement
None known.
Figures



















Update of
- doi: 10.1002/14651858.CD007426
Similar articles
-
Relaxation techniques for pain management in labour.Cochrane Database Syst Rev. 2018 Mar 28;3(3):CD009514. doi: 10.1002/14651858.CD009514.pub2. Cochrane Database Syst Rev. 2018. PMID: 29589650 Free PMC article.
-
Hypnosis for pain management during labour and childbirth.Cochrane Database Syst Rev. 2016 May 19;2016(5):CD009356. doi: 10.1002/14651858.CD009356.pub3. Cochrane Database Syst Rev. 2016. PMID: 27192949 Free PMC article.
-
Techniques of monitoring blood glucose during pregnancy for women with pre-existing diabetes.Cochrane Database Syst Rev. 2017 Jun 11;6(6):CD009613. doi: 10.1002/14651858.CD009613.pub3. Cochrane Database Syst Rev. 2017. Update in: Cochrane Database Syst Rev. 2019 May 23;5:CD009613. doi: 10.1002/14651858.CD009613.pub4. PMID: 28602020 Free PMC article. Updated.
-
Acupuncture or acupressure for induction of labour.Cochrane Database Syst Rev. 2017 Oct 17;10(10):CD002962. doi: 10.1002/14651858.CD002962.pub4. Cochrane Database Syst Rev. 2017. PMID: 29036756 Free PMC article.
-
Planned early delivery versus expectant management for hypertensive disorders from 34 weeks gestation to term.Cochrane Database Syst Rev. 2017 Jan 15;1(1):CD009273. doi: 10.1002/14651858.CD009273.pub2. Cochrane Database Syst Rev. 2017. PMID: 28106904 Free PMC article.
Cited by
-
Efficacy of advice from healthcare professionals to pregnant women on avoiding constrictive clothing around the trunk: a study protocol for a randomised controlled trial.BMJ Open. 2015 Sep 30;5(9):e008252. doi: 10.1136/bmjopen-2015-008252. BMJ Open. 2015. PMID: 26423851 Free PMC article. Clinical Trial.
-
Is maternal trait anxiety a risk factor for late preterm and early term deliveries?BMC Pregnancy Childbirth. 2016 Sep 29;16(1):286. doi: 10.1186/s12884-016-1070-1. BMC Pregnancy Childbirth. 2016. PMID: 27680098 Free PMC article.
-
Evaluation of a birth preparation program on lumbopelvic pain, urinary incontinence, anxiety and exercise: a randomized controlled trial.BMC Pregnancy Childbirth. 2013 Jul 29;13:154. doi: 10.1186/1471-2393-13-154. BMC Pregnancy Childbirth. 2013. PMID: 23895188 Free PMC article. Clinical Trial.
-
The Influence of Forest Activities in a University Campus Forest on Student's Psychological Effects.Int J Environ Res Public Health. 2021 Mar 2;18(5):2457. doi: 10.3390/ijerph18052457. Int J Environ Res Public Health. 2021. PMID: 33801534 Free PMC article.
-
Sleep facilitators and barriers in gestational diabetes mellitus: a qualitative study.BMC Pregnancy Childbirth. 2025 Apr 30;25(1):521. doi: 10.1186/s12884-025-07652-7. BMC Pregnancy Childbirth. 2025. PMID: 40307810 Free PMC article.
References
References to studies included in this review
Bahadoran 2010 {published data only}
Bastani 2006 {published data only}
-
- Bastani F, Hidarnia A, Kazemnejad A, Vafaei M, Kashanian M. A randomized controlled trial of the effects of applied relaxation training on reducing anxiety and perceived stress in pregnant women. Journal of Midwifery & Women's Health 2005;50(4):e36‐e40. - PubMed
-
- Bastani F, Hidarnia A, Montgomery KS, Aguilar‐Vafaei ME, Kazemnejad A. Does relaxation education in anxious primigravid Iranian women influence adverse pregnancy outcomes?: a randomized controlled trial. Journal of Perinatal & Neonatal Nursing 2006;20(2):138‐46. - PubMed
Casko 2002 {published data only}
-
- Casko RB. An analysis of the effectiveness of relaxation training for preterm labor and of interactions between relaxation exercises, state and trait anxiety, and desire for control in women with preterm labor [thesis]. Iowa: University of Iowa, 2002.
Chambers 2007 {published data only}
-
- Chambers AS. Relaxation during pregnancy to reduce stress and anxiety and their associated complications [thesis]. Arizona, USA: University of Arizona, 2007.
Dasari 2007 {published data only}
-
- Dasari P, Kodenchery MM. Psychological factors in preterm labor and psychotherapeutic intervention. International Journal of Gynecology & Obstetrics 2007;97(3):196‐7. - PubMed
Field 2004 {published data only}
-
- Field T, Diego MA, Hernandez‐Reif M, Schanberg S, Kuhn C. Massage therapy effects on depressed pregnant women. Journal of Psychosomatic Obstetrics and Gynaecology 2004;25(2):115‐22. - PubMed
Gijsbers 1990 {published data only}
-
- Gijsbers Van Wijk CMT, Geus JAC, Schutte MF, Wildschut HIJ, Zuuren FJ. Symptom perception during treatment of preterm labor: an experimental approach to measure the benefits of psychological intervention. Journal of Psychosomatic Obstetrics and Gynaecology 1990;11:185‐96.
Jallo 2007 {published data only}
-
- Jallo NL. The effects of relaxation‐guided imagery on maternal stress [thesis]. Virginia: University of Virginia, 2007.
Janke 1999 {published data only}
-
- Janke J. The effect of relaxation therapy on preterm labor outcomes. Journal of Obstetric, Gynecologic, and Neonatal Nursing 1999;28(3):255‐63. - PubMed
Satyapriya 2009 {published data only}
-
- Satyapriya M, Nagendra HR, Nagarathna R, Padmalatha V. Effect of integrated yoga on stress and heart rate variability in pregnant women. International Journal of Gynecology & Obstetrics 2009;104(3):218‐22. - PubMed
Yang 2009 {published data only}
-
- Yang M, Li L, Zhu H, Alexander IM, Liu S, Zhou W, et al. Music therapy to relieve anxiety in pregnant women on bedrest: a randomized, controlled trial. MCN, American Journal of Maternal Child Nursing 2009;34(5):316‐23. - PubMed
References to studies excluded from this review
Brown 1999 {published data only}
-
- Brown DC, Murphy M. Medical hypnosis in preterm labor: a randomized clinical trial. Report of two pilot projects. Hypnos 1999;26(2):77‐87.
Feinstein 2000 {published data only}
-
- Feinstein N. Maternal coping with preterm labor: an intervention [thesis]. Rochester, New York: University of Rochester, 2000.
Omer 1986 {published data only}
-
- Omer H, Friedlander D, Palti Z. Hypnotic relaxation in the treatment of premature labor. Psychosomatic Medicine 1986;48(5):351‐61. - PubMed
References to studies awaiting assessment
Bauer 2010 {published data only}
-
- Bauer CL, Victorson D, Rosenbloom S, Barocas J, Silver RK. Alleviating distress during antepartum hospitalization: a randomized controlled trial of music and recreation therapy. Journal of Women's Health 2010;19(3):523‐31. - PubMed
Urech 2010 {published data only}
-
- Urech C, Alder J, Bitzer J, Hosli I. The effect of relaxation exercises on psychological wellbeing during pregnancy [Entspannungs‐Ubungen wahrend der Schwangerschaft: Der Einfluss auf das psychobiologische Wohlbefinden]. Geburtshilfe und Frauenheilkunde 2009;69:163.
-
- Urech C, Fink NS, Wilhelm FH, Bitzer J, Alder J. Effects of relaxation on psychobiological wellbeing during pregnancy: a randomized controlled trial. Psychoneuroendocrinology 2010;35:1348‐55. - PubMed
Yu 2010 {published data only}
-
- Yu WJ, Song JE. Effects of abdominal breathing on state anxiety, stress, and tocolytic dosage for pregnant women in preterm labor. Journal of Korean Academy of Nursing 2010;40(3):442‐52. - PubMed
Additional references
Astin 2003
-
- Astin JA, Shapiro SL, Eisenberg DM, Forys KL. Mind‐body medicine: state of the science, implications for practice. Journal of the American Board of Family Practice 2003;16:131‐47. - PubMed
Burke 2000
-
- Burke C, Morrison JJ. Perinatal factors and preterm delivery in an Irish obstetric population. Journal of Perinatal Medicine 2000;28:49‐53. - PubMed
Chung 2001
-
- Chung TKH, Lau TK, Yip ASK, Chiu HFK, Lee DTS. Antepartum depressive symptomatology is associated with adverse obstetric and neonatal outcomes. Psychosomatic Medicine 2001;63:830‐4. - PubMed
Davis 1998
-
- Davis M, Eshelman ER, McKay M. The relaxation & stress reduction workbook. Oakland: New Harbinger Publication Inc, 1998.
Egger 1997
Harbord 2006
-
- Harbord RM, Egger M, Sterne JA. A modified test for small‐study effects in meta‐analyses of controlled trials with binary endpoints. Statistics in Medicine 2006;25(20):3443‐57. - PubMed
Higgins 2011
-
- Higgins JPT, Green S, editors. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [updated March 2011]. The Cochrane Collaboration, 2011. Available from www.cochrane‐handbook.org.
Kiss 2004
RevMan 2011 [Computer program]
-
- The Nordic Cochrane Centre, The Cochrane Collaboration. Review Manager (RevMan). Version 5.1. Copenhagen: The Nordic Cochrane Centre, The Cochrane Collaboration, 2011.
Rondo 2003
-
- Rondo PHC, Ferreira RF, Nogueira F, Ribeiro MCN, Lobert H, Artes R. Maternal psychological stress and distress as predictors of low birth weight, prematurity and intrauterine growth retardation. European Journal of Clinical Nutrition 2003;57:266‐72. - PubMed
Steer 2006
-
- Steer PJ. The epidemiology of preterm labour ‐ why have advances not equated to reduced incidence?. BJOG: an international journal of obstetrics and gynaecology 2006;113(Suppl 3):1‐3. - PubMed
Von Der Pool 1998
-
- Pool BA. Preterm labor: diagnosis and treatment. American Family Physician 1998;57(10):2457‐64. - PubMed
Weismiller 1999
-
- Weismiller DG. Preterm labor. American Family Physician 1999;59(3):593‐602. - PubMed
Witter 1993
-
- Witter FR, Keith LG. Textbook of Prematurity: Antecedents, Treatment and Outcome. Boston: Little, Brown and Company, 1993.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

