Autoimmune diseases and venous thromboembolism: a review of the literature
- PMID: 22937487
- PMCID: PMC3427982
Autoimmune diseases and venous thromboembolism: a review of the literature
Abstract
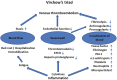
Venous thromboembolism (VTE) is major health problem and is sometimes complicated by lethal pulmonary embolism (PE). Disturbances of the coagulation and anticoagulation systems are important risk factors for VTE. Comparative studies suggest that coagulation and innate immunity have a shared evolutionary origin. It is therefore unsurprising that the immune and coagulation systems are linked, with many molecular components being important for both systems. Systemic inflammation modulates thrombotic responses by suppressing fibrinolysis, upregulating procoagulant, and downregulating anticoagulants, and autoimmune disorders such as systemic lupus erythematosus (SLE), inflammatory bowel disease (IBD), and Behçet's syndrome have been linked to an increased risk of VTE. Recent reports have further shown that a majority of autoimmune and immune-mediated disorders are linked to an increased risk of venous thrombosis, PE, or VTE. For instance, a Swedish nationwide study found that the risk of PE was increased in the first year after hospitalization for 33 different autoimmune disorders. Especially high risks were noted for several autoimmune diseases such as immune thrombocytopenic purpura, polyarteritis nodosa, polymyositis/dermatomyositis, ulcerative colitis, and SLE. Another study from England, also based on hospitalization data, found that immune-mediated disorders were associated with an increased risk of VTE compared with other medical causes of hospitalization. Multiple mechanisms may operate and disease-specific factors, such as cardiolipin antibodies, have been identified. However, inflammation by itself appears to change the hemostatic balance in a thrombogenic direction. Recent epidemiological studies, together with previous experimental and clinical studies, indicate that autoimmune disorders should not only be viewed as inflammatory disorders, but also hypercoagulable disorders. Research to identify thrombotic risk factors, elucidate the mechanisms involved, and investigate prophylactic regiments is needed. The present review describes the epidemiological, clinical, and experimental evidence for the connection between VTE and autoimmune and immune-mediated disorders.
Keywords: Autoimmune diseases; blood coagulation disorders; immunology; inflammation; inflammatory bowel diseases; pulmonary embolism; rheumatic diseases; venous thromboembolism; venous thrombosis.
Figures
References
-
- Heit JA, Silverstein MD, Mohr DN, Petterson TM, Lohse CM, O’Fallon WM, Melton LJ 3rd. The epidemiology of venous thromboembolism in the community. Thromb Haemost. 2001;86:452–463. - PubMed
-
- White R. The Epidemiology of venous thromboembolism. Circulation. 2003;107:I4–I8. - PubMed
-
- Goldhaber SZ, Visani L, De Rosa M. Acute pulmonary embolism: clinical outcomes in the International Cooperative Pulmonary Embolism Registry (ICOPER) Lancet. 1999;353:1386–1389. - PubMed
-
- Goldhaber SZ, Elliott CG. Acute pulmonary embolism: part I: epidemiology, pathophysiology, and diagnosis. Circulation. 2003;108:2726–2729. - PubMed
-
- Dahlbäck B. Advances in understanding pathogenic mechanisms of thrombophilic disorders. Blood. 2008;112:19–127. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical