Characterization of the transport topology in patient-specific abdominal aortic aneurysm models
- PMID: 22952409
- PMCID: PMC3427345
- DOI: 10.1063/1.4744984
Characterization of the transport topology in patient-specific abdominal aortic aneurysm models
Abstract
Abdominal aortic aneurysm (AAA) is characterized by disturbed blood flow patterns that are hypothesized to contribute to disease progression. The transport topology in six patient-specific abdominal aortic aneurysms was studied. Velocity data were obtained by image-based computational fluid dynamics modeling, with magnetic resonance imaging providing the necessary simulation parameters. Finite-time Lyapunov exponent (FTLE) fields were computed from the velocity data, and used to identify Lagrangian coherent structures (LCS). The combination of FTLE fields and LCS was used to characterize topological flow features such as separation zones, vortex transport, mixing regions, and flow impingement. These measures offer a novel perspective into AAA flow. It was observed that all aneurysms exhibited coherent vortex formation at the proximal segment of the aneurysm. The evolution of the systolic vortex strongly influences the flow topology in the aneurysm. It was difficult to predict the vortex dynamics from the aneurysm morphology, motivating the application of image-based flow modeling.
Figures











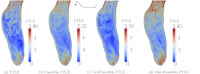
References
-
- Salsac A. V., Sparks S. R., Chomaz J. M., and Lasheras J. C., “Evolution of the wall shear stresses during the progressive enlargement of symmetric abdominal aortic aneurysms,” J. Fluid Mech. 560, 19–52 (2006). 10.1017/S002211200600036X - DOI
-
- Suh G. Y., Les A. S., Tenforde A. S., Shadden S. C., Spilker R. L., Yeung J. J., Cheng C. P., Herfkens R. J., Dalman R. L., and Taylor C. A., “Quantification of particle residence time in abdominal aortic aneurysms using magnetic resonance imaging and computational fluid dynamics,” Ann. Biomed. Eng. 39, 864–883 (2011). 10.1007/s10439-010-0202-4 - DOI - PMC - PubMed
-
- Les A. S., Shadden S. C., Figueroa C. A., Park J. M., Tedesco M. M., Herfkens R. J., Dalman R. L., and Taylor C. A., “Quantification of hemodynamics in abdominal aortic aneurysms during rest and exercise using magnetic resonance imaging and computational fluid dynamics,” Ann. Biomed. Eng. 38, 1288–1313 (2010). 10.1007/s10439-010-9949-x - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources
