Declining liver utilization for transplantation in the United States and the impact of donation after cardiac death
- PMID: 22965893
- PMCID: PMC3535500
- DOI: 10.1002/lt.23547
Declining liver utilization for transplantation in the United States and the impact of donation after cardiac death
Abstract
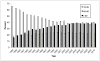
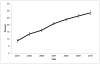
Worsening donor liver quality resulting in decreased organ utilization may be contributing to the recent decline in liver transplants nationally. We sought to examine trends in donor liver utilization and the relationship between donor characteristics and nonuse. We used the United Network for Organ Sharing database to review all deceased adult organ donors in the United States from whom at least 1 solid organ was transplanted into a recipient. Trends in donor characteristics were examined. Multivariate logistic regression was used to evaluate the association between donor characteristics and liver nonuse between 2004 and 2010. Population attributable risk proportions were determined for donor factors associated with nonuse. We analyzed 107,259 organ donors. The number of unused livers decreased steadily from 1958 (66% of donors) in 1988 to 841 (15%) in 2004 but then gradually increased to 1345 (21%) in 2010. The donor age, the body mass index (BMI), and the prevalence of diabetes and donation after cardiac death (DCD) all increased over time, and all 4 factors were independently associated with liver nonuse. DCD had the highest adjusted odds ratio (OR) for nonuse, and the odds increased nearly 4-fold between 2004 [OR = 5.53, 95% confidence interval (CI) = 4.57-6.70] and 2010 (OR = 21.31, 95% CI = 18.30-24.81). The proportion of nonuse attributable to DCD increased from 9% in 2004 to 28% in 2010. In conclusion, the proportion of donor livers not used has increased since 2004. Older donor age, greater BMI, diabetes, and DCD are all independently associated with nonuse and are on the rise nationally. Current trends may lead to significant declines in liver transplant availability.
Copyright © 2012 American Association for the Study of Liver Diseases.
Conflict of interest statement
Figures





Comment in
-
Donation after cardiac death liver transplantation: another fly in the ointment.Liver Transpl. 2013 Jan;19(1):1-2. doi: 10.1002/lt.23563. Liver Transpl. 2013. PMID: 23124996 No abstract available.
References
-
- Spitzer AL, Lao OB, Dick AA, Bakthavatsalam R, Halldorson JB, Yeh MM, et al. The biopsied donor liver: incorporating macrosteatosis into high-risk donor assessment. Liver Transpl. 2010;16(7):874–84. - PubMed
-
- McCormack L, Petrowsky H, Jochum W, Mullhaupt B, Weber M, Clavien PA. Use of severely steatotic grafts in liver transplantation: a matched case-control study. Ann Surg. 2007;246(6):940–6. discussion 6–8. - PubMed
-
- Feng S, Goodrich NP, Bragg-Gresham JL, Dykstra DM, Punch JD, DebRoy MA, et al. Characteristics associated with liver graft failure: the concept of a donor risk index. Am J Transplant. 2006;6(4):783–90. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
