Self-reported barriers to colorectal cancer screening in a racially diverse, low-income study population
- PMID: 22976770
- PMCID: PMC3560309
- DOI: 10.1007/s10900-012-9612-6
Self-reported barriers to colorectal cancer screening in a racially diverse, low-income study population
Abstract
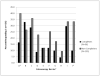
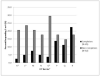
Colorectal cancer (CRC) screening is underutilized, especially in low income, high minority populations. We examined the effect test-specific barriers have on colonoscopy and fecal immunochemical test (FIT) completion, what rationales are given for non-completion, and what "switch" patterns exist when participants are allowed to switch from one test to another. Low income adults who were not up-to-date with CRC screening guidelines were recruited from safety-net clinics and offered colonoscopy or FIT (n = 418). Follow up telephone surveys assessed test-specific barriers. Test completion was determined from patient medical records. For subjects who desired colonoscopy at baseline, finding a time to come in and transportation applied more to non-completers than completers (p = 0.001 and p < 0.001, respectively). For participants who initially wanted FIT, keeping track of cards, never putting stool on cards, and not remembering to mail cards back applied more to non-completers than completers (p = 0.003, p = 0.006, and p < 0.001, respectively). The most common rationale given for not completing screening was a desire for the other screening modality: 7 % of patients who initially preferred screening by FIT completed colonoscopy, while 8 % of patients who initially preferred screening by colonoscopy completed FIT. We conclude that test-specific barriers apply more to subjects who did not complete CRC screening. As a common rationale for test non-completion is a desire to receive a different screening modality, our findings suggest screening rates could be increased by giving patients the opportunity to switch tests after an initial choice is made.
Figures
Similar articles
-
Outreach invitations for FIT and colonoscopy improve colorectal cancer screening rates: A randomized controlled trial in a safety-net health system.Cancer. 2016 Feb 1;122(3):456-63. doi: 10.1002/cncr.29770. Epub 2015 Nov 4. Cancer. 2016. PMID: 26535565 Free PMC article. Clinical Trial.
-
Patient-Reported Barriers to Completing a Diagnostic Colonoscopy Following Abnormal Fecal Immunochemical Test Among Uninsured Patients.J Gen Intern Med. 2019 Sep;34(9):1730-1736. doi: 10.1007/s11606-019-05117-0. Epub 2019 Jun 21. J Gen Intern Med. 2019. PMID: 31228053 Free PMC article.
-
Effect of Colonoscopy Outreach vs Fecal Immunochemical Test Outreach on Colorectal Cancer Screening Completion: A Randomized Clinical Trial.JAMA. 2017 Sep 5;318(9):806-815. doi: 10.1001/jama.2017.11389. JAMA. 2017. PMID: 28873161 Free PMC article. Clinical Trial.
-
Barriers and Facilitators to Timely Colonoscopy Completion for Safety Net Clinic Patients.Am J Health Behav. 2020 Jul 1;44(4):460-472. doi: 10.5993/AJHB.44.4.8. Am J Health Behav. 2020. PMID: 32553027
-
Colorectal Cancer Screening: Recommendations for Physicians and Patients from the U.S. Multi-Society Task Force on Colorectal Cancer.Am J Gastroenterol. 2017 Jul;112(7):1016-1030. doi: 10.1038/ajg.2017.174. Epub 2017 Jun 6. Am J Gastroenterol. 2017. PMID: 28555630 Review.
Cited by
-
Alaska Native Patient and Provider Perspectives on the Multitarget Stool DNA Test Compared With Colonoscopy for Colorectal Cancer Screening.J Prim Care Community Health. 2019 Jan-Dec;10:2150132719884295. doi: 10.1177/2150132719884295. J Prim Care Community Health. 2019. PMID: 31646933 Free PMC article.
-
Utilization of Colorectal Cancer Screening among Saudi Elderly Population: A Study from the Saudi National Survey for Elderly Health.Asian Pac J Cancer Prev. 2018 Dec 25;19(12):3401-3407. doi: 10.31557/APJCP.2018.19.12.3401. Asian Pac J Cancer Prev. 2018. PMID: 30583346 Free PMC article.
-
Determinants of variations in self-reported barriers to colonoscopy among uninsured patients in a primary care setting.J Community Health. 2015 Apr;40(2):260-70. doi: 10.1007/s10900-014-9925-8. J Community Health. 2015. PMID: 25096763
-
Follow-up colonoscopy after an abnormal stool-based colorectal cancer screening result: analysis of steps in the colonoscopy completion process.BMC Gastroenterol. 2021 Sep 28;21(1):356. doi: 10.1186/s12876-021-01923-1. BMC Gastroenterol. 2021. PMID: 34583638 Free PMC article.
-
Decisional stage distribution for colorectal cancer screening among diverse, low-income study participants.Health Educ Res. 2015 Jun;30(3):400-11. doi: 10.1093/her/cyv006. Epub 2015 Feb 25. Health Educ Res. 2015. PMID: 25721254 Free PMC article.
References
-
- Altekruse SF, Kosary CL, Krapcho M, et al. SEER Cancer Statistics Review, 1975-2007. National Cancer Institute; Bethesda, MD: 2010. http://seer.cancer.gov/csr/1975_2007/, based on November 2009 SEER data submission, posted to the SEER web site.
-
- Sonnenberg A, Delcò F, Inadomi JM. Cost-effectiveness of colonoscopy in screening for colorectal cancer. Annals of Internal Medicine. 2000;133(8):573–584. - PubMed
-
- Pignone M, Saha S, Hoerger T, Mandelblatt J. Cost-effectiveness analyses of colorectal cancer screening. Annals of Internal Medicine. 2002;137(2):96–104. - PubMed
-
- Calonge N, Petitti DB, DeWitt TG, et al. Screening for Colorectal Cancer: U.S. Preventive Services Task Force Recommendation Statement. Annals of Internal Medicine. 2008;149(9):627–637. - PubMed
-
- Levin B, Lieberman DA, McFarland B, et al. Screening and surveillance for the early detection of colorectal cancer and adenomatous polyps, 2008: a joint guideline from the American Cancer Society, the US Multi-Society Task Force on Colorectal Cancer, and the American College of Radiology. Gastroenterology. 2008;134(5):1570–1595. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

