Increased cortical porosity in type 2 diabetic postmenopausal women with fragility fractures
- PMID: 22991256
- PMCID: PMC3534818
- DOI: 10.1002/jbmr.1763
Increased cortical porosity in type 2 diabetic postmenopausal women with fragility fractures
Abstract
The primary goal of this study was to assess peripheral bone microarchitecture and strength in postmenopausal women with type 2 diabetes with fragility fractures (DMFx) and to compare them with postmenopausal women with type 2 diabetics without fractures (DM). Secondary goals were to assess differences in nondiabetic postmenopausal women with fragility fractures (Fx) and nondiabetic postmenopausal women without fragility fractures (Co), and in DM and Co women. Eighty women (mean age 61.3 ± 5.7 years) were recruited into these four groups (DMFx, DM, Fx, and Co; n = 20 per group). Participants underwent dual-energy X-ray absorptiometry (DXA) and high-resolution peripheral quantitative computed tomography (HR-pQCT) of the ultradistal and distal radius and tibia. In the HR-pQCT images volumetric bone mineral density and cortical and trabecular structure measures, including cortical porosity, were calculated. Bone strength was estimated using micro-finite element analysis (µFEA). Differential strength estimates were obtained with and without open cortical pores. At the ultradistal and distal tibia, DMFx had greater intracortical pore volume (+52.6%, p = 0.009; +95.4%, p = 0.020), relative porosity (+58.1%, p = 0.005; +87.9%, p = 0.011) and endocortical bone surface (+10.9%, p = 0.031; +11.5%, p = 0.019) than DM. At the distal radius DMFx had 4.7-fold greater relative porosity (p < 0.0001) than DM. At the ultradistal radius, intracortical pore volume was significantly higher in DMFx than DM (+67.8%, p = 0.018). DMFx also displayed larger trabecular heterogeneity (ultradistal radius: +36.8%, p = 0.035), and lower total and cortical BMD (ultradistal tibia: -12.6%, p = 0.031; -6.8%, p = 0.011) than DM. DMFx exhibited significantly higher pore-related deficits in stiffness, failure load, and cortical load fraction at the ultradistal and distal tibia, and the distal radius than DM. Comparing nondiabetic Fx and Co, we only found a nonsignificant trend with increase in pore volume (+38.9%, p = 0.060) at the ultradistal radius. The results of our study suggest that severe deficits in cortical bone quality are responsible for fragility fractures in postmenopausal diabetic women.
Copyright © 2013 American Society for Bone and Mineral Research.
Figures

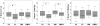


References
-
- Schwartz AV, Sellmeyer DE, Ensrud KE, Cauley JA, Tabor HK, Schreiner PJ, Jamal SA, Black DM, Cummings SR. Older women with diabetes have an increased risk of fracture: a prospective study. The Journal of clinical endocrinology and metabolism. 2001;86(1):32–38. - PubMed
-
- Janghorbani M, Van Dam RM, Willett WC, Hu FB. Systematic review of type 1 and type 2 diabetes mellitus and risk of fracture. American journal of epidemiology. 2007;166(5):495–505. - PubMed
-
- de L, II, van der Klift M, de Laet CE, van Daele PL, Hofman A, Pols HA. Bone mineral density and fracture risk in type-2 diabetes mellitus: the Rotterdam Study. Osteoporosis international : a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA. 2005;16(12):1713–1720. - PubMed
-
- Vestergaard P. Discrepancies in bone mineral density and fracture risk in patients with type 1 and type 2 diabetes--a meta-analysis. Osteoporosis international : a journal established as result of cooperation between the European Foundation for Osteoporosis and the National Osteoporosis Foundation of the USA. 2007;18(4):427–444. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

