Antibiotic exposure and IBD development among children: a population-based cohort study
- PMID: 23008454
- PMCID: PMC4074626
- DOI: 10.1542/peds.2011-3886
Antibiotic exposure and IBD development among children: a population-based cohort study
Abstract
Objective: To determine whether childhood antianaerobic antibiotic exposure is associated with the development of inflammatory bowel disease (IBD).
Methods: This retrospective cohort study employed data from 464 UK ambulatory practices participating in The Health Improvement Network. All children with ≥ 2 years of follow-up from 1994 to 2009 were followed between practice enrollment and IBD development, practice deregistration, 19 years of age, or death; those with previous IBD were excluded. All antibiotic prescriptions were captured. Antianaerobic antibiotic agents were defined as penicillin, amoxicillin, ampicillin, penicillin/β-lactamase inhibitor combinations, tetracyclines, clindamycin, metronidazole, cefoxitin, carbapenems, and oral vancomycin.
Results: A total of 1072426 subjects contributed 6.6 million person-years of follow-up; 748 developed IBD. IBD incidence rates among antianaerobic antibiotic unexposed and exposed subjects were 0.83 and 1.52/10000 person-years, respectively, for an 84% relative risk increase. Exposure throughout childhood was associated with developing IBD, but this relationship decreased with increasing age at exposure. Exposure before 1 year of age had an adjusted hazard ratio of 5.51 (95% confidence interval [CI]: 1.66-18.28) but decreased to 2.62 (95% CI: 1.61-4.25) and 1.57 (95% CI: 1.35-1.84) by 5 and 15 years, respectively. Each antibiotic course increased the IBD hazard by 6% (4%-8%). A dose-response effect existed, with receipt of >2 antibiotic courses more highly associated with IBD development than receipt of 1 to 2 courses, with adjusted hazard ratios of 4.77 (95% CI: 2.13-10.68) versus 3.33 (95% CI: 1.69-6.58).
Conclusions: Childhood antianaerobic antibiotic exposure is associated with IBD development.
Figures
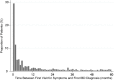


Comment in
-
Antibiotic exposure is associated with development of inflammatory bowel disease.J Pediatr. 2013 May;162(5):1077. doi: 10.1016/j.jpeds.2013.02.045. J Pediatr. 2013. PMID: 23617975 No abstract available.
References
-
- Malaty HM, Fan X, Opekun AR, Thibodeaux C, Ferry GD. Rising incidence of inflammatory bowel disease among children: a 12-year study. J Pediatr Gastroenterol Nutr. 2010;50(1):27–31 - PubMed
-
- Sartor RB. Microbial influences in inflammatory bowel diseases. Gastroenterology. 2008;134(2):577–594 - PubMed
-
- Gradel KO, Nielsen HL, Schønheyder HC, Ejlertsen T, Kristensen B, Nielsen H. Increased short- and long-term risk of inflammatory bowel disease after salmonella or campylobacter gastroenteritis. Gastroenterology. 2009;137(2):495–501 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

