Personal attributes that influence the adequate management of hypertension and dyslipidemia in patients with type 2 diabetes. Results from the DIAB-CORE Cooperation
- PMID: 23035799
- PMCID: PMC3503646
- DOI: 10.1186/1475-2840-11-120
Personal attributes that influence the adequate management of hypertension and dyslipidemia in patients with type 2 diabetes. Results from the DIAB-CORE Cooperation
Abstract
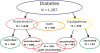
Background: Hypertension and dyslipidemia are often insufficiently controlled in persons with type 2 diabetes (T2D) in Germany. In the current study we evaluated individual characteristics that are assumed to influence the adequate treatment and control of hypertension and dyslipidemia and aimed to identify the patient group with the most urgent need for improved health care.
Methods: The analysis was based on the DIAB-CORE project in which cross-sectional data from five regional population-based studies and one nationwide German study, conducted between 1997 and 2006, were pooled. We compared the frequencies of socio-economic and lifestyle factors along with comorbidities in hypertensive participants with or without the blood pressure target of<140/90 mmHg. Similar studies were also performed in participants with dyslipidemia with and without the target of total cholesterol/HDL cholesterol ratio<5. Furthermore, we compared participants who received antihypertensive/lipid lowering treatment with those who were untreated. Univariable and multivariable logistic regression models were used to assess the odds of potentially influential factors.
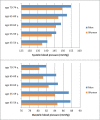
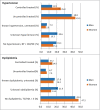
Results: We included 1287 participants with T2D of whom n=1048 had hypertension and n=636 had dyslipidemia. Uncontrolled blood pressure was associated with male sex, low body mass index (BMI), no history of myocardial infarction (MI) and study site. Uncontrolled blood lipid levels were associated with male sex, no history of MI and study site. The odds of receiving no pharmacotherapy for hypertension were significantly greater in men, younger participants, those with BMI<30 kg/m(2) and those without previous MI or stroke. Participants with dyslipidemia received lipid lowering medication less frequently if they were male and had not previously had an MI. The more recent studies HNR and CARLA had the greatest numbers of well controlled and treated participants.
Conclusion: In the DIAB-CORE study, the patient group with the greatest odds of uncontrolled co-morbidities and no pharmacotherapy was more likely comprised of younger men with low BMI and no history of cardiovascular disease.
Figures
Similar articles
-
Blood pressure and lipid management fall far short in persons with type 2 diabetes: results from the DIAB-CORE Consortium including six German population-based studies.Cardiovasc Diabetol. 2012 May 8;11:50. doi: 10.1186/1475-2840-11-50. Cardiovasc Diabetol. 2012. PMID: 22569118 Free PMC article.
-
Pharmacological management of modifiable cardiovascular risk factors (blood pressure and lipids) following diagnosis of myocardial infarction, stroke and diabetes: comparison between population-based studies in Russia and Norway.BMC Cardiovasc Disord. 2020 May 19;20(1):234. doi: 10.1186/s12872-020-01513-1. BMC Cardiovasc Disord. 2020. PMID: 32430002 Free PMC article.
-
Factors associated with therapeutic goal attainment in patients with concomitant hypertension and dyslipidemia.Hosp Pract (1995). 2014 Apr;42(2):77-88. doi: 10.3810/hp.2014.04.1106. Hosp Pract (1995). 2014. PMID: 24769787
-
Single Pill Regimen Leads to Better Adherence and Clinical Outcome in Daily Practice in Patients Suffering from Hypertension and/or Dyslipidemia: Results of a Meta-Analysis.High Blood Press Cardiovasc Prev. 2020 Apr;27(2):157-164. doi: 10.1007/s40292-020-00370-5. Epub 2020 Mar 26. High Blood Press Cardiovasc Prev. 2020. PMID: 32219670 Free PMC article. Review.
-
Beyond low-density lipoprotein: addressing the atherogenic lipid triad in type 2 diabetes mellitus and the metabolic syndrome.Am J Cardiovasc Drugs. 2005;5(6):379-87. doi: 10.2165/00129784-200505060-00005. Am J Cardiovasc Drugs. 2005. PMID: 16259526 Review.
Cited by
-
Potential contribution of lifestyle and socioeconomic factors to healthy user bias in antihypertensives and lipid-lowering drugs.Open Heart. 2017 Mar 9;4(1):e000417. doi: 10.1136/openhrt-2016-000417. eCollection 2017. Open Heart. 2017. PMID: 28761670 Free PMC article.
-
Evaluating Adherence to Concomitant Diabetes, Hypertension, and Hyperlipidemia Treatments and Cardiovascular Outcomes Among Elderly Patients Using Marginal Structural Modeling.High Blood Press Cardiovasc Prev. 2022 Nov;29(6):601-610. doi: 10.1007/s40292-022-00543-4. Epub 2022 Sep 24. High Blood Press Cardiovasc Prev. 2022. PMID: 36152232
-
Sex, Prescribing Practices and Guideline Recommended, Blood Pressure, and LDL Cholesterol Targets at Baseline in the BARI 2D Trial.Int J Endocrinol. 2015;2015:610239. doi: 10.1155/2015/610239. Epub 2015 Mar 19. Int J Endocrinol. 2015. PMID: 25873955 Free PMC article.
-
LEADER 5: prevalence and cardiometabolic impact of obesity in cardiovascular high-risk patients with type 2 diabetes mellitus: baseline global data from the LEADER trial.Cardiovasc Diabetol. 2016 Feb 10;15:29. doi: 10.1186/s12933-016-0341-5. Cardiovasc Diabetol. 2016. PMID: 26864124 Free PMC article. Clinical Trial.
-
Magnitude of, and Factors Associated with Cardiovascular Disease Among Type Two Diabetes Mellitus Patients.Diabetes Metab Syndr Obes. 2020 Nov 3;13:4123-4129. doi: 10.2147/DMSO.S254883. eCollection 2020. Diabetes Metab Syndr Obes. 2020. PMID: 33177852 Free PMC article.
References
-
- Berry J, Keebler ME, McGuire DK. Diabetes mellitus and cardiovascular disease. Pandora's box has been opened. Herz. 2004;29:456–462. - PubMed
-
- Mancia G. The association of hypertension and diabetes: prevalence, cardiovascular risk and protection by blood pressure reduction. Acta Diabetol. 2005;42(Suppl 1):S17–S25. - PubMed
-
- Scott R, Donoghoe M, Watts GF, O'Brien R, Pardy C, Taskinen MR, Davis TM, Colman PG, Manning P, Fulcher G, Keech AC. Impact of metabolic syndrome and its components on cardiovascular disease event rates in 4900 patients with type 2 diabetes assigned to placebo in the FIELD randomised trial. Cardiovasc Diabetol. 2011;10:102. doi: 10.1186/1475-2840-10-102. - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

