A study of respiration-correlated cone-beam CT scans to correct target positioning errors in radiotherapy of thoracic cancer
- PMID: 23039621
- PMCID: PMC3461048
- DOI: 10.1118/1.4748503
A study of respiration-correlated cone-beam CT scans to correct target positioning errors in radiotherapy of thoracic cancer
Abstract
Purpose: There is increasingly widespread usage of cone-beam CT (CBCT) for guiding radiation treatment in advanced-stage lung tumors, but difficulties associated with daily CBCT in conventionally fractionated treatments include imaging dose to the patient, increased workload and longer treatment times. Respiration-correlated cone-beam CT (RC-CBCT) can improve localization accuracy in mobile lung tumors, but further increases the time and workload for conventionally fractionated treatments. This study investigates whether RC-CBCT-guided correction of systematic tumor deviations in standard fractionated lung tumor radiation treatments is more effective than 2D image-based correction of skeletal deviations alone. A second study goal compares respiration-correlated vs respiration-averaged images for determining tumor deviations.
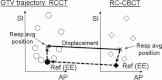
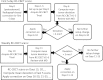
Methods: Eleven stage II-IV nonsmall cell lung cancer patients are enrolled in an IRB-approved prospective off-line protocol using RC-CBCT guidance to correct for systematic errors in GTV position. Patients receive a respiration-correlated planning CT (RCCT) at simulation, daily kilovoltage RC-CBCT scans during the first week of treatment and weekly scans thereafter. Four types of correction methods are compared: (1) systematic error in gross tumor volume (GTV) position, (2) systematic error in skeletal anatomy, (3) daily skeletal corrections, and (4) weekly skeletal corrections. The comparison is in terms of weighted average of the residual GTV deviations measured from the RC-CBCT scans and representing the estimated residual deviation over the treatment course. In the second study goal, GTV deviations computed from matching RCCT and RC-CBCT are compared to deviations computed from matching respiration-averaged images consisting of a CBCT reconstructed using all projections and an average-intensity-projection CT computed from the RCCT.
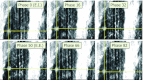
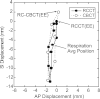
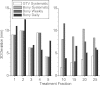
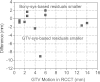
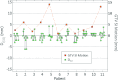
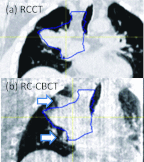
Results: Of the eleven patients in the GTV-based systematic correction protocol, two required no correction, seven required a single correction, one required two corrections, and one required three corrections. Mean residual GTV deviation (3D distance) following GTV-based systematic correction (mean ± 1 standard deviation 4.8 ± 1.5 mm) is significantly lower than for systematic skeletal-based (6.5 ± 2.9 mm, p = 0.015), and weekly skeletal-based correction (7.2 ± 3.0 mm, p = 0.001), but is not significantly lower than daily skeletal-based correction (5.4 ± 2.6 mm, p = 0.34). In two cases, first-day CBCT images reveal tumor changes-one showing tumor growth, the other showing large tumor displacement-that are not readily observed in radiographs. Differences in computed GTV deviations between respiration-correlated and respiration-averaged images are 0.2 ± 1.8 mm in the superior-inferior direction and are of similar magnitude in the other directions.
Conclusions: An off-line protocol to correct GTV-based systematic error in locally advanced lung tumor cases can be effective at reducing tumor deviations, although the findings need confirmation with larger patient statistics. In some cases, a single cone-beam CT can be useful for assessing tumor changes early in treatment, if more than a few days elapse between simulation and the start of treatment. Tumor deviations measured with respiration-averaged CT and CBCT images are consistent with those measured with respiration-correlated images; the respiration-averaged method is more easily implemented in the clinic.
Figures

References
-
- RTOG0617, “A randomized phase III comparison of standard-dose (60 Gy) versus high-dose (74 Gy) conformal radiotherapy with concurrent and consolidation carboplatin paclitaxel +/− cetuximab in patients with stage IIIA/IIIB non-small cell lung cancer” (2011) (available URL: http://www.rtog.org/ClinicalTrials/ProtocolTable/StudyDetails.aspx?study...). Last accessed April 30, 2012.
-
- RTOG1106, “Randomized phase II trial of individualized adaptive radiotherapy using during-treatment FDG-PET/CT and modern technology in locally advanced non-small cell lung cancer (NSCLC)” (2011) (available URL: http://www.rtog.org/ClinicalTrials/ProtocolTable/StudyDetails.aspx?study...). Last accessed April 30, 2012.
-
- Bissonnette J. P., Franks K. N., Purdie T. G., Moseley D. J., Sonke J. J., Jaffray D. A., Dawson L. A., and Bezjak A., “Quantifying interfraction and intrafraction tumor motion in lung stereotactic body radiotherapy using respiration-correlated cone beam computed tomography,” Int. J. Radiat. Oncol. Biol. Phys. 75, 688–695 (2009).10.1016/j.ijrobp.2008.11.066 - DOI - PubMed
-
- Purdie T. G., Moseley D. J., Bissonnette J. P., Sharpe M. B., Franks K., Bezjak A., and Jaffray D. A., “Respiration correlated cone-beam computed tomography and 4DCT for evaluating target motion in Stereotactic Lung Radiation Therapy,” Acta Oncol. 45, 915–922 (2006).10.1080/02841860600907345 - DOI - PubMed
-
- Grills I. S., Hugo G., Kestin L. L., Galerani A. P., Chao K. K., Wloch J., and Yan D., “Image-guided radiotherapy via daily online cone-beam CT substantially reduces margin requirements for stereotactic lung radiotherapy,” Int. J. Radiat. Oncol. Biol. Phys. 70, 1045–1056 (2008).10.1016/j.ijrobp.2007.07.2352 - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

