Community-based care for the management of type 2 diabetes: an evidence-based analysis
- PMID: 23074528
- PMCID: PMC3377524
Community-based care for the management of type 2 diabetes: an evidence-based analysis
Abstract
In June 2008, the Medical Advisory Secretariat began work on the Diabetes Strategy Evidence Project, an evidence-based review of the literature surrounding strategies for successful management and treatment of diabetes. This project came about when the Health System Strategy Division at the Ministry of Health and Long-Term Care subsequently asked the secretariat to provide an evidentiary platform for the Ministry's newly released Diabetes Strategy.After an initial review of the strategy and consultation with experts, the secretariat identified five key areas in which evidence was needed. Evidence-based analyses have been prepared for each of these five areas: insulin pumps, behavioural interventions, bariatric surgery, home telemonitoring, and community based care. For each area, an economic analysis was completed where appropriate and is described in a separate report.To review these titles within the Diabetes Strategy Evidence series, please visit the Medical Advisory Secretariat Web site, http://www.health.gov.on.ca/english/providers/program/mas/mas_about.html,DIABETES STRATEGY EVIDENCE PLATFORM: Summary of Evidence-Based AnalysesContinuous Subcutaneous Insulin Infusion Pumps for Type 1 and Type 2 Adult Diabetics: An Evidence-Based AnalysisBehavioural Interventions for Type 2 Diabetes: An Evidence-Based AnalysisBARIATRIC SURGERY FOR PEOPLE WITH DIABETES AND MORBID OBESITY: An Evidence-Based SummaryCommunity-Based Care for the Management of Type 2 Diabetes: An Evidence-Based AnalysisHome Telemonitoring for Type 2 Diabetes: An Evidence-Based AnalysisApplication of the Ontario Diabetes Economic Model (ODEM) to Determine the Cost-effectiveness and Budget Impact of Selected Type 2 Diabetes Interventions in Ontario
Objective: The objective of this report is to determine the efficacy of specialized multidisciplinary community care for the management of type 2 diabetes compared to usual care.
Clinical need: TARGET POPULATION AND CONDITION Diabetes (i.e. diabetes mellitus) is a highly prevalent chronic metabolic disorder that interferes with the body's ability to produce or effectively use insulin. The majority (90%) of diabetes patients have type 2 diabetes. (1) Based on the United Kingdom Prospective Diabetes Study (UKPDS), intensive blood glucose and blood pressure control significantly reduce the risk of microvascular and macrovascular complications in type 2 diabetics. While many studies have documented that patients often do not meet the glycemic control targets specified by national and international guidelines, factors associated with glycemic control are less well studied, one of which is the provider(s) of care. Multidisciplinary approaches to care may be particularly important for diabetes management. According guidelines from the Canadian Diabetes Association (CDA), the diabetes health care team should be multi-and interdisciplinary. Presently in Ontario, the core diabetes health care team consists of at least a family physician and/or diabetes specialist, and diabetes educators (registered nurse and registered dietician). Increasing the role played by allied health care professionals in diabetes care and their collaboration with physicians may represent a more cost-effective option for diabetes management. Several systematic reviews and meta-analyses have examined multidisciplinary care programs, but these have either been limited to a specific component of multidisciplinary care (e.g. intensified education programs), or were conducted as part of a broader disease management program, of which not all were multidisciplinary in nature. Most reviews also do not clearly define the intervention(s) of interest, making the evaluation of such multidisciplinary community programs challenging.
Research questions: What is the evidence of efficacy of specialized multidisciplinary community care provided by at least a registered nurse, registered dietician and physician (primary care and/or specialist) for the management of type 2 diabetes compared to usual care? [Henceforth referred to as Model 1]What is the evidence of efficacy of specialized multidisciplinary community care provided by at least a pharmacist and a primary care physician for the management of type 2 diabetes compared to usual care? [Henceforth referred to as Model 2]
Inclusion criteria: English language full-reportsPublished between January 1, 2000 and September 28, 2008Randomized controlled trials (RCTs), systematic reviews and meta-analysesType 2 diabetic adult population (≥18 years of age)Total sample size ≥30Describe specialized multidisciplinary community care defined as ambulatory-based care provided by at least two health care disciplines (of which at least one must be a specialist in diabetes) with integrated communication between the care providers.Compared to usual care (defined as health care provision by non-specialist(s) in diabetes, such as primary care providers; may include referral to other health care professionals/services as necessary)≥6 months follow-up
Exclusion criteria: Studies where discrete results on diabetes cannot be abstractedPredominantly home-based interventionsInpatient-based interventions
Outcomes of interest: The primary outcomes for this review were glycosylated hemoglobin (rHbA1c) levels and systolic blood pressure (SBP).
Search strategy: A literature search was performed on September 28, 2008 using OVID MEDLINE, MEDLINE In-Process and Other Non-Indexed Citations, EMBASE, the Cumulative Index to Nursing & Allied Health Literature (CINAHL), the Cochrane Library, and the International Agency for Health Technology Assessment (INAHTA) for studies published between January 1, 2000 and September 28, 2008. Abstracts were reviewed by a single reviewer and, for those studies meeting the eligibility criteria, full-text articles were obtained. Reference lists were also examined for any additional relevant studies not identified through the search. Articles with unknown eligibility were reviewed with a second clinical epidemiologist, then a group of epidemiologists until consensus was established. The quality of evidence was assessed as high, moderate, low or very low according to GRADE methodology. Given the high clinical heterogeneity of the articles that met the inclusion criteria, specific models of specialized multidisciplinary community care were examined based on models of care that are currently being supported in Ontario, models of care that were commonly reported in the literature, as well as suggestions from an Expert Advisory Panel Meeting held on January 21, 2009.
Summary of findings: The initial search yielded 2,116 unique citations, from which 22 RCTs trials and nine systematic reviews published were identified as meeting the eligibility criteria. Of these, five studies focused on care provided by at least a nurse, dietician, and physician (primary care and/or specialist) model of care (Model 1; see Table ES 1), while three studies focused on care provided by at least a pharmacist and primary care physician (Model 2; see Table ES 2). Based on moderate quality evidence, specialized multidisciplinary community care Model 2 has demonstrated a statistically and clinically significant reduction in HbA1c of 1.0% compared with usual care. The effects of this model on SBP, however, are uncertain compared with usual care, based on very-low quality evidence. Specialized multidisciplinary community care Model 2 has demonstrated a statistically and clinically significant reduction in both HbA1c of 1.05% (based on high quality evidence) and SBP of 7.13 mm Hg (based on moderate quality evidence) compared to usual care. For both models, the evidence does not suggest a preferred setting of care delivery (i.e., primary care vs. hospital outpatient clinic vs. community clinic). Table ES1:Summary of Results of Meta-Analyses of the Effects of Multidisciplinary Care Model 1OutcomeEstimate of effect(95% CI)Heterogeneity I(2)(p-value)GRADEGlycosylated Hemoglobin (HbA1c [%])-1.00 [-1.27, -0.73]4% (p=0.37)Moderate-quality Subgroup: Moderate-to-High Quality-0.91 [-1.19, -0.62]0% (p=0.74)Systolic Blood Pressure (mm Hg)-2.04 [-13.80, 9.72]89% (p=0.002)Very-low quality*Mean change from baseline to follow-up between intervention and control groupsTable ES2:Summary of Results of Meta-Analyses of the Effects of Multidisciplinary Care Model 2OutcomeEstimate of effect(95% CI)Heterogeneity I(2)(p-value)GRADEGlycosylated Hemoglobin (HbA1c [%])-1.05 [-1.57, -0.52]0% (p=0.75)High-qualitySystolic Blood Pressure (mm Hg)-7.13 [-11.78, -2.48]46% (p=0.17)Moderate quality*Mean change from baseline to follow-up between intervention and control groups.
Figures







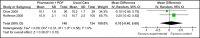
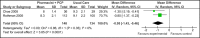
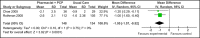




References
-
- Canadian Diabetes Association Clinical Practice Guidelines Expert Committee. Canadian Diabetes Association 2008 clinical practice guidelines for the prevention and management of diabetes in Canada. Can J Diabetes. 2008;32((Suppl 1)):S1–S201. - PubMed
-
- Lipscombe LL, Hux JE. Trends in diabetes prevalence, incidence, and mortality in Ontario, Canada 1995-2005: a population-based study. Lancet. 2007;369(9563):750–6. - PubMed
-
- Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33) Lancet. 1998;352(9131):837–53. UK Prospective Diabetes Study (UKPDS) Group. - PubMed
-
- Shah BR, Hux JE, Laupacis A, Mdcm BZ, Austin PC, van WC. Diabetic patients with prior specialist care have better glycaemic control than those with prior primary care. J Eval Clin Pract. 2005;11(6):568–75. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
