Platelets in pulmonary vascular physiology and pathology
- PMID: 23130099
- PMCID: PMC3487299
- DOI: 10.4103/2045-8932.101398
Platelets in pulmonary vascular physiology and pathology
Abstract
Almost a trillion platelets pass through the pulmonary circulation every minute, yet little is known about how they support pulmonary physiology or contribute to the pathogenesis of lung diseases. When considering this conundrum, three questions jump out: Does platelet production in the lungs occur? Why does severe thrombocytopenia-which undercuts the principal physiological role of platelets to effect hemostasis-not lead to pulmonary hemorrhage? Why does atherothrombosis-which platelets initiate, maintain, and trigger is other critically important arterial beds-not develop in the pulmonary artery? The purpose of this review is to explore these and derivative questions by providing data within a conceptual framework that begins to organize a subject that is largely unassembled.
Keywords: cell signaling; hemostasis; platelets; thrombosis; vascular biology.
Conflict of interest statement
Figures

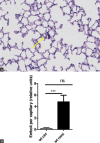


References
-
- Kroll MH. Platelets in pulmonary vascular physiology and pathology. In: Yuan JX, Garcia JG, Hales CA, Rich S, Archer SL, West JB, editors. Textbook of Pulmonary Vascular Disease. New York, N.Y: Springer; 2011. pp. 371–84.
-
- Battinelli EM, Hartwig JH, Italiano JE., Jr Delivering new insight into the biology of megakaryopoiesis and thrombopoiesis. Curr Opin Hematol. 2007;14:419–26. - PubMed
-
- Junt T, Schulze H, Chen Z, Massberg S, Goerge T, Krueger A, et al. Dynamic visualization of thrombopoiesis within bone marrow. Science. 2007;317:1767–70. - PubMed
LinkOut - more resources
Full Text Sources

