Mupirocin and chlorhexidine resistance in Staphylococcus aureus in patients with community-onset skin and soft tissue infections
- PMID: 23147738
- PMCID: PMC3535967
- DOI: 10.1128/AAC.01633-12
Mupirocin and chlorhexidine resistance in Staphylococcus aureus in patients with community-onset skin and soft tissue infections
Abstract
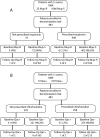
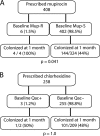
Decolonization measures, including mupirocin and chlorhexidine, are often prescribed to prevent Staphylococcus aureus skin and soft tissue infections (SSTI). The objective of this study was to determine the prevalence of high-level mupirocin and chlorhexidine resistance in S. aureus strains recovered from patients with SSTI before and after mupirocin and chlorhexidine administration and to determine whether carriage of a mupirocin- or chlorhexidine-resistant strain at baseline precluded S. aureus eradication. We recruited 1,089 patients with community-onset SSTI with or without S. aureus colonization. In addition to routine care, 483 patients were enrolled in a decolonization trial: 408 received intranasal mupirocin (with or without antimicrobial baths), and 258 performed chlorhexidine body washes. Patients were followed for up to 12 months with repeat colonization cultures. All S. aureus isolates were tested for high-level mupirocin and chlorhexidine resistance. At baseline, 23/1,089 (2.1%) patients carried a mupirocin-resistant S. aureus strain and 10/1,089 (0.9%) patients carried chlorhexidine-resistant S. aureus. Of 4 patients prescribed mupirocin, who carried a mupirocin-resistant S. aureus strain at baseline, 100% remained colonized at 1 month compared to 44% of the 324 patients without mupirocin resistance at baseline (P = 0.041). Of 2 patients prescribed chlorhexidine, who carried a chlorhexidine-resistant S. aureus strain at baseline, 50% remained colonized at 1 month compared to 48% of the 209 patients without chlorhexidine resistance at baseline (P = 1.0). The overall prevalence of mupirocin and chlorhexidine resistance is low in S. aureus isolates recovered from outpatients, but eradication efforts were less successful in patients carrying a mupirocin-resistant S. aureus strain at baseline.
Figures
References
-
- Calfee DP, Salgado CD, Classen D, Arias KM, Podgorny K, Anderson DJ, Burstin H, Coffin SE, Dubberke ER, Fraser V, Gerding DN, Griffin FA, Gross P, Kaye KS, Klompas M, Lo E, Marschall J, Mermel LA, Nicolle L, Pegues DA, Perl TM, Saint S, Weinstein RA, Wise R, Yokoe DS. 2008. Strategies to prevent transmission of methicillin-resistant Staphylococcus aureus in acute care hospitals. Infect. Control Hosp. Epidemiol. 29(Suppl 1):S62–S80 - PubMed
-
- Bode LG, Kluytmans JA, Wertheim HF, Bogaers D, Vandenbroucke-Grauls CM, Roosendaal R, Troelstra A, Box AT, Voss A, van der Tweel I, van Belkum A, Verbrugh HA, Vos MC. 2010. Preventing surgical-site infections in nasal carriers of Staphylococcus aureus. N. Engl. J. Med. 362:9–17 - PubMed
-
- Milstone AM, Passaretti CL, Perl TM. 2008. Chlorhexidine: expanding the armamentarium for infection control and prevention. Clin. Infect. Dis. 46:274–281 - PubMed
-
- Perl TM, Cullen JJ, Wenzel RP, Zimmerman MB, Pfaller MA, Sheppard D, Twombley J, French PP, Herwaldt LA. 2002. Intranasal mupirocin to prevent postoperative Staphylococcus aureus infections. N. Engl. J. Med. 346:1871–1877 - PubMed
-
- Creech CB, Beekmann SE, Chen Y, Polgreen PM. 2008. Variability among pediatric infectious diseases specialists in the treatment and prevention of methicillin-resistant Staphylococcus aureus skin and soft tissue infections. Pediatr. Infect. Dis. J. 27:270–272 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

