Outcomes of palliative bowel surgery for malignant bowel obstruction in patients with gynecological malignancy
- PMID: 23162616
- PMCID: PMC3499592
- DOI: 10.3892/ol.2012.835
Outcomes of palliative bowel surgery for malignant bowel obstruction in patients with gynecological malignancy
Abstract
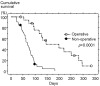
The aim of this study was to evaluate the outcomes of patients with a gynecological malignancy who received palliative care with and without surgical procedures for malignant bowel obstruction (MBO) and to explore prognostic factors to aid the selection of patients who would benefit from palliative surgery. Medical records of patients with MBO due to a gynecological malignancy treated at our institute between 2005 and 2010 were reviewed. Successful palliation following surgery was defined as the ability to tolerate solid food for at least 60 days. Clinical variables were analyzed using Chi-square or Fisher's exact tests. Survival was evaluated using the Kaplan-Meier method and log-rank test. A total of 53 cases were identified; 20 had bowel surgery for MBO as a palliative procedure and 33 did not. Colostomy was performed in 11 (55%) of 20 patients and ileostomy was performed in 7 (35%). The postoperative morbidity was 35% and mortality within 30 days was 5%. Successful palliation following surgery was achieved in 14 (70%) of 20 cases with a median period of 146 days (range, 61-294). Survival following the diagnosis of MBO was longer in cases with surgery than those without (median survival time, 146 versus 69 days; P<0.0001). Although age, presence of ascites, laboratory values and types of prior anticancer therapy were not significantly different, a longer interval from last anticancer therapy to diagnosis of MBO was observed in patients who underwent surgery compared with those who did not (median, 57 versus 30 days; P<0.05), as well as superior performance status. Among the patients with surgery, the interval was also longer in patients with successful palliation compared with those without (median, 83 versus 32 days; P<0.05). The palliative benefit of surgery for MBO in selected patients with gynecological malignancy was observed. The interval from last anticancer therapy to diagnosis of MBO may serve as a prognostic factor when considering surgical intervention.
Figures
References
-
- Krebs HB, Goplerud DR. Surgical management of bowel obstruction in advanced ovarian carcinoma. Obstet Gynecol. 1983;61:327–330. - PubMed
-
- Fernandes JR, Seymour RJ, Suissa S. Bowel obstruction in patients with ovarian cancer: a search for prognostic factors. Am J Obstet Gynecol. 1988;158:244–249. - PubMed
-
- Zoetmulder FA, Helmerhorst TJ, van Coevorden F, Wolfs PE, Leyer JP, Hart AA. Management of bowel obstruction in patients with advanced ovarian cancer. Eur J Cancer. 1994;30A:1625–1628. - PubMed
-
- Ripamonti C, Bruera E. Palliative management of malignant bowel obstruction. Int J Gynecol Cancer. 2002;12:135–143. - PubMed
-
- Medina-Franco H, García-Alvarez MN, Ortiz-López LJ, Cuairán JZ. Predictors of adverse surgical outcome in the management of malignant bowel obstruction. Rev Invest Clin. 2008;60:212–216. - PubMed
LinkOut - more resources
Full Text Sources
Medical