Effects of etomidate on complications related to intubation and on mortality in septic shock patients treated with hydrocortisone: a propensity score analysis
- PMID: 23171852
- PMCID: PMC3672604
- DOI: 10.1186/cc11871
Effects of etomidate on complications related to intubation and on mortality in septic shock patients treated with hydrocortisone: a propensity score analysis
Abstract
Introduction: Endotracheal intubation in the ICU is associated with a high incidence of complications. Etomidate use is debated in septic shock because it increases the risk of critical illness-related corticosteroid insufficiency, which may impact outcome. We hypothesized that hydrocortisone, administered in all septic shock cases in our ICU, may counteract some negative effects of etomidate.
Methods: A single-center observational study was carried out in septic shock patients, treated with hydrocortisone and intubated within the first 48 hours of septic shock. Co-primary end points were life-threatening complications incidence occurring within the first hour after intubation and mortality during the ICU stay. Statistical analyses included unmatched and matched cohorts using a propensity score analysis. P < 0.05 was considered significant.
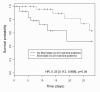
Results: Sixty patients in the etomidate cohort and 42 patients in the non-etomidate cohort were included. Critical illness-related corticosteroid insufficiency was 79% in the etomidate cohort and 52% in the non-etomidate cohort (P = 0.01). After intubation, life-threatening complications occurred in 36% of the patients whatever the cohort. After adjustment with propensity score analysis, etomidate was a protective factor for death in the ICU both in unmatched (hazard ratio, 0.33 (0.15 to 0.75); P < 0.01)) and matched cohorts (hazard ratio, 0.33 (0.112 to 0.988); P = 0.04).
Conclusion: In septic shock patients treated with hydrocortisone, etomidate did not decrease life-threatening complications following intubation, but when associated with hydrocortisone it also did not impair outcome.
Figures

Comment in
-
Etomidate for intubation of patients who have sepsis or septic shock--where do we go from here?Crit Care. 2012 Dec 27;16(6):189. doi: 10.1186/cc11889. Crit Care. 2012. PMID: 23273139 Free PMC article.
Similar articles
-
Etomidate for intubation of patients who have sepsis or septic shock--where do we go from here?Crit Care. 2012 Dec 27;16(6):189. doi: 10.1186/cc11889. Crit Care. 2012. PMID: 23273139 Free PMC article.
-
Outcomes of etomidate in severe sepsis and septic shock.Chest. 2010 Dec;138(6):1327-32. doi: 10.1378/chest.10-0790. Epub 2010 Jul 22. Chest. 2010. PMID: 20651024
-
Single-dose etomidate is not associated with increased mortality in ICU patients with sepsis: analysis of a large electronic ICU database.Crit Care Med. 2013 Mar;41(3):774-83. doi: 10.1097/CCM.0b013e318274190d. Crit Care Med. 2013. PMID: 23318491
-
Should we use etomidate as an induction agent for endotracheal intubation in patients with septic shock?: a critical appraisal.Chest. 2005 Mar;127(3):1031-8. doi: 10.1378/chest.127.3.1031. Chest. 2005. PMID: 15764790 Review.
-
[Etomidate can not be recommended to patients with septic shock].Ugeskr Laeger. 2011 May 16;173(20):1421-3. Ugeskr Laeger. 2011. PMID: 21586246 Review. Danish.
Cited by
-
Corticosteroid receptor rebalancing alleviates critical illness-related corticosteroid insufficiency after traumatic brain injury by promoting paraventricular nuclear cell survival via Akt/CREB/BDNF signaling.J Neuroinflammation. 2020 Oct 25;17(1):318. doi: 10.1186/s12974-020-02000-2. J Neuroinflammation. 2020. PMID: 33100225 Free PMC article.
-
Etomidate for intubation of patients who have sepsis or septic shock--where do we go from here?Crit Care. 2012 Dec 27;16(6):189. doi: 10.1186/cc11889. Crit Care. 2012. PMID: 23273139 Free PMC article.
-
Current trends in emergency airway management: a clinical review.Clin Exp Emerg Med. 2024 Sep;11(3):243-258. doi: 10.15441/ceem.23.173. Epub 2024 Mar 15. Clin Exp Emerg Med. 2024. PMID: 38485262 Free PMC article.
-
Risk factors for corticosteroid insufficiency during the sub-acute phase of acute traumatic brain injury.Neural Regen Res. 2020 Jul;15(7):1259-1265. doi: 10.4103/1673-5374.272611. Neural Regen Res. 2020. PMID: 31960811 Free PMC article.
-
Incidence of and risk factors for severe cardiovascular collapse after endotracheal intubation in the ICU: a multicenter observational study.Crit Care. 2015 Jun 18;19(1):257. doi: 10.1186/s13054-015-0975-9. Crit Care. 2015. PMID: 26084896 Free PMC article.
References
-
- Jaber S, Amraoui J, Lefrant JY, Arich C, Cohendy R, Landreau L, Calvet Y, Capdevila X, Mahamat A, Eledjam JJ. Clinical practice and risk factors for immediate complications of endotracheal intubation in the intensive care unit: a prospective, multiple-center study. Crit Care Med. 2006;16:2355–2361. doi: 10.1097/01.CCM.0000233879.58720.87. - DOI - PubMed
-
- Petrini F, Accorsi A, Adrario E, Agro F, Amicucci G, Antonelli M, Azzeri F, Baroncini S, Bettelli G, Cafaggi C, Cattano D, Chinelli E, Corbanese U, Corso R, Della Puppa A, Di Filippo A, Facco E, Favaro R, Favero R, Frova G, Giunta F, Giurati G, Giusti F, Guarino A, Iannuzzi E, Ivani G, Mazzon D, Menarini M, Merli G, Mondello E. et al.Recommendations for airway control and difficult airway management. Minerva Anestesiol. 2005;16:617–657. - PubMed
-
- Jaber S, Jung B, Corne P, Sebbane M, Muller L, Chanques G, Verzilli D, Jonquet O, Eledjam JJ, Lefrant JY. An intervention to decrease complications related to endotracheal intubation in the intensive care unit: a prospective, multiple-center study. Intensive Care Med. 2010;16:248–255. doi: 10.1007/s00134-009-1717-8. - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

