Psychological therapies for the management of chronic and recurrent pain in children and adolescents
- PMID: 23235601
- PMCID: PMC3715398
- DOI: 10.1002/14651858.CD003968.pub3
Psychological therapies for the management of chronic and recurrent pain in children and adolescents
Update in
-
Psychological therapies for the management of chronic and recurrent pain in children and adolescents.Cochrane Database Syst Rev. 2014 May 5;2014(5):CD003968. doi: 10.1002/14651858.CD003968.pub4. Cochrane Database Syst Rev. 2014. Update in: Cochrane Database Syst Rev. 2018 Sep 29;9:CD003968. doi: 10.1002/14651858.CD003968.pub5. PMID: 24796681 Free PMC article. Updated.
Abstract
Background: Chronic pain affects many children, who report severe pain, distressed mood, and disability. Psychological therapies are emerging as effective interventions to treat children with chronic or recurrent pain. This update adds recently published randomised controlled trials (RCTs) to the review published in 2009.
Objectives: To assess the effectiveness of psychological therapies, principally cognitive behavioural therapy and behavioural therapy, for reducing pain, disability, and improving mood in children and adolescents with recurrent, episodic, or persistent pain. We also assessed the risk of bias and methodological quality of the included studies.
Search methods: Searches were undertaken of MEDLINE, EMBASE, and PsycLIT. We searched for RCTs in references of all identified studies, meta-analyses and reviews. Date of most recent search: March 2012.
Selection criteria: RCTs with at least 10 participants in each arm post-treatment comparing psychological therapies with active treatment were eligible for inclusion (waiting list or standard medical care) for children or adolescents with episodic, recurrent or persistent pain.
Data collection and analysis: All included studies were analysed and the quality of the studies recorded. All treatments were combined into one class: psychological treatments; headache and non-headache outcomes were separately analysed on three outcomes: pain, disability, and mood. Data were extracted at two time points; post-treatment (immediately or the earliest data available following end of treatment) and at follow-up (at least three months after the post-treatment assessment point, but not more than 12 months).
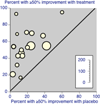
Main results: Eight studies were added in this update of the review, giving a total of 37 studies. The total number of participants completing treatments was 1938. Twenty-one studies addressed treatments for headache (including migraine); seven for abdominal pain; four included mixed pain conditions including headache pain, two for fibromyalgia, two for pain associated with sickle cell disease, and one for juvenile idiopathic arthritis. Analyses revealed five significant effects. Pain was found to improve for headache and non-headache groups at post-treatment, and for the headache group at follow-up. Mood significantly improved for the headache group at follow-up, although, this should be interpreted with caution as there were only two small studies entered into the analysis. Finally, disability significantly improved in the non-headache group at post-treatment. There were no other significant effects.
Authors' conclusions: Psychological treatments are effective in reducing pain intensity for children and adolescents (<18 years) with headache and benefits from therapy appear to be maintained. Psychological treatments also improve pain and disability for children with non-headache pain. There is limited evidence available to estimate the effects of psychological therapies on mood for children and adolescents with headache and non-headache pain. There is also limited evidence to estimate the effects on disability in children with headache. These conclusions replicate and add to those of the previous review which found psychological therapies were effective in reducing pain intensity for children with headache and non-headache pain conditions, and these effects were maintained at follow-up.
Figures



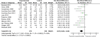












Update of
-
Psychological therapies for the management of chronic and recurrent pain in children and adolescents.Cochrane Database Syst Rev. 2009 Apr 15;(2):CD003968. doi: 10.1002/14651858.CD003968.pub2. Cochrane Database Syst Rev. 2009. Update in: Cochrane Database Syst Rev. 2012 Dec 12;12:CD003968. doi: 10.1002/14651858.CD003968.pub3. PMID: 19370592 Updated.
References
References to studies included in this review
-
- Abram HS, Buckloh LM, Schilling LS, Armatti Wiltrout S, Ramirez-Garnica G, Turk WR. A randomized, controlled trail of a neurological and psychoeducational group appointment model for pediatric headaches. Children’s Healthcare. 2007;36:249–265.
-
- Alfven G, Lindstrom A. A new method for the treatment of recurrent abdominal pain of prolonged negative stress origin. Acta Pediatrica. 2007;96:76–81. - PubMed
-
- Barry J, von Baeyer CL. Brief cognitive-behavioral group treatment for children’s headache. Clinical Journal of Pain. 1997;13:215–220. - PubMed
-
- Bussone G, Grazzi L, D’Amico D, Leone M, Andrasik F. Biofeedback-assisted relaxation training for young adolescents with tension-type headache: A controlled study. Cephalalgia. 1988;18:463–467. - PubMed
References to studies excluded from this review
-
- Fentress DW, Masek BJ, Mehegan JE, Benson H. Biofeedback and relaxation-response training in the treatment of pediatric migraine. Developmental Medicine and Child Neurology. 1986;28:139–146. - PubMed
-
- Kroner-Herwig B, Mohn U, Pothmann R. Comparison of biofeedback and relaxation in the treatment of pediatric headache and the influence of parent involvement on outcome. Applied Psychophysiology and Biofeedback. 1998;23:143–157. - PubMed
-
- Larsson B, Melin L. Chronic headaches in adolescents: treatment in a school setting with relaxation training as compared with information-contact and self-registration. Pain. 1986;25:325–336. - PubMed
-
- Olness K, MacDonald JT, Uden DL. Comparison of self-hypnosis and propranolol in the treatment of juvenile classic migraine. Pediatrics. 1987;79(4):593–597. - PubMed
-
- Sanders MR, Rebgetz M, Morrison M, Bor W, Gordon A, Dadds M, et al. Cognitive-behavioral treatment of recurrent nonspecific abdominal pain in children: an analysis of generalization, maintenance, and side effects. Journal of Consulting and Clinical Psychology. 1989;57(2):294–300. - PubMed
Additional references
-
- Bursch B, Walco GA, Zeltzer L. Clinical assessment and management of chronic pain and pain-associated disability syndrome. Developmental and Behavioral Pediatrics. 1998;19:45–53. - PubMed
-
- Cohen J. A power primer. Psychological Bulletin. 1992;112(1):155–159. - PubMed
-
- Eccleston C, Williams ACdeC, Morley S. Psychological therapies for the management of chronic pain (excluding headache) in adults. Cochrane Database of Systematic Reviews. 2009;(Issue 2) - PubMed
References to other published versions of this review
-
- Eccleston C, Yorke L, Morley S, Williams ACdeC, Mastroyannopoulou A. Psychological therapies for the management of chronic and recurrent pain in children and adolescents. Cochrane Database of Systematic Reviews. 2003;(Issue 1) - PubMed
-
- Eccleston C, Palermo TM, Williams ACDC, Lewandowski A, Morley S. Psychological therapies for the management of chronic and recurrent pain in children and adolescents. Cochrane Database of Systematic Reviews. 2009;(Issue 2) - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

