Vaginal degeneration following implantation of synthetic mesh with increased stiffness
- PMID: 23240802
- PMCID: PMC3531826
- DOI: 10.1111/1471-0528.12085
Vaginal degeneration following implantation of synthetic mesh with increased stiffness
Abstract
Objective: To compare the impact of the prototype prolapse mesh Gynemesh PS with that of two new-generation lower stiffness meshes, UltraPro and SmartMesh, on vaginal morphology and structural composition.
Design: A mechanistic study employing a nonhuman primate model.
Setting: Magee-Womens Research Institute at the University of Pittsburgh.
Population: Parous rhesus macaques, with similar age, weight, parity and Pelvic Organ Prolapse-Questionnaire scores.
Methods: Following Institutional Animal Care Use Committee approval, 50 rhesus macaques were implanted with Gynemesh PS (n = 12), UltraPro with its blue line perpendicular to the longitudinal axis of vagina (n = 10), UltraPro with its blue line parallel to the longitudinal axis of vagina (n = 8) or SmartMesh (n = 8) via sacrocolpopexy following hysterectomy. Sham-operated animals (n = 12) served as controls.
Main outcome measures: The mesh-vagina complex was removed after 12 weeks and analysed for histomorphology, in situ cell apoptosis, total collagen, elastin, glycosaminoglycan content and total collagenase activity. Appropriate statistics and correlation analyses were performed accordingly.
Results: Relative to sham and the two lower stiffness meshes, Gynemesh PS had the greatest negative impact on vaginal histomorphology and composition. Compared with sham, implantation with Gynemesh PS caused substantial thinning of the smooth muscle layer (1557 ± 499 μm versus 866 ± 210 μm, P = 0.02), increased apoptosis particularly in the area of the mesh fibres (P = 0.01), decreased collagen and elastin content (20%, P = 0.03 and 43%, P = 0.02, respectively) and increased total collagenase activity (135%, P = 0.01). Glycosaminoglycan, a marker of tissue injury, was highest with Gynemesh PS compared with sham and other meshes (P = 0.01).
Conclusion: Mesh implantation with the stiffer mesh Gynemesh PS induced a maladaptive remodelling response consistent with vaginal degeneration.
© 2013 The Authors BJOG An International Journal of Obstetrics and Gynaecology © 2013 RCOG.
Conflict of interest statement
Figures
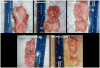
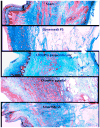

References
-
- Olsen AL, et al. Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol. 1997;89(4):501–6. - PubMed
-
- Boyles SH, Weber AM, Meyn L. Procedures for pelvic organ prolapse in the United States, 1979–1997. Am J Obstet Gynecol. 2003;188(1):108–15. - PubMed
-
- Kenton K, Mueller ER. The global burden of female pelvic floor disorders. BJU Int. 2006;98(Suppl 1):1–5. discussion 6–7. - PubMed
-
- Subak LL, et al. Cost of pelvic organ prolapse surgery in the United States. Obstet Gynecol. 2001;98(4):646–51. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

