Graft-versus-host disease impairs vaccine responses through decreased CD4+ and CD8+ T cell proliferation and increased perforin-mediated CD8+ T cell apoptosis
- PMID: 23275602
- PMCID: PMC3626171
- DOI: 10.4049/jimmunol.1200391
Graft-versus-host disease impairs vaccine responses through decreased CD4+ and CD8+ T cell proliferation and increased perforin-mediated CD8+ T cell apoptosis
Abstract
Tumor-targeted vaccines represent a strategy to enhance the graft-versus-leukemia effect after allogeneic blood and marrow transplantation (BMT). We have previously shown that graft-versus-host disease (GVHD) can negatively impact quantitative responses to vaccines. Using a minor histocompatibility Ag-mismatched BMT (B6 → B6 × C3H.SW) followed by adoptive transfer of HY-specific T cells and HY-expressing dendritic cells, we assessed whether GVHD induced by donor lymphocyte infusion (DLI) affects the persistence, proliferation, and survival of vaccine-responding, nonalloantigen reactive T cells. Both CD8(+) and CD4(+) HY-specific T cells undergo less vaccine-driven proliferation in allogeneic recipients with GVHD. Although vaccine-responding CD8(+) T cells show decreased IFN-γ and CD107a production, CD4(+) T cells exhibit increased programmed death 1 and T cell Ig mucin-like domain 3 expression. In addition, the degree of apoptosis in vaccine-responding CD8(+) T cells was higher in the presence of GVHD, but there was no difference in CD4(+) T cell apoptosis. Using Fas ligand-deficient or TRAIL-deficient DLI had no impact on apoptosis of HY-specific T cells. However, perforin-deficient alloreactive DLI induced significantly less apoptosis of vaccine-responding CD8(+) T cells and resulted in enhanced tumor protection. Thus, diminished vaccine responses during GVHD result from impaired proliferation of CD8(+) and CD4(+) T cells responding to vaccination, with an additional contribution from perforin-mediated CD8(+) T cell apoptosis. These results provide important insights toward optimizing vaccine responses after allogeneic BMT.
Figures



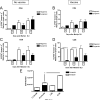


References
-
- Crooks GM, Weinberg K, Mackall C. Immune Reconstitution: From Stem Cells to Lymphocytes. Biology of Blood and Marrow Transplantation. 2006;12(1)(Supplement 1):42–6. - PubMed
-
- Hebib NC, Deas O, Rouleau M, Durrbach A, Charpentier B, Beaujean F, et al. Peripheral Blood T Cells Generated After Allogeneic Bone Marrow Transplantation: Lower Levels of Bcl-2 Protein and Enhanced Sensitivity to Spontaneous and CD95-Mediated Apoptosis In Vitro. Abrogation of the Apoptotic Phenotype Coincides With the Recovery of Normal Naive/Primed T-Cell Profiles. Blood. 1999 Sep 1;94(5):1803–13. 1999. - PubMed
-
- Lin M-T, Tseng L-H, Frangoul H, Gooley T, Pei J, Barsoukov A, et al. Increased apoptosis of peripheral blood T cells following allogeneic hematopoietic cell transplantation. Blood. 2000 Jun 15;95(12):3832–9. 2000. - PubMed
-
- Brochu S, Rioux-Masse B, Roy J, Roy D-C, Perreault C. Massive Activation-Induced Cell Death of Alloreactive T Cells With Apoptosis of Bystander Postthymic T Cells Prevents Immune Reconstitution in Mice With Graft-Versus-Host Disease. Blood. 1999 Jul 15;94(2):390–400. 1999. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Molecular Biology Databases
Research Materials
Miscellaneous

