Primary intraosseous squamous cell carcinoma mimicking periapical disease: a case report
- PMID: 23301215
- PMCID: PMC3534183
- DOI: 10.5624/isd.2012.42.4.265
Primary intraosseous squamous cell carcinoma mimicking periapical disease: a case report
Abstract
Primary intraosseous squamous cell carcinoma (PIOSCC) is a rare carcinoma, which arises within the jaws without connection to the oral mucosa and presumably develops from a remnant of odontogenic epithelium. We present a case of solid type PIOSCC in a 52-year-old male patient complaining of dull pain on his left lower molar. In this case, early stage PIOSCC mimicking a periapical lesion might lead to a one-year delay in treatment due to the misdiagnosis of osteomyelitis after extraction of the third molar. The clinical, radiological, and histologic features are described. In this case, there was initial radiographic evidence for PIOSCC mimicking a periapical lesion. Incautious radiographic interpretation and treatment procedures had delayed the correct diagnosis and resulted in extensive bony destruction during the patient's disease progression.
Keywords: Carcinoma, Squamous Cell; Head and Neck Neoplasms; Mandible; Periapical Disease.
Figures

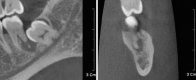
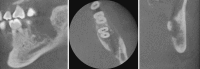

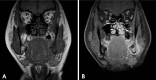
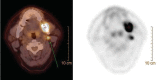
References
-
- Barnes L, Eveson JW, Reichart P, Sidransky D. World Health Organization classification of tumours: Pathology and genetics of head and neck tumours. Lyon: IARC Press; 2005. pp. 290–291.
-
- Eversole LR. Malignant epithelial odontogenic tumors. Semin Diagn Pathol. 1999;16:317–324. - PubMed
-
- Pindborg JJ, Kramer IR, Torloni H. International histological classification of tumours, No. 5. Histological typing of odontogenic tumours, jaw cysts, and allied lesions. Geneva: World Health Organization; 1971. pp. 35–36.
-
- Elzay RP. Primary intraosseous carcinoma of the jaws. Review and update of odontogenic carcinoma. Oral Surg Oral Med Oral Pathol. 1982;54:299–303. - PubMed
-
- Slootweg PJ, Müller H. Malignant ameloblastoma or ameloblastic carcinoma. Oral Surg Oral Med Oral Pathol. 1984;57:168–176. - PubMed

