Translating an understanding of the pathogenesis of hepatic fibrosis to novel therapies
- PMID: 23305825
- PMCID: PMC4151461
- DOI: 10.1016/j.cgh.2013.01.005
Translating an understanding of the pathogenesis of hepatic fibrosis to novel therapies
Abstract
The response to injury is one of wound healing and fibrogenesis, which ultimately leads to fibrosis. The fibrogenic response to injury is a generalized one across virtually all organ systems. In the liver, the injury response, typically occurring over a prolonged period of time, leads to cirrhosis (although it should be pointed out that not all patients with liver injury develop cirrhosis). The fact that many different diseases result in cirrhosis suggests a common pathogenesis. The study of hepatic fibrogenesis over the past 2 decades has been remarkably active, leading to a considerable understanding of this process. It clearly has been shown that the hepatic stellate cell is a central component in the fibrogenic process. It also has been recognized that other effector cells are important in the fibrogenic process, including resident fibroblasts, bone marrow-derived cells, fibrocytes, and even perhaps cells derived from epithelial cells (ie, through epithelial to mesenchymal transition). A key aspect of the biology of fibrogenesis is that the fibrogenic process is dynamic; thus, even advanced fibrosis (or cirrhosis) is reversible. Together, an understanding of the cellular basis for liver fibrogenesis, along with multiple aspects of the basic pathogenesis of fibrosis, have highlighted many exciting potential therapeutic opportunities. Thus, although the most effective antifibrotic therapy is simply treatment of the underlying disease, in situations in which this is not possible, specific antifibrotic therapy is likely not only to become feasible, but will soon become a reality. This review highlights the mechanisms underlying fibrogenesis that may be translated into future antifibrotic therapies and to review the current state of clinical development.
Copyright © 2013 AGA Institute. Published by Elsevier Inc. All rights reserved.
Figures

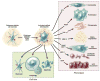
References
-
- Schuppan D. Structure of the extracellular matrix in normal and fibrotic liver: collagens and glycoproteins. Semin Liver Dis. 1990;10:1–10. - PubMed
-
- Rockey DC. The cell and molecular biology of hepatic fibrogenesis. Clinical and therapeutic implications. Clin Liver Dis. 2000;4:319–55. - PubMed
-
- Rockey DC. Antifibrotic therapy in chronic liver disease. Clin Gastroenterol Hepatol. 2005;3:95–107. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

