Assessment of whole body MRI and sestamibi technetium-99m bone marrow scan in prediction of multiple myeloma disease progression and outcome: a prospective comparative study
- PMID: 23315438
- PMCID: PMC3549203
- DOI: 10.1136/bmjopen-2012-002025
Assessment of whole body MRI and sestamibi technetium-99m bone marrow scan in prediction of multiple myeloma disease progression and outcome: a prospective comparative study
Abstract
Objectives: This study aims primarily to determine whether whole body MRI (WB-MRI) and Sestamibi Technetium-99m-bone marrow (MIBI) scans in the same patients produce the same estimate of disease load and location, and secondly, to study possible association between the bone disease detected by these scans and the effect on disease outcome and survival. Bone disease occurs in about 90% of multiple myeloma (MM) patients. There are no data comparing the new diagnostic modalities with WB-MRI and MIBI in MM.
Design: A prospective comparative study between WB-MRI and MIBI scans in assessing bone disease and outcome of MM.
Participants and methods: Sixty-two consecutive patients with confirmed MM underwent simultaneous WB-MRI (both axial T1 and turbo spin echo short tau inversion recovery (STIR)) and MIBI scans at a single institution from January 2010 to January 2011, and their survival status was determined in January 2012. The median age was 62 years (range 37-88) with a male-to-female ratio of 33 : 29.
Results: In vertebrae and long bones, MRI scan detected more disease compared with MIBI scan (p<0.001) but there was less difference in the skull (p=0.09). In the ribcage, the MIBI scan detected more lytic lesions of the ribs compared with MRI scan (p<0.001). Thirteen of the 62 patients died during the 24-month follow-up. Increased disease detected in all bones by both scans was associated with increased mortality risk (MIBI p=0.001; MRI-STIR p=0.044; but not MRI-T1 p=0.44). In all combined bone groups, the mean MIBI scan results provided a better prediction of mortality than MRI scan over the follow-up period (MRI-T1 vs MIBI p=0.019; MRI-STIR vs MIBI p=0.047).
Conclusions: Although WB-MRI detected more MM bone disease, MIBI scan predicted overall disease outcome and mortality better than MRI scan. Further studies to define optimum use of these imaging techniques are warranted.
Trial registration number: The study was registered prospectively in the Australian and New Zealand Clinical Trials Registry at http://www.ANZCTR.org.au under No: ACTRN12609000761268.
Figures


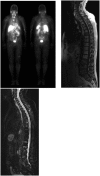
Similar articles
-
Technetium-99m 2-methoxy-isobutyl-isonitrile uptake scintigraphy in detection of the bone marrow infiltration in multiple myeloma: correlation with MRI and other prognostic factors.Ann Hematol. 2007 Nov;86(11):805-13. doi: 10.1007/s00277-007-0329-z. Epub 2007 Aug 8. Ann Hematol. 2007. PMID: 17684742 Clinical Trial.
-
Multiple myeloma: predictive value of Tc-99m MIBI scintigraphy and MRI in its diagnosis and therapy.Nucl Med Rev Cent East Eur. 2008;11(1):12-6. Nucl Med Rev Cent East Eur. 2008. PMID: 19173182 Clinical Trial.
-
Value of Tc-99m sestamibi scintigraphy in the detection of bone lesions in multiple myeloma: comparison with Tc-99m methylene diphosphonate.Ann Hematol. 2001 Jun;80(6):349-53. doi: 10.1007/s002770100302. Ann Hematol. 2001. PMID: 11475149
-
18F-FDG PET/CT, 99mTc-MIBI, and MRI in evaluation of patients with multiple myeloma.J Nucl Med. 2008 Feb;49(2):195-200. doi: 10.2967/jnumed.107.045641. Epub 2008 Jan 16. J Nucl Med. 2008. PMID: 18199607
-
Technetium-99m sestamibi scintigraphy is sensitive and specific for the staging and the follow-up of patients with multiple myeloma: a multicentre study on 397 scans.Br J Haematol. 2007 Mar;136(5):729-35. doi: 10.1111/j.1365-2141.2006.06489.x. Br J Haematol. 2007. PMID: 17233770
Cited by
-
99mTc-sestamibi SPECT/CT and 18F-FDG-PET/CT have similar performance but different imaging patterns in newly diagnosed multiple myeloma.Nucl Med Commun. 2020 Oct;41(10):1081-1088. doi: 10.1097/MNM.0000000000001259. Nucl Med Commun. 2020. PMID: 32732603 Free PMC article.
References
-
- Kyle RA, Gertz MA, Witzig TE, et al. Review of 1027 patients with newly diagnosed multiple myeloma. Mayo Clin Proc 2003;78:21–33 - PubMed
-
- Rajkumar SV, Kyle RA. Multiple myeloma—diagnosis and treatment. Mayo Clin Proc 2005;80:1371–82 - PubMed
-
- Roodman GD. Pathogenesis of myeloma bone disease. Blood Cells Mol Dis 2004;32:290–2 - PubMed
-
- Parkin DM, Bray F, Ferlay J, et al. Global cancer statistics, 2002. CA Cancer J Clin 2005;55:74–108 - PubMed
-
- D'Sa S, Abildgaard N, Tighe J, et al. Guidelines for the use of imaging in the management of myeloma. Br J Haematol 2007;137:49–63 - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
