The potassium channel KCa3.1 as new therapeutic target for the prevention of obliterative airway disease
- PMID: 23325003
- PMCID: PMC3777777
- DOI: 10.1097/TP.0b013e318275a2f4
The potassium channel KCa3.1 as new therapeutic target for the prevention of obliterative airway disease
Abstract
Background: The calcium-activated potassium channel KCa3.1 is critically involved in T-cell activation as well as in the proliferation of smooth muscle cells and fibroblasts. We sought to investigate whether KCa3.1 contributes to the pathogenesis of obliterative airway disease (OAD) and whether knockout or pharmacologic blockade would prevent the development of OAD.
Methods: Tracheas from CBA donors were heterotopically transplanted into the omentum of C57Bl/6J wild-type or KCa3.1 mice. C57Bl/6J recipients were either left untreated or received the KCa3.1 blocker TRAM-34 (120 mg/kg/day). Histopathology and immunologic assays were performed on postoperative day 5 or 28.
Results: Subepithelial T-cell and macrophage infiltration on postoperative day 5, as seen in untreated allografts, was significantly reduced in the KCa3.1 and TRAM-34 groups. Also, systemic Th1 activation was significantly and Th2 mildly reduced by KCa3.1 knockout or blockade. After 28 days, luminal obliteration of tracheal allografts was reduced from 89%±21% in untreated recipients to 53%±26% (P=0.010) and 59%±33% (P=0.032) in KCa3.1 and TRAM-34-treated animals, respectively. The airway epithelium was mostly preserved in syngeneic grafts, mostly destroyed in the KCa3.1 and TRAM-34 groups, and absent in untreated allografts. Allografts triggered an antibody response in untreated recipients, which was significantly reduced in KCa3.1 animals. KCa3.1 was detected in T cells, airway epithelial cells, and myofibroblasts. TRAM-34 dose-dependently suppressed proliferation of wild-type C57B/6J splenocytes but did not show any effect on KCa3.1 splenocytes.
Conclusions: Our findings suggest that KCa3.1 channels are involved in the pathogenesis of OAD and that KCa3.1 blockade holds promise to reduce OAD development.
Conflict of interest statement
Conflict of interests
none
Figures

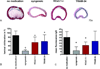


References
-
- Christie JD, Edwards LB, Kucheryavaya AY, et al. The Registry of the International Society for Heart and Lung Transplantation: Twenty-seventh official adult lung and heart-lung transplant report--2010. The Journal of Heart and Lung Transplantation. 29(10):1104. - PubMed
-
- Sundaresan S, Trulock EP, Mohanakumar T, Cooper JD, Patterson GA. Prevalence and outcome of bronchiolitis obliterans syndrome after lung transplantation. The Annals of Thoracic Surgery. 1995;60(5):1341. - PubMed
-
- Paradis I, Yousem S, Griffith B. Airway obstruction and bronchiolitis obliterans after lung transplantation. Clin Chest Med. 1993;14(4):751. - PubMed
-
- Burke C, Baldwin J, Morris A, et al. Twenty-eight cases of human heart-lung transplantation. The Lancet. 1986;327(8480):517. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

