Adverse events in healthy individuals and MDR-TB contacts treated with anti-tuberculosis drugs potentially effective for preventing development of MDR-TB: a systematic review
- PMID: 23326464
- PMCID: PMC3543458
- DOI: 10.1371/journal.pone.0053599
Adverse events in healthy individuals and MDR-TB contacts treated with anti-tuberculosis drugs potentially effective for preventing development of MDR-TB: a systematic review
Abstract
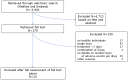
A recent systematic review concluded that there is insufficient evidence on the effectiveness to support or reject preventive therapy for treatment of contacts of patients with multidrug resistant tuberculosis (MDR-TB). Whether preventive therapy is favorable depends both on the effectiveness and the adverse events of the drugs used. We performed a systematic review to assess adverse events in healthy individuals and MDR-TB contacts treated with anti-tuberculosis drugs potentially effective for preventing development of MDR-TB. We searched MEDLINE, EMBASE, and other databases (August 2011). Record selection, data extraction, and study quality assessment were done in duplicate. The quality of evidence was assessed using the GRADE approach. Of 6,901 identified references, 20 studies were eligible. Among the 16 studies in healthy volunteers (a total of 87 persons on either levofloxacin, moxifloxacin, ofloxacin, or rifabutin, mostly for 1 week), serious adverse events and treatment discontinuation due to adverse events were rare (<1 and <5%, respectively), but mild adverse events frequently occurred. Due to small sample sizes of the levofloxacin and ofloxacin studies an increased frequency of mild adverse events compared to placebo could not be demonstrated or excluded. For moxifloxacin the comparative results were inconsistent. In four studies describing preventive therapy of MDR-TB contacts, therapy was stopped for 58-100% of the included persons because of the occurrence of adverse events ranging from mild adverse events such as nausea and dizziness to serious events requiring treatment. The quality of the evidence was very low. Although the number of publications and quality of evidence are low, the available evidence suggests that shortly after starting treatment the occurrence of serious adverse events is rare. Mild adverse events occur more frequently and may be of importance because these may provoke treatment interruption.
Conflict of interest statement
Figures
References
-
- World Health Organization (2010) Multidrug and extensively drug-resistant TB (M/XDR-TB): 2010 global report on surveillance and response. Geneva: WHO.
-
- Becerra MC, Appleton SC, Franke MF, Chalco K, Arteaga F, et al. (2011) Tuberculosis burden in households of patients with multidrug-resistant and extensively drug-resistant tuberculosis: a retrospective cohort study. Lancet 377 (9760) 147–152. - PubMed
-
- Kritski AL, Marques MJ, Rabahi MF, Vieira MA, Werneck-Barroso E, et al. (1996) Transmission of tuberculosis to close contacts of patients with multidrug-resistant tuberculosis. Am J Respir Crit Care Med 153 (1) 331–335. - PubMed
-
- Teixeira L, Perkins MD, Johnson JL, Keller R, Palaci M, et al. (2001) Infection and disease among household contacts of patients with multidrug-resistant tuberculosis. Int J Tuberc Lung Dis 5 (4) 321–328. - PubMed
-
- Grandjean L, Crossa A, Gilman RH, Herrera C, Bonilla C, et al. (2011) Tuberculosis in household contacts of multidrug-resistant tuberculosis patients. Int J Tuberc Lung Dis 15 (9) 1164–i, 1164-1269, i. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources