Comorbidities and mortality in hypercapnic obese under domiciliary noninvasive ventilation
- PMID: 23341888
- PMCID: PMC3547027
- DOI: 10.1371/journal.pone.0052006
Comorbidities and mortality in hypercapnic obese under domiciliary noninvasive ventilation
Abstract
Background: The higher mortality rate in untreated patients with obesity-associated hypoventilation is a strong rationale for long-term noninvasive ventilation (NIV). The impacts of comorbidities, medications and NIV compliance on survival of these patients remain largely unexplored.
Methods: Observational cohort of hypercapnic obese patients initiated on NIV between March 2003 and July 2008. Survival curves were estimated by the Kaplan-Meier method. Anthropometric measurements, pulmonary function, blood gases, nocturnal SpO(2) indices, comorbidities, medications, conditions of NIV initiation and NIV compliance were used as covariates. Univariate and multivariate Cox models allowed to assess predictive factors of mortality.
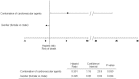
Results: One hundred and seven patients (56% women), in whom NIV was initiated in acute (36%) or chronic conditions, were followed during 43±14 months. The 1, 2, 3 years survival rates were 99%, 94%, and 89%, respectively. In univariate analysis, death was associated with older age (>61 years), low FEV1 (<66% predicted value), male gender, BMI×time, concomitant COPD, NIV initiation in acute condition, use of inhaled corticosteroids, ß-blockers, nonthiazide diuretics, angiotensin-converting enzyme inhibitors and combination of cardiovascular drugs (one diuretic and at least one other cardiovascular agent). In multivariate analysis, combination of cardiovascular agents was the only factor independently associated with higher risk of death (HR = 5.3; 95% CI 1.18; 23.9). Female gender was associated with lower risk of death.
Conclusion: Cardiovascular comorbidities represent the main factor predicting mortality in patient with obesity-associated hypoventilation treated by NIV. In this population, NIV should be associated with a combination of treatment modalities to reduce cardiovascular risk.
Conflict of interest statement
Figures


Similar articles
-
Prospective cross-sectional multicenter study on domiciliary noninvasive ventilation in stable hypercapnic COPD patients.Int J Chron Obstruct Pulmon Dis. 2018 Aug 10;13:2367-2374. doi: 10.2147/COPD.S164384. eCollection 2018. Int J Chron Obstruct Pulmon Dis. 2018. PMID: 30127600 Free PMC article.
-
Acute Respiratory Failure in Obesity-Hypoventilation Syndrome Managed in the ICU.Respir Care. 2019 Dec;64(12):1545-1554. doi: 10.4187/respcare.06901. Epub 2019 Sep 10. Respir Care. 2019. PMID: 31506342
-
Impact of noninvasive home ventilation on long-term survival in chronic hypercapnic COPD: a prospective observational study.Int J Clin Pract. 2007 Sep;61(9):1516-22. doi: 10.1111/j.1742-1241.2007.01427.x. Int J Clin Pract. 2007. PMID: 17686094
-
[Noninvasive ventilation in patients with persistent hypercapnia].Med Klin Intensivmed Notfmed. 2015 Apr;110(3):182-7. doi: 10.1007/s00063-014-0373-0. Epub 2014 Jun 19. Med Klin Intensivmed Notfmed. 2015. PMID: 24938398 Review. German.
-
Noninvasive Ventilation in the Critically Ill Patient With Obesity Hypoventilation Syndrome: A Review.J Intensive Care Med. 2017 Aug;32(7):421-428. doi: 10.1177/0885066616663179. Epub 2016 Aug 15. J Intensive Care Med. 2017. PMID: 27530511 Review.
Cited by
-
Obesity might be a good prognosis factor for COPD patients using domiciliary noninvasive mechanical ventilation.Int J Chron Obstruct Pulmon Dis. 2016 Aug 19;11:1895-901. doi: 10.2147/COPD.S108813. eCollection 2016. Int J Chron Obstruct Pulmon Dis. 2016. PMID: 27578969 Free PMC article.
-
Evaluation and Management of Obesity Hypoventilation Syndrome. An Official American Thoracic Society Clinical Practice Guideline.Am J Respir Crit Care Med. 2019 Aug 1;200(3):e6-e24. doi: 10.1164/rccm.201905-1071ST. Am J Respir Crit Care Med. 2019. PMID: 31368798 Free PMC article.
-
Long-Term Mortality following Acute Noninvasive Ventilation for Obesity-Related Respiratory Failure: A Retrospective Single-Centre Study.Can Respir J. 2023 Oct 12;2023:5370197. doi: 10.1155/2023/5370197. eCollection 2023. Can Respir J. 2023. PMID: 37868785 Free PMC article.
-
A history of home mechanical ventilation: The past, present and future.Chron Respir Dis. 2024 Jan-Dec;21:14799731241240776. doi: 10.1177/14799731241240776. Chron Respir Dis. 2024. PMID: 38512223 Free PMC article. Review.
-
Defining obesity hypoventilation syndrome.Breathe (Sheff). 2021 Sep;17(3):210089. doi: 10.1183/20734735.0089-2021. Breathe (Sheff). 2021. PMID: 35035556 Free PMC article. Review.
References
-
- Young T, Shahar E, Nieto FJ, Redline S, Newman AB, et al. (2002) Predictors of sleep-disordered breathing in community-dwelling adults: the Sleep Heart Health Study. Arch Intern Med 162: 893–900. - PubMed
-
- Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med 342: 1378–1384. - PubMed
-
- Sharma SK, Agrawal S, Damodaran D, Sreenivas V, Kadhiravan T, et al. (2011) CPAP for the metabolic syndrome in patients with obstructive sleep apnea. N Engl J Med 365: 2277–2286. - PubMed
-
- Nowbar S, Burkart KM, Gonzales R, Fedorowicz A, Gozansky WS, et al. (2004) Obesity-associated hypoventilation in hospitalized patients: prevalence, effects, and outcome. Am J Med 116: 1–7. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

