Evaluation of Xpert MTB/RIF and MODS assay for the diagnosis of pediatric tuberculosis
- PMID: 23343418
- PMCID: PMC3562258
- DOI: 10.1186/1471-2334-13-31
Evaluation of Xpert MTB/RIF and MODS assay for the diagnosis of pediatric tuberculosis
Abstract
Background: Tuberculosis (TB) in children is rarely confirmed due to the lack of effective diagnostic tools; only 10 to 15% of pediatric TB is smear positive due to paucibacillary samples and the difficulty of obtaining high-quality specimens from children. We evaluate here the accuracy of Xpert MTB/RIF in comparison with the Micoroscopic observation drug susceptibility (MODS) assay for diagnosis of TB in children using samples stored during a previously reported evaluation of the MODS assay.
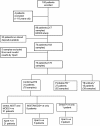
Methods: Ninety-six eligible children presenting with suspected TB were recruited consecutively at Pham Ngoc Thach Hospital in Ho Chi Minh City Viet Nam between May to December 2008 and tested by Ziehl-Neelsen smear, MODS and Mycobacterial growth Indicator (MGIT, Becton Dickinson) culture. All samples sent by the treating clinician for testing were included in the analysis. An aliquot of processed sample deposit was stored at -20°C and tested in the present study by Xpert MTB/RIF test. 183 samples from 73 children were available for analysis by Xpert. Accuracy measures of MODS and Xpert were summarized.
Results: The sensitivity (%) in detecting children with a clinical diagnosis of TB for smear, MODS and Xpert were 37.9 [95% CI 25.5; 51.6], 51.7 [38.2; 65.0] and 50.0 [36.6; 63.4], respectively (per patient analysis). Xpert was significantly more sensitive than smear (P=0.046). Testing of additional samples did not increase case detection for MODS while testing of a second sputum sample by Xpert detected only two additional cases. The positive and negative predictive values (%) of Xpert were 100.0 [88.0; 100.0] and 34.1 [20.5; 49.9], respectively, while those of MODS were 96.8 [83.3; 99.9] and 33.3 [19.6; 49.5].
Conclusion: MODS culture and Xpert MTB/RIF test have similar sensitivities for the detection of pediatric TB. Xpert MTB RIF is able to detect tuberculosis and rifampicin resistance within two hours. MODS allows isolation of cultures for further drug susceptibility testing but requires approximately one week to become positive. Testing of multiple samples by xpert detected only two additional cases and the benefits must be considered against costs in each setting. Further research is required to evaluate the optimal integration of Xpert into pediatric testing algorithms.
Figures
References
-
- Nelson LJ, Wells CD. Global epidemiology of childhood tuberculosis. Int J Tuberc Lung Dis. 2004;8(5):636–647. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical