Pancreatic β-cell dysfunction and risk of new-onset diabetes after kidney transplantation
- PMID: 23378624
- PMCID: PMC3687295
- DOI: 10.2337/dc12-1894
Pancreatic β-cell dysfunction and risk of new-onset diabetes after kidney transplantation
Abstract
Objective: Chronic exposure to calcineurin inhibitors and corticosteroids poses renal transplant recipients (RTR) at high risk for development of new-onset diabetes after transplantation (NODAT). Pancreatic β-cell dysfunction may be crucial to the pathophysiology of NODAT and specific markers for β-cell dysfunction may have additive value for predicting NODAT in this population. Therefore, we prospectively investigated whether proinsulin, as a marker of pancreatic β-cell dysfunction, is associated with future development of NODAT and improves prediction of it.
Research design and methods: All RTR between 2001 and 2003 with a functioning graft for ≥1 year were considered eligible for inclusion, except for subjects with diabetes at baseline who were excluded. We recorded incidence of NODAT until April 2012.
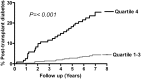
Results: A total of 487 RTR (age 50 ± 12 years, 55% men) participated at a median time of 6.0 (interquartile range [IQR], 2.6-11.5) years after transplantation. Median fasting proinsulin levels were 16.6 (IQR, 11.0-24.2) pmol/L. During median follow-up for 10.1 (IQR, 9.1-10.4) years, 42 (35%) RTR had development of NODAT in the highest quartile of the distribution of proinsulin versus 34 (9%) in the lowest three quartiles (P < 0.001). In Cox regression analyses, proinsulin (hazard ratio, 2.29; 95% CI, 1.85-2.83; P < 0.001) was strongly associated with NODAT development. This was independent of age, sex, calcineurine inhibitors, prednisolone use, components of the metabolic syndrome, or homeostasis model assessment.
Conclusions: In conclusion, fasting proinsulin is strongly associated with NODAT development in RTR. Our results highlight the role of β-cell dysfunction in the pathophysiology of NODAT and indicate the potential value of proinsulin for identification of RTR at increased risk for NODAT.
Figures
Similar articles
-
Remnant lipoprotein cholesterol is associated with incident new onset diabetes after transplantation (NODAT) in renal transplant recipients: results of the TransplantLines Biobank and cohort Studies.Cardiovasc Diabetol. 2022 Mar 16;21(1):41. doi: 10.1186/s12933-022-01475-y. Cardiovasc Diabetol. 2022. PMID: 35296331 Free PMC article.
-
Role of insulin resistance indices in predicting new-onset diabetes after kidney transplantation.Transpl Int. 2013 Mar;26(3):273-80. doi: 10.1111/tri.12026. Epub 2012 Dec 11. Transpl Int. 2013. PMID: 23230898 Clinical Trial.
-
Plasma Malondialdehyde and Risk of New-Onset Diabetes after Transplantation in Renal Transplant Recipients: A Prospective Cohort Study.J Clin Med. 2019 Apr 4;8(4):453. doi: 10.3390/jcm8040453. J Clin Med. 2019. PMID: 30987358 Free PMC article.
-
Can new-onset diabetes after kidney transplant be prevented?Diabetes Care. 2013 May;36(5):1406-12. doi: 10.2337/dc12-2067. Diabetes Care. 2013. PMID: 23613600 Free PMC article. Review.
-
New onset of diabetes after transplantation - an overview of epidemiology, mechanism of development and diagnosis.Transpl Immunol. 2014 Jan;30(1):52-8. doi: 10.1016/j.trim.2013.10.006. Epub 2013 Oct 29. Transpl Immunol. 2014. PMID: 24184293 Review.
Cited by
-
New-Onset Diabetes Mellitus after Kidney Transplantation.J Clin Med. 2024 Mar 27;13(7):1928. doi: 10.3390/jcm13071928. J Clin Med. 2024. PMID: 38610694 Free PMC article. Review.
-
Managing Post-Transplant Diabetes Mellitus after Kidney Transplantation: Challenges and Advances in Treatment.Pharmaceuticals (Basel). 2024 Jul 26;17(8):987. doi: 10.3390/ph17080987. Pharmaceuticals (Basel). 2024. PMID: 39204092 Free PMC article. Review.
-
Genetics of new-onset diabetes after transplantation.J Am Soc Nephrol. 2014 May;25(5):1037-49. doi: 10.1681/ASN.2013040383. Epub 2013 Dec 5. J Am Soc Nephrol. 2014. PMID: 24309190 Free PMC article.
-
Glucometabolism in Kidney Transplant Recipients with and without Posttransplant Diabetes: Focus on Beta-Cell Function.Biomedicines. 2024 Jan 30;12(2):317. doi: 10.3390/biomedicines12020317. Biomedicines. 2024. PMID: 38397919 Free PMC article.
-
Fasting Proinsulin Independently Predicts Incident Type 2 Diabetes in the General Population.J Pers Med. 2022 Jul 12;12(7):1131. doi: 10.3390/jpm12071131. J Pers Med. 2022. PMID: 35887628 Free PMC article.
References
-
- Kuypers DR, Claes K, Bammens B, Evenepoel P, Vanrenterghem Y. Early clinical assessment of glucose metabolism in renal allograft recipients: diagnosis and prediction of post-transplant diabetes mellitus (PTDM). Nephrol Dial Transplant 2008;23:2033–2042 - PubMed
-
- Chadban S. New-onset diabetes after transplantation—should it be a factor in choosing an immunosuppressant regimen for kidney transplant recipients. Nephrol Dial Transplant 2008;23:1816–1818 - PubMed
-
- Kasiske BL, Snyder JJ, Gilbertson D, Matas AJ. Diabetes mellitus after kidney transplantation in the United States. Am J Transplant 2003;3:178–185 - PubMed
-
- Bee YM, Tan HC, Tay TL, Kee TY, Goh SY, Kek PC. Incidence and risk factors for development of new-onset diabetes after kidney transplantation. Ann Acad Med Singapore 2011;40:160–167 - PubMed
-
- Pfützner A, Pfützner AH, Larbig M, Forst T. Role of intact proinsulin in diagnosis and treatment of type 2 diabetes mellitus. Diabetes Technol Ther 2004;6:405–412 - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous