Use of dietary linoleic acid for secondary prevention of coronary heart disease and death: evaluation of recovered data from the Sydney Diet Heart Study and updated meta-analysis
- PMID: 23386268
- PMCID: PMC4688426
- DOI: 10.1136/bmj.e8707
Use of dietary linoleic acid for secondary prevention of coronary heart disease and death: evaluation of recovered data from the Sydney Diet Heart Study and updated meta-analysis
Erratum in
- BMJ. 2013;346:f903
Abstract
Objective: To evaluate the effectiveness of replacing dietary saturated fat with omega 6 linoleic acid, for the secondary prevention of coronary heart disease and death.
Design: Evaluation of recovered data from the Sydney Diet Heart Study, a single blinded, parallel group, randomized controlled trial conducted in 1966-73; and an updated meta-analysis including these previously missing data.
Setting: Ambulatory, coronary care clinic in Sydney, Australia.
Participants: 458 men aged 30-59 years with a recent coronary event.
Interventions: Replacement of dietary saturated fats (from animal fats, common margarines, and shortenings) with omega 6 linoleic acid (from safflower oil and safflower oil polyunsaturated margarine). Controls received no specific dietary instruction or study foods. All non-dietary aspects were designed to be equivalent in both groups.
Outcome measures: All cause mortality (primary outcome), cardiovascular mortality, and mortality from coronary heart disease (secondary outcomes). We used an intention to treat, survival analysis approach to compare mortality outcomes by group.
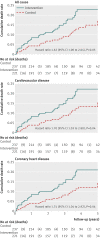
Results: The intervention group (n=221) had higher rates of death than controls (n=237) (all cause 17.6% v 11.8%, hazard ratio 1.62 (95% confidence interval 1.00 to 2.64), P=0.05; cardiovascular disease 17.2% v 11.0%, 1.70 (1.03 to 2.80), P=0.04; coronary heart disease 16.3% v 10.1%, 1.74 (1.04 to 2.92), P=0.04). Inclusion of these recovered data in an updated meta-analysis of linoleic acid intervention trials showed non-significant trends toward increased risks of death from coronary heart disease (hazard ratio 1.33 (0.99 to 1.79); P=0.06) and cardiovascular disease (1.27 (0.98 to 1.65); P=0.07).
Conclusions: Advice to substitute polyunsaturated fats for saturated fats is a key component of worldwide dietary guidelines for coronary heart disease risk reduction. However, clinical benefits of the most abundant polyunsaturated fatty acid, omega 6 linoleic acid, have not been established. In this cohort, substituting dietary linoleic acid in place of saturated fats increased the rates of death from all causes, coronary heart disease, and cardiovascular disease. An updated meta-analysis of linoleic acid intervention trials showed no evidence of cardiovascular benefit. These findings could have important implications for worldwide dietary advice to substitute omega 6 linoleic acid, or polyunsaturated fats in general, for saturated fats.
Trial registration: Clinical trials NCT01621087.
Conflict of interest statement
Competing interests: All authors have completed the ICMJE uniform disclosure form at
Figures



Comment in
-
Old study sheds new light on the fatty acids and cardiovascular health debate.BMJ. 2013 Feb 4;346:f493. doi: 10.1136/bmj.f493. BMJ. 2013. PMID: 23386269 No abstract available.
-
ACP Journal Club. Review: replacing dietary saturated fatty acids with n-6 polyunsaturated fatty acids does not reduce mortality.Ann Intern Med. 2013 May 21;158(10):JC6. doi: 10.7326/0003-4819-158-10-201305210-02006. Ann Intern Med. 2013. PMID: 23689785 No abstract available.
-
[Linoleic acid and heart infarct].Ned Tijdschr Geneeskd. 2013;157(22):A6290. Ned Tijdschr Geneeskd. 2013. PMID: 23714298 Dutch.
References
-
- Dietary fat and its relation to heart attacks and strokes. Report by the Central Committee for Medical and Community Program of the American Heart Association. JAMA 1961;175:389-91. - PubMed
-
- Keys A, Anderson JT, Grande F. Serum cholesterol response to changes in diet: iodine value of dietary fat versus 2S-P. Metab Clin Exptl 1965;14:747-58. - PubMed
-
- De Caterina R. n-3 fatty acids in cardiovascular disease. N Engl J Med 2011;364:2439-50. - PubMed
-
- Dietary supplementation with n-3 polyunsaturated fatty acids and vitamin E after myocardial infarction: results of the GISSI-Prevenzione trial. Gruppo Italiano per lo Studio della Sopravvivenza nell’Infarto miocardico. Lancet 1999;354:447-55. - PubMed
-
- Yokoyama M, Origasa H, Matsuzaki M, Matsuzawa Y, Saito Y, Ishikawa Y, et al. Effects of eicosapentaenoic acid on major coronary events in hypercholesterolaemic patients (JELIS): a randomised open-label, blinded endpoint analysis. Lancet 2007;369:1090-8. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
