One-year assessment of surgical outcomes in Class III patients using cone beam computed tomography
- PMID: 23403336
- PMCID: PMC3970766
- DOI: 10.1016/j.ijom.2013.01.002
One-year assessment of surgical outcomes in Class III patients using cone beam computed tomography
Abstract
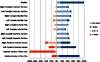
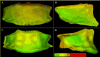
The purpose of this study was to apply a novel method to evaluate surgical outcomes at 1 year after orthognathic surgery for Class III patients undergoing two different surgical protocols. Fifty patients divided equally into two groups (maxillary advancement only and combined with mandibular setback) had cone beam computed tomography (CBCT) scans taken pre-surgery, at splint removal, and at 1-year post-surgery. An automatic cranial base superimposition method was used to register, and shape correspondence was applied to assess, the overall changes between pre-surgery and splint removal (surgical changes) and between splint removal and 1-year post-surgery at the end of orthodontic treatment (post-surgical adaptations). Post-surgical maxillary adaptations were exactly the same for both groups, with 52% of the patients having changes >2mm. Approximately half of the post-surgical changes in the maxilla for both groups were vertical. The two-jaw group showed significantly greater surgical and post-surgical changes in the ramus, chin, and most of the condylar surfaces (P<0.05). Post-surgical adaptation on the anterior part of the chin was also more significant in the two-jaw group (P<0.05). Regardless of the type of surgery, marked post-surgical adaptations were observed in the regions evaluated, which explain the adequate maxillary-mandibular relationship at 1-year post-surgery on average, with individual variability.
Copyright © 2013 International Association of Oral and Maxillofacial Surgeons. All rights reserved.
Figures









References
-
- Proffit WR, Phillips C, Prewitt JW, Turvey TA. Stability after surgical–orthodontic correction of skeletal Class III malocclusion. 2. Maxillary advancement. Int J Adult Orthodon Orthognath Surg. 1991;6:71–80. - PubMed
-
- Proffit WR, Phillips C, Turvey TA. Stability after surgical–orthodontic corrective of skeletal Class III malocclusion. 3. Combined maxillary and mandibular procedures. Int J Adult Orthodon Orthognath Surg. 1991;6:211–225. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

