Changes in seroadaptive practices from before to after diagnosis of recent HIV infection among men who have sex with men
- PMID: 23405145
- PMCID: PMC3566177
- DOI: 10.1371/journal.pone.0055397
Changes in seroadaptive practices from before to after diagnosis of recent HIV infection among men who have sex with men
Abstract
Objective: We assessed changes in sexual behavior among men who have sex with men (MSM), before and for several years after HIV diagnosis, accounting for adoption of a variety of seroadaptive practices.
Methods: We collected self-reported sexual behavior data every 3 months from HIV-positive MSM at various stages of HIV infection. To establish population level trends in sexual behavior, we used negative binomial regression to model the relationship between time since diagnosis and several sexual behavior variables: numbers of (a) total partners, (b) potentially discordant partners (PDP; i.e., HIV-negative or unknown-status partners), (c) PDPs with whom unprotected anal intercourse (UAI) occurred, and (d) PDPs with whom unprotected insertive anal intercourse (uIAI) occurred.
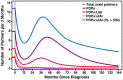
Results: A total of 237 HIV-positive MSM contributed 502 interviews. UAI with PDPs occurred with a mean of 4.2 partners in the 3 months before diagnosis. This declined to 0.9 partners/3 months at 12 months after diagnosis, and subsequently rose to 1.7 partners/3 months at 48 months, before falling again to 1.0 partners/3 months at 60 months. The number of PDPs with whom uIAI occurred dropped from 2.4 in the pre-diagnosis period to 0.3 partners/3 months (an 87.5% reduction) by 12 months after enrollment, and continued to decline over time.
Conclusion: Within months after being diagnosed with HIV, MSM adopted seroadaptive practices, especially seropositioning, where the HIV-positive partner was not in the insertive position during UAI, resulting in a sustained decline in the sexual activity associated with the highest risk of HIV transmission.
Conflict of interest statement
Figures
References
-
- Gates, G. How many people are lesbian, gay, bisexual, and transgender? Available: http://williamsinstitute.law.ucla.edu/wp-content/uploads/Gates-How-Many-.... Accessed February 16 2012.
-
- Aidala AA, Lee G, Garbers S, Chiasson MA (2006) Sexual behaviors and sexual risk in a prospective cohort of HIV-positive men and women in New York City, 1994–2002: implications for prevention. AIDS Educ Prev 18: 12–32. - PubMed
-
- Bachmann LH, Grimley DM, Waithaka Y, Desmond R, Saag MS, et al. (2005) Sexually transmitted disease/HIV transmission risk behaviors and sexually transmitted disease prevalence among HIV-positive men receiving continuing care. Sex Transm Dis 32: 20–26. - PubMed
-
- Colfax GN, Buchbinder SP, Cornelisse PG, Vittinghoff E, Mayer K, et al. (2002) Sexual risk behaviors and implications for secondary HIV transmission during and after HIV seroconversion. AIDS 16: 1529–1535. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

