Left ventricular global function index by magnetic resonance imaging--a novel marker for assessment of cardiac performance for the prediction of cardiovascular events: the multi-ethnic study of atherosclerosis
- PMID: 23424238
- PMCID: PMC3691067
- DOI: 10.1161/HYPERTENSIONAHA.111.198028
Left ventricular global function index by magnetic resonance imaging--a novel marker for assessment of cardiac performance for the prediction of cardiovascular events: the multi-ethnic study of atherosclerosis
Abstract
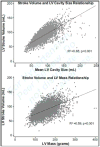
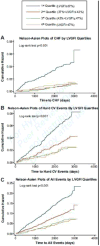
Left ventricular (LV) function is generally assessed independent of structural remodeling and vice versa. The purpose of this study was to evaluate a novel LV global function index (LVGFI) that integrates LV structure with global function and to assess its predictive value for cardiovascular (CV) events throughout adult life in a multiethnic population of men and women without history of CV diseases at baseline. A total of 5004 participants in the Multi-Ethnic Study of Atherosclerosis underwent a cardiac magnetic resonance study and were followed up for a median of 7.2 years. The LVGFI by cardiac magnetic resonance was defined by the ratio of stroke volume divided by LV total volume defined as the sum of mean LV cavity and myocardial volumes. Cox proportional hazard models were constructed to predict the end points of heart failure, hard CV events, and a combined end point of all CV events after adjustment for established risk factors, calcium score, and biomarkers. A total of 579 (11.6%) CV events were observed during the follow-up period. In adjusted models, the end points of heart failure, hard CV events, and all events were all significantly associated with LVGFI (heart failure, hazard ratio=0.64, P<0.0001; hard CV events, hazard ratio=0.79, P=0.007; all events, hazard ratio=0.79, P<0.0001). LVGFI had a significant independent predictive value in the multivariable models for all CV event categories. The LVGFI was a powerful predictor of incident HF, hard CV events, and a composite end point, including all events in this multiethnic cohort.
Figures




Comment in
-
Prognostic importance of a new measure of global systolic heart function in healthy adults.Hypertension. 2013 Apr;61(4):762-4. doi: 10.1161/HYPERTENSIONAHA.112.199992. Epub 2013 Feb 19. Hypertension. 2013. PMID: 23424234 No abstract available.
References
-
- Gaasch WH, Zile MR. Left ventricular structural remodeling in health and disease with special emphasis on volume, mass, and geometry. J Am Coll Cardiol. 2011;58:1733–1740. - PubMed
-
- Gjesdal O, Bluemke DA, Lima JA. Cardiac remodeling at the population level--risk factors, screening, and outcomes. Nat Rev Cardiol. 2011;8:673–685. - PubMed
-
- Pfeffer MA, Braunwald E, Moyé LA, Basta L, Brown EJ, Cuddy TE, Davis BR, Geltman EM, Goldman S, Flaker GC, Klein M, Lamas GA, Packer M, Rouleau J, Rouleau JL, Rutherford J, Wertheimer JH, Hawkins M. Effect of enalapril on mortality and the development of heart failure in asymptomatic patients with reduced left ventricular ejection fractions. The SOLVD Investigators. N Engl J Med. 1992;327:685–691. - PubMed
-
- Pfeffer MA, Braunwald E, Moye LA, Basta L, Brown EJJ, Cuddy TE, Davis BR, Geltman EM, Goldman S, Flaker GC, Klein M, Lamas GA, Packer M, Rouleau J, Rouleau JL, Rutherford J, Wertheimer JH, Hawkins CM. Effect of captopril on mortality and morbidity in patients with left ventricular dysfunction after myocardial infarction. Results of the survival and ventricular enlargement trial. The SAVE Investigators. N Engl J Med. 1992;327:669–677. - PubMed
-
- Cygankiewicz I, Zareba W, Vazquez R, Bayes-Genis A, Pascual D, Macaya C, Almendral J, Fiol M, Bardaji A, Gonzalez-Juanatey JR, Nieto V, Valdes M, Cinca J, de Luna AB. Risk stratification of mortality in patients with heart failure and left ventricular ejection fraction >35% Am J Cardiol. 2009;103:1003–1010. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Molecular Biology Databases
Research Materials
Miscellaneous

