Cytokines in the systemic inflammatory response syndrome: a review
- PMID: 23441054
- PMCID: PMC3484588
Cytokines in the systemic inflammatory response syndrome: a review
Abstract
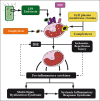
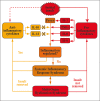
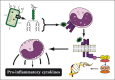
Introduction: Patients subject to major surgery, suffering sepsis, major trauma, or following cardiopulmonary bypass exhibit a systemic inflammatory response. This inflammatory response involves a complex array of inflammatory polypeptide molecules known as cytokines. It is well accepted that the loss of local control of the release of these cytokines leads to systemic inflammation and potentially deleterious consequences including the Systemic Inflammatory Response Syndrome, Multi-Organ Dysfunction Syndrome, shock and death.
Methods: The Medline database was searched for literature on mechanisms involved in the development of SIRS and potential targets for modifying the inflammatory response. We focus on the novel therapy of cytokine adsorption as a promising removal technology.
Results: Accumulating data from human studies and experimental animal models suggests that both pro- and anti- inflammatory cytokines are released following a variety of initiating stimuli including endotoxin release, complement activation, ischaemia reperfusion injury and others.
Discussion: Pro-and anti-inflammatory cytokines interact in a complex and unpredictable manner to influence the immune system and eventually cause multiple end organ effects. Cytokine adsorption therapy provides a potential solution to improving outcomes following Systemic Inflammatory Response Syndrome.
Keywords: SIRS; cytokine; inflammatory response; syndrome; systemic.
Conflict of interest statement
Figures

Similar articles
-
Systemic inflammation after trauma.Injury. 2007 Dec;38(12):1336-45. doi: 10.1016/j.injury.2007.10.003. Epub 2007 Nov 28. Injury. 2007. PMID: 18048040 Review.
-
[The importance of cytokines in the posttraumatic inflammatory reaction].Unfallchirurg. 2005 Oct;108(10):793-4, 796-803. doi: 10.1007/s00113-005-1005-1. Unfallchirurg. 2005. PMID: 16175346 Review. German.
-
Minimizing systemic inflammation during cardiopulmonary bypass in the pediatric population.Artif Organs. 2014 Jan;38(1):11-8. doi: 10.1111/aor.12195. Epub 2013 Oct 31. Artif Organs. 2014. PMID: 24392866 Review.
-
Controlling the complement system in inflammation.Immunopharmacology. 1997 Dec;38(1-2):51-62. doi: 10.1016/s0162-3109(97)00057-x. Immunopharmacology. 1997. PMID: 9476114 Review.
-
Treatment of post-cardiopulmonary bypass SIRS by hemoadsorption: a case series.Int J Artif Organs. 2016 May 16;39(3):141-6. doi: 10.5301/ijao.5000492. Epub 2016 Apr 25. Int J Artif Organs. 2016. PMID: 27140295
Cited by
-
Traumatic inflammatory response: pathophysiological role and clinical value of cytokines.Eur J Trauma Emerg Surg. 2024 Aug;50(4):1313-1330. doi: 10.1007/s00068-023-02388-5. Epub 2023 Dec 27. Eur J Trauma Emerg Surg. 2024. PMID: 38151578 Free PMC article. Review.
-
Thromboelastometry profile in critically ill patients: A single-center, retrospective, observational study.PLoS One. 2018 Feb 20;13(2):e0192965. doi: 10.1371/journal.pone.0192965. eCollection 2018. PLoS One. 2018. PMID: 29462165 Free PMC article.
-
Evaluation of Inflammation Caused by Cardiopulmonary Bypass in a Small Animal Model.Biology (Basel). 2020 Apr 20;9(4):81. doi: 10.3390/biology9040081. Biology (Basel). 2020. PMID: 32326072 Free PMC article. Review.
-
Regulation of immune responses to infection through interaction between stem cell-derived exosomes and toll-like receptors mediated by microRNA cargoes.Front Cell Infect Microbiol. 2024 May 2;14:1384420. doi: 10.3389/fcimb.2024.1384420. eCollection 2024. Front Cell Infect Microbiol. 2024. PMID: 38756232 Free PMC article. Review.
-
Mitochondrial dysfunction in rat splenocytes following hemorrhagic shock.Biochim Biophys Acta Mol Basis Dis. 2017 Oct;1863(10 Pt B):2526-2533. doi: 10.1016/j.bbadis.2017.08.024. Epub 2017 Aug 26. Biochim Biophys Acta Mol Basis Dis. 2017. PMID: 28844961 Free PMC article.
References
-
- Bone RC, Balk RA, Cerra FB. et al. Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest. 1992;101:1644–1655. - PubMed
-
- Bone RC. Immunologic dissonance: a continuing evolution in our understanding of the systemic inflammatory response syndrome (SIRS) and the multiple organ dysfunction syndrome (MODS) Ann Intern Med. 1996;125:680–687. - PubMed
-
- Salvo I, De Cian W, Musicco M. et al. The Italian SEPSIS study: preliminary results on the incidence and evolution of SIRS, sepsis, severe sepsis and septic shock. Intensive Care Med. 1995;2:S244–S249. - PubMed
-
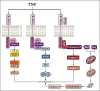
- Wajant H, Pfizenmaier K, Scheurich P. Tumor necrosis factor signaling. Cell Death Differ. 2003;10:45–65. - PubMed
-
- Willatts S M, Speller DC, Winter RJ. Incidence of gram-negative bacteraemia in sepsis syndrome. Implications for immunotherapy. Anaesthesia. 1994;49:751–754. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
