Bariatric surgery complications before vs after implementation of a national policy restricting coverage to centers of excellence
- PMID: 23443442
- PMCID: PMC3785293
- DOI: 10.1001/jama.2013.755
Bariatric surgery complications before vs after implementation of a national policy restricting coverage to centers of excellence
Abstract
Importance: Starting in 2006, the Centers for Medicare & Medicaid Services (CMS) has restricted coverage of bariatric surgery to hospitals designated as centers of excellence (COE) by 2 major professional organizations.
Objective: To evaluate whether the implementation of the COE component of the national coverage decision was associated with improved bariatric surgery outcomes in Medicare patients.
Design, setting, and patients: Retrospective, longitudinal study using 2004-2009 hospital discharge data from 12 states (n = 321,464 patients) of changes in outcomes in Medicare patients undergoing bariatric surgery (n = 6723 before and n = 15,854 after implementation of the policy). A difference-in-differences analytic approach was used to evaluate whether the national coverage decision was associated with improved outcomes in Medicare patients above and beyond existing time trends in non-Medicare patients (n = 95,558 before and n = 155,117 after implementation of the policy).
Main outcome measures: Risk-adjusted rates of any complication, serious complications, and reoperation.
Results: Bariatric surgery outcomes improved during the study period in both Medicare and non-Medicare patients; however, this change was already under way prior to the CMS coverage decision. After accounting for patient factors, changes in procedure type, and preexisting time trends toward improved outcomes, there were no statistically significant improvements in outcomes after (vs before) implementation of the CMS national coverage decision for any complication (8.0% after vs 7.0% before; relative risk [RR], 1.14 [95% CI, 0.95-1.33]), serious complications (3.3% vs 3.6%, respectively; RR, 0.92 [95% CI, 0.62-1.22]), and reoperation (1.0% vs 1.1%; RR, 0.90 [95% CI, 0.64-1.17]). In a direct assessment comparing outcomes at hospitals designated as COEs (n = 179) vs hospitals without the COE designation (n = 519), no significant differences were found for any complication (5.5% vs 6.0%, respectively; RR, 0.98 [95% CI, 0.90-1.06]), serious complications (2.2% vs 2.5%; RR, 0.92 [95% CI, 0.84-1.00]), and reoperation (0.83% vs 0.96%; RR, 1.00 [95% CI, 0.86-1.17]).
Conclusions and relevance: Among Medicare patients undergoing bariatric surgery, there was no significant difference in the rates of complications and reoperation before vs after the CMS policy of restricting coverage to COEs. Combined with prior studies showing no association of COE designation and outcomes, these results suggest that Medicare should reconsider this policy.
Conflict of interest statement
Figures
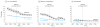
Comment in
-
Promoting quality surgical care: the next steps.JAMA. 2013 Feb 27;309(8):827-8. doi: 10.1001/jama.2013.1503. JAMA. 2013. PMID: 23443448 No abstract available.
-
Letter to the editor: Response to JAMA article which did not accept these letters delineating numerous problems with the published study.Surg Obes Relat Dis. 2013 Sep-Oct;9(5):831. doi: 10.1016/j.soard.2013.06.002. Epub 2013 Jun 6. Surg Obes Relat Dis. 2013. PMID: 24079903 No abstract available.
References
-
- Flum DR, Salem L, Elrod JA, Dellinger EP, Cheadle A, Chan L. Early mortality among Medicare beneficiaries undergoing bariatric surgical procedures. JAMA. 2005;294:1903–8. - PubMed
-
- Pratt GM, McLees B, Pories WJ. The ASBS Bariatric Surgery Centers of Excellence program: a blueprint for quality improvement. Surg Obes Relat Dis. 2006;2:497–503. discussion. - PubMed
-
- Hollenbeak CS, Rogers AM, Barrus B, Wadiwala I, Cooney RN. Surgical volume impacts bariatric surgery mortality: a case for centers of excellence. Surgery. 2008;144:736–43. - PubMed
-
- Schirmer B, Jones DB. The American College of Surgeons Bariatric Surgery Center Network: establishing standards. Bull Am Coll Surg. 2007;92:21–7. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

