Brain-reactive antibodies and disease
- PMID: 23516983
- PMCID: PMC4401150
- DOI: 10.1146/annurev-immunol-020711-075041
Brain-reactive antibodies and disease
Abstract
Autoimmune diseases currently affect 5-7% of the world's population; in most diseases there are circulating autoantibodies. Brain-reactive antibodies are present in approximately 2-3% of the general population but do not usually contribute to brain pathology. These antibodies penetrate brain tissue only early in development or under pathologic conditions. This restriction on their pathogenicity and the lack of correlation between serum titers and brain pathology have, no doubt, contributed to a delayed appreciation of the contribution of autoantibodies in diseases of the central nervous system. Nonetheless, it is increasingly clear that antibodies can cause damage in the brain and likely initiate or aggravate multiple neurologic conditions; brain-reactive antibodies contribute to symptomatology in autoimmune disease, infectious disease, and malignancy.
Figures
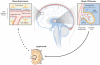

References
-
- Kowal C, DeGiorgio LA, Nakaoka T, Hetherington H, Huerta PT, et al. Cognition and immunity; antibody impairs memory. Immunity. 2004;21:179–88. - PubMed
-
- Berer K, Mues M, Koutrolos M, Rasbi ZA, Boziki M, et al. Commensal microbiota and myelin autoantigen cooperate to trigger autoimmune demyelination. Nature. 2011;479:538–41. - PubMed
-
- Meinl E, Krumbholz M, Hohlfeld R. B lineage cells in the inflammatory central nervous system environment: migration, maintenance, local antibody production, and therapeutic modulation. Ann. Neurol. 2006;59(6):880–92. - PubMed
-
- Galea I, Bechmann I, Perry VH. What is immune privilege (not)? Trends Immunol. 2007;28:12–18. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

