Combined serological, genetic, and inflammatory markers differentiate non-IBD, Crohn's disease, and ulcerative colitis patients
- PMID: 23518807
- PMCID: PMC3792797
- DOI: 10.1097/MIB.0b013e318280b19e
Combined serological, genetic, and inflammatory markers differentiate non-IBD, Crohn's disease, and ulcerative colitis patients
Abstract
Background: Previous studies have demonstrated that serological markers can assist in diagnosing inflammatory bowel disease (IBD). In this study, we aim to build a diagnostic tool incorporating serological markers, genetic variants, and markers of inflammation into a computational algorithm to examine patterns of combinations of markers to (1) identify patients with IBD and (2) differentiate patients with Crohn's disease (CD) from ulcerative colitis (UC).
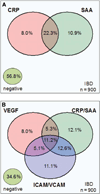
Methods: In this cross-sectional study, patient blood samples from 572 CD, 328 UC, 437 non-IBD controls, and 183 healthy controls from academic and community centers were analyzed for 17 markers: 8 serological markers (ASCA-IgA, ASCA-IgG, ANCA, pANCA, OmpC, CBir1, A4-Fla2, and FlaX), 4 genetic markers (ATG16L1, NKX2-3, ECM1, and STAT3), and 5 inflammatory markers (CRP, SAA, ICAM-1, VCAM-1, and VEGF). A diagnostic Random Forest algorithm was constructed to classify IBD, CD, and UC.
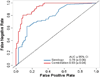
Results: Receiver operating characteristic analysis compared the diagnostic accuracy of using a panel of serological markers only (ASCA-IgA, ASCA-IgG, ANCA, pANCA, OmpC, and CBir1) versus using a marker panel that in addition to the serological markers mentioned above also included gene variants, inflammatory markers, and 2 additional serological markers (A4-Fla2 and FlaX). The extended marker panel increased the IBD versus non-IBD discrimination area under the curve from 0.80 (95% confidence interval [CI], ±0.05) to 0.87 (95% CI, ±0.04; P < 0.001). The CD versus UC discrimination increased from 0.78 (95% CI, ±0.06) to 0.93 (95% CI, ±0.04; P < 0.001).
Conclusions: Incorporating a combination of serological, genetic, and inflammation markers into a diagnostic algorithm improved the accuracy of identifying IBD and differentiating CD from UC versus using serological markers alone.
Figures



References
-
- Bossuyt X. Serologic markers in inflammatory bowel disease. Clin Chem. 2006;57:171–181. - PubMed
-
- Targan SR, Landers CJ, Yang H, et al. Antibodies to CBir1 flagellin define a unique response that is associated independently with complicated Crohn’s disease. Gastroenterology. 2005;128:2020–2028. - PubMed
-
- Landers CJ, Cohavy O, Misra R, et al. Selected loss of tolerance evidenced by Crohn’s disease-associated immune responses to auto- and microbial antigens. Gastroenterology. 2002;123:689–699. - PubMed
-
- McGuckin MA, Eri R, Simms LA, et al. Intestinal barrier dysfunction in inflammatory bowel diseases. Inflamm Bowel Dis. 2009;15:100–113. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous
