Increased brain white matter axial diffusivity associated with fatigue, pain and hyperalgesia in Gulf War illness
- PMID: 23526988
- PMCID: PMC3603990
- DOI: 10.1371/journal.pone.0058493
Increased brain white matter axial diffusivity associated with fatigue, pain and hyperalgesia in Gulf War illness
Abstract
Background: Gulf War exposures in 1990 and 1991 have caused 25% to 30% of deployed personnel to develop a syndrome of chronic fatigue, pain, hyperalgesia, cognitive and affective dysfunction.
Methods: Gulf War veterans (n = 31) and sedentary veteran and civilian controls (n = 20) completed fMRI scans for diffusion tensor imaging. A combination of dolorimetry, subjective reports of pain and fatigue were correlated to white matter diffusivity properties to identify tracts associated with symptom constructs.
Results: Gulf War Illness subjects had significantly correlated fatigue, pain, hyperalgesia, and increased axial diffusivity in the right inferior fronto-occipital fasciculus. ROC generated thresholds and subsequent binary regression analysis predicted CMI classification based upon axial diffusivity in the right inferior fronto-occipital fasciculus. These correlates were absent for controls in dichotomous regression analysis.
Conclusion: The right inferior fronto-occipital fasciculus may be a potential biomarker for Gulf War Illness. This tract links cortical regions involved in fatigue, pain, emotional and reward processing, and the right ventral attention network in cognition. The axonal neuropathological mechanism(s) explaining increased axial diffusivity may account for the most prominent symptoms of Gulf War Illness.
Conflict of interest statement
Figures

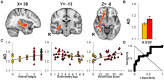


References
-
- RAC-GWVI: The Research Advisory Committee on Gulf War Veterans’ Illnesses (2008) Gulf War Illness and the Health of Gulf War Veterans. Washington, DC: U.S. Government Printing Office.
-
- Fukuda K, Nisenbaum R, Stewart G, Thompson WW, Robin L, et al. (1998) Chronic multisymptom illness affecting Air Force veterans of the Gulf War. JAMA 280: 981–988. - PubMed
-
- Kang HK, Li B, Mahan CM, Eisen SA, Engel CC (2009) Health of US veterans of 1991 Gulf War: a follow-up survey in 10 years. J Occup Environ Med. 4: 401–410. - PubMed
-
- Fukuda K, Straus SE, Hickie I, Sharpe MC, Dobbins JG, et al. (1994) The chronic fatigue syndrome: a comprehensive approach to its definition and study International Chronic Fatigue Syndrome Study Group. Ann Intern Med. 12: 953–959. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

