Perineural mast cells are specifically enriched in pancreatic neuritis and neuropathic pain in pancreatic cancer and chronic pancreatitis
- PMID: 23555989
- PMCID: PMC3610867
- DOI: 10.1371/journal.pone.0060529
Perineural mast cells are specifically enriched in pancreatic neuritis and neuropathic pain in pancreatic cancer and chronic pancreatitis
Abstract
Background: Pancreatic neuritis is a histopathological hallmark of pancreatic neuropathy and correlates to abdominal neuropathic pain sensation in pancreatic adenocarcinoma (PCa) and chronic pancreatitis (CP). However, inflammatory cell subtypes that compose pancreatic neuritis and their correlation to the neuropathic pain syndrome in PCa and CP are yet unknown.
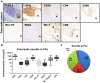
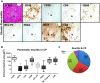
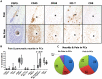
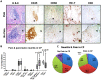
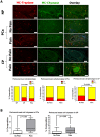
Methods: Inflammatory cells within pancreatic neuritis lesions of patients with PCa (n = 20) and CP (n = 20) were immunolabeled and colorimetrically quantified with the pan-leukocyte marker CD45, with CD68 (macrophages), CD8 (cytotoxic T-lymphocytes), CD4 (T-helper cells), CD20 (B-lymphocytes), NCL-PC (plasma cells), neutrophil elastase, PRG2 (eosinophils), anti-mast cell (MC) tryptase and correlated to pain sensation. Perineural mast cell subtypes were analyzed by double immunolabeling with MC chymase. Expression and neural immunoreactivity of protease-activated receptor type 1 (PAR-1) and type 2 (PAR-2) were analyzed in PCa and CP and correlated to pain status of the patients.
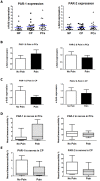
Results: In PCa and CP, nerves were predominantly infiltrated by cytotoxic T-lymphocytes (PCa: 35% of all perineural inflammatory cells, CP: 33%), macrophages (PCa: 39%, CP: 33%) and MC (PCa: 21%, CP: 27%). In both entities, neuropathic pain sensation was associated with a specific increase of perineural MC (PCa without pain: 14% vs. PCa with pain: 31%; CP without pain: 19% vs. CP with pain: 34%), not affecting the frequency of other inflammatory cell subtypes. The vast majority of these MC contained MC chymase. PAR-1 and PAR-2 expression did not correlate to the pain sensation of PCa and CP patients.
Conclusion: Pancreatic neuritis in PC and CP is composed of cytotoxic T-lymphocytes, macrophages and MC. The specific enrichment of MC around intrapancreatic nerves in neuropathic pain due to PCa and CP suggests the presence of MC-induced visceral hypersensitivity in the pancreas. Therefore, pancreatic and enteric neuropathies seem to share a similar type of neuro-immune interaction in the generation of visceral pain.
Conflict of interest statement
Figures

References
-
- Ceyhan GO, Bergmann F, Kadihasanoglu M, Altintas B, Demir IE, et al.. (2009) Pancreatic neuropathy and neuropathic pain--a comprehensive pathomorphological study of 546 cases. Gastroenterology 136: : 177-186 e171. - PubMed
-
- Bockman DE, Buchler M, Malfertheiner P, Beger HG (1988) Analysis of nerves in chronic pancreatitis. Gastroenterology 94: 1459–1469. - PubMed
-
- Ceyhan GO, Demir IE, Maak M, Friess H (2010) Fate of nerves in chronic pancreatitis: Neural remodeling and pancreatic neuropathy. Best Pract Res Clin Gastroenterol 24: 311–322. - PubMed
-
- Di Sebastiano P, Fink T, Weihe E, Friess H, Innocenti P, et al. (1997) Immune cell infiltration and growth-associated protein 43 expression correlate with pain in chronic pancreatitis. Gastroenterology 112: 1648–1655. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

