Enhanced bone regeneration in rat calvarial defects implanted with surface-modified and BMP-loaded bioactive glass (13-93) scaffolds
- PMID: 23567939
- PMCID: PMC3669642
- DOI: 10.1016/j.actbio.2013.03.039
Enhanced bone regeneration in rat calvarial defects implanted with surface-modified and BMP-loaded bioactive glass (13-93) scaffolds
Abstract
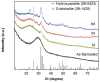
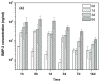
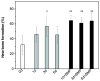
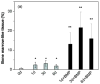
The repair of large bone defects, such as segmental defects in the long bones of the limbs, is a challenging clinical problem. Our recent work has shown the ability to create porous scaffolds of silicate 13-93 bioactive glass by robocasting which have compressive strengths comparable to human cortical bone. The objective of this study was to evaluate the capacity of those strong porous scaffolds with a grid-like microstructure (porosity=50%; filament width=330μm; pore width=300μm) to regenerate bone in a rat calvarial defect model. Six weeks post-implantation, the amount of new bone formed within the implants was evaluated using histomorphometric analysis. The amount of new bone formed in implants composed of the as-fabricated scaffolds was 32% of the available pore space (area). Pretreating the as-fabricated scaffolds in an aqueous phosphate solution for 1, 3 and 6days to convert a surface layer to hydroxyapatite prior to implantation enhanced new bone formation to 46%, 57% and 45%, respectively. New bone formation in scaffolds pretreated for 1, 3 and 6days and loaded with bone morphogenetic protein-2 (BMP-2) (1μg per defect) was 65%, 61% and 64%, respectively. The results show that converting a surface layer of the glass to hydroxyapatite or loading the surface-treated scaffolds with BMP-2 can significantly improve the capacity of 13-93 bioactive glass scaffolds to regenerate bone in an osseous defect. Based on their mechanical properties evaluated previously and their capacity to regenerate bone found in this study, these 13-93 bioactive glass scaffolds, pretreated or loaded with BMP-2, are promising in structural bone repair.
Copyright © 2013 Acta Materialia Inc. Published by Elsevier Ltd. All rights reserved.
Figures







Similar articles
-
Effect of bioactive borate glass microstructure on bone regeneration, angiogenesis, and hydroxyapatite conversion in a rat calvarial defect model.Acta Biomater. 2013 Aug;9(8):8015-26. doi: 10.1016/j.actbio.2013.04.043. Epub 2013 May 2. Acta Biomater. 2013. PMID: 23643606
-
Hollow hydroxyapatite microspheres: a novel bioactive and osteoconductive carrier for controlled release of bone morphogenetic protein-2 in bone regeneration.Acta Biomater. 2013 Sep;9(9):8374-83. doi: 10.1016/j.actbio.2013.05.029. Epub 2013 Jun 5. Acta Biomater. 2013. PMID: 23747325 Free PMC article.
-
Bone regeneration in rat calvarial defects implanted with fibrous scaffolds composed of a mixture of silicate and borate bioactive glasses.Acta Biomater. 2013 Nov;9(11):9126-36. doi: 10.1016/j.actbio.2013.06.039. Epub 2013 Jul 1. Acta Biomater. 2013. PMID: 23827095
-
Regenerating bone with bioactive glass scaffolds: A review of in vivo studies in bone defect models.Acta Biomater. 2017 Oct 15;62:1-28. doi: 10.1016/j.actbio.2017.08.030. Epub 2017 Aug 24. Acta Biomater. 2017. PMID: 28844964 Review.
-
Bone repair scaffold coated with bone morphogenetic protein-2 for bone regeneration in murine calvarial defect model: Systematic review and quality evaluation.Int J Artif Organs. 2019 Jul;42(7):325-337. doi: 10.1177/0391398819834944. Epub 2019 Mar 25. Int J Artif Organs. 2019. PMID: 30905250
Cited by
-
Main 3D Manufacturing Techniques for Customized Bone Substitutes. A Systematic Review.Materials (Basel). 2021 May 12;14(10):2524. doi: 10.3390/ma14102524. Materials (Basel). 2021. PMID: 34066290 Free PMC article. Review.
-
Bone Healing in Rat Segmental Femur Defects with Graphene-PCL-Coated Borate-Based Bioactive Glass Scaffolds.Polymers (Basel). 2022 Sep 18;14(18):3898. doi: 10.3390/polym14183898. Polymers (Basel). 2022. PMID: 36146043 Free PMC article.
-
50 years of scanning electron microscopy of bone-a comprehensive overview of the important discoveries made and insights gained into bone material properties in health, disease, and taphonomy.Bone Res. 2019 May 22;7:15. doi: 10.1038/s41413-019-0053-z. eCollection 2019. Bone Res. 2019. PMID: 31123620 Free PMC article.
-
Relaxin enhances bone regeneration with BMP-2-loaded hydroxyapatite microspheres.J Biomed Mater Res A. 2020 May;108(5):1231-1242. doi: 10.1002/jbm.a.36897. Epub 2020 Feb 24. J Biomed Mater Res A. 2020. PMID: 32043751 Free PMC article.
-
Bone regeneration by nanohydroxyapatite/chitosan/poly(lactide-co-glycolide) scaffolds seeded with human umbilical cord mesenchymal stem cells in the calvarial defects of the nude mice.Biomed Res Int. 2015;2015:261938. doi: 10.1155/2015/261938. Epub 2015 Oct 13. Biomed Res Int. 2015. PMID: 26550565 Free PMC article.
References
-
- Cancedda R, Giannoni P, Mastrogiacomo M. A tissue engineering approach to bone repair in large animal models and in clinical practice. Biomaterials. 2007;28:4240–50. - PubMed
-
- Giannoudis PV, Dinopoulos H, Tsiridis E. Bone substitutes: An update. Injury. 2005;36:S20–S7. - PubMed
-
- Laurencin C, Khan Y, El-Amin SF. Bone graft substitutes. Expert Rev Med Devices. 2006;3:49–57. - PubMed
-
- Hench LL. Bioceramics. J Am Ceram Soc. 1998;81:1705–28.
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

