Endothelial junction regulation: a prerequisite for leukocytes crossing the vessel wall
- PMID: 23571667
- PMCID: PMC6741525
- DOI: 10.1159/000348828
Endothelial junction regulation: a prerequisite for leukocytes crossing the vessel wall
Abstract
The leukocytes of the innate immune system, especially neutrophils and monocytes, exit the circulation early in the response to local inflammation and infection. This is necessary to control and prevent the spread of infections before an adaptive immune response can be raised. The endothelial cells and the intercellular junctions that connect them form a barrier that leukocytes need to pass in order to get to the site of inflammation. The junctions are tightly regulated which ensures that leukocytes only exit when and where they are needed. This regulation is disturbed in many chronic inflammatory diseases which are characterized by ongoing recruitment and interstitial accumulation of leukocytes. In this review, we summarize the molecular mechanisms that regulate endothelial cell-cell junctions and prevent or permit leukocyte transendothelial migration.
Copyright © 2013 S. Karger AG, Basel.
Figures

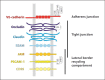
References
-
- Aird WC. Phenotypic heterogeneity of the endothelium. 1. Structure, function, and mechanisms. Circ Res. 2007;100:158–173. - PubMed
-
- Wolburg H, Lippoldt A. Tight junctions of the blood-brain barrier: development, composition and regulation. Vascul Pharmacol. 2002;38:323–337. - PubMed
-
- Miyasaka M, Tanaka T. Lymphocyte trafficking across high endothelial venules: dogmas and enigmas. Nat Rev Immunol. 2004;4:360–370. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

