Role of contrast-enhanced ultrasonography in percutaneous radiofrequency ablation of liver metastases and efficacy evaluation
- PMID: 23592894
- PMCID: PMC3626975
- DOI: 10.3978/j.issn.1000-9604.2013.01.02
Role of contrast-enhanced ultrasonography in percutaneous radiofrequency ablation of liver metastases and efficacy evaluation
Abstract
Objective: To retrospectively investigate the role of contrast-enhanced ultrasonography (CEUS) in percutaneous radiofrequency ablation (RFA) in patients with liver metastases and evaluate the therapeutic efficacy of RFA assisted by CEUS.
Methods: From May 2004 to September 2010, 136 patients with 219 liver metastatic lesions received CEUS examination 1 h before RFA (CEUS group), and other 126 patients with 216 lesions without CEUS examination in the earlier period were served as a historical control group. The mean tumor size was 3.2 cm and the mean tumor number was 1.6 in the CEUS group, while 3.4 cm and 1.7 in the control group, respectively (P>0.05). The clinical characteristics, recurrence results and survival outcomes were compared between two groups.
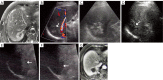
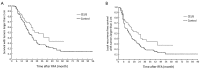
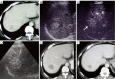
Results: In the CEUS group, two isoechoic tumors were not demonstrated on unenhanced ultrasonography (US), and 63 (47%) of 134 tumors examined with CEUS were 0.3 cm larger than with unenhanced US. Furthermore, in 18.4% of 136 patients, additional 1-3 tumors were detected on CEUS. The CEUS group showed higher early tumor necrosis and lower intrahepatic recurrence than the control group. The 3-year overall survival (OS) rate and the 3-year local recurrence-free survival (LRFS) rate in the CEUS group were 50.1% and 38.3%, in contrast to 25.3% and 19.3% in the control group, respectively (P=0.002 and P<0.001).
Conclusions: CEUS provides important information for RFA treatment in patients with liver metastases and better therapeutic effect could be attained.
Keywords: Contrast media; liver metastases; radiofrequency ablation; ultrasonography.
Figures




Similar articles
-
Role of contrast enhanced ultrasound in radiofrequency ablation of metastatic liver carcinoma.Chin J Cancer Res. 2012 Mar;24(1):44-51. doi: 10.1007/s11670-012-0044-8. Chin J Cancer Res. 2012. PMID: 23359761 Free PMC article.
-
[Efficacy of radiofrequency ablation to treat advanced hepatocellular carcinoma].Zhonghua Gan Zang Bing Za Zhi. 2012 Apr;20(4):256-60. doi: 10.3760/cma.j.issn.1007-3418.2012.04.006. Zhonghua Gan Zang Bing Za Zhi. 2012. PMID: 22964144 Chinese.
-
The role of contrast-enhanced ultrasound in planning treatment protocols for hepatocellular carcinoma before radiofrequency ablation.Clin Radiol. 2007 Aug;62(8):752-60. doi: 10.1016/j.crad.2006.12.013. Epub 2007 Jun 4. Clin Radiol. 2007. PMID: 17604763
-
[Application of contrast-enhanced ultrasonography in selecting indication of radiofrequency ablation among hepatocellular carcinoma patients].Zhonghua Yi Xue Za Zhi. 2005 Dec 28;85(49):3491-4. Zhonghua Yi Xue Za Zhi. 2005. PMID: 16686066 Clinical Trial. Chinese.
-
Radiofrequency ablation of liver tumors: the role of microbubble ultrasound contrast agents.Ultrasound Q. 2006 Mar;22(1):41-7. Ultrasound Q. 2006. PMID: 16641792 Review.
Cited by
-
Comparison of real-time contrast-enhanced ultrasonography and standard ultrasonography in liver cancer microwave ablation.Exp Ther Med. 2016 Sep;12(3):1345-1348. doi: 10.3892/etm.2016.3448. Epub 2016 Jun 10. Exp Ther Med. 2016. PMID: 27602065 Free PMC article.
-
Acoustic radiation force impulse elastography for efficacy evaluation after hepatocellular carcinoma radiofrequency ablation: a comparative study with contrast-enhanced ultrasound.Biomed Res Int. 2014;2014:901642. doi: 10.1155/2014/901642. Epub 2014 May 6. Biomed Res Int. 2014. PMID: 24895624 Free PMC article.
-
Study of ultrasound-guided percutaneous microwave ablation combined with portal vein embolization for rapid future liver remnant increase of planned hepatectomy.Front Oncol. 2023 Jan 4;12:926810. doi: 10.3389/fonc.2022.926810. eCollection 2022. Front Oncol. 2023. PMID: 36686725 Free PMC article.
-
[Interventional sonography of the liver and kidneys].Radiologe. 2013 Nov;53(11):962-73. doi: 10.1007/s00117-012-2459-0. Radiologe. 2013. PMID: 24177722 German.
-
Early Diagnosis of Intrahepatic Pseudoaneurysm during Radiofrequency Ablation using Contrast-Enhanced Ultrasound.Malays J Med Sci. 2015 Nov;22(6):58-62. Malays J Med Sci. 2015. PMID: 28223887 Free PMC article.
References
-
- Stang A, Keles H, von Seydewitz C, et al. Percutanous and intraoperative ultrasound-guided radiofrequency ablation of hepatic tumours. Ultraschall Med 2007;28:181-8 - PubMed
-
- Gillams AR, Lees WR. Five-year survival in 309 patients with colorectal liver metastases treated with radiofrequency ablation. Eur Radiol 2009;19:1206-13 - PubMed
-
- Chen MH, Wei Y, Yan K, et al. Treatment strategy to optimize radiofrequency ablation for liver malignancies. J Vasc Interv Radiol 2006;17:671-83 - PubMed
-
- Wu JY, Chen MH, Yan k, et al. Ultrasound-guided radiofrequency ablation in the treatment of liver metastases. Journal of Beijing Medical University 2001;33:449-51
LinkOut - more resources
Full Text Sources
