Giant anterior chest wall basal cell carcinoma: a reconstructive challenge and review of the literature
- PMID: 23598936
- PMCID: PMC3645802
- DOI: 10.1136/bcr-2013-008871
Giant anterior chest wall basal cell carcinoma: a reconstructive challenge and review of the literature
Abstract
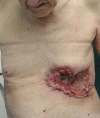
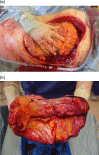
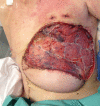
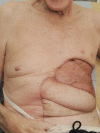
Giant basal cell carcinomas (GBCC) are rare, accounting for <1% of BCCs. Those occurring on the anterior chest wall are a very rare subset that brings particular reconstructive challenges. We describe a 75-year-old man whose 13.5 cm diameter ulcerating GBCC on his left anterior chest came to medical attention following a fall. The lesion was resected en-bloc with adjacent ribs, and reconstructed with an omental flap, superiorly pedicled vertical rectus abdominus myocutaneous (VRAM) flap and split skin grafting. While the myriad reasons for delayed presentation of giant cutaneous malignancies are well documented, the complex nature of reconstruction and requirement for an integrated multidisciplinary approach are less so. It is of importance to note that the cicatricial nature of these lesions may result in a much larger defect requiring reconstruction than appreciated prior to resection. Documented cases of anterior chest wall GBCC and the treatment strategies employed are reviewed.
Figures
References
-
- Randle HW, Roenigk RK, Brodland DG. Giant basal cell carcinoma (T3): who is at risk? Cancer 1993;2013:1624–30 - PubMed
-
- Archontaki M, Stavrianos SP, Korkolis DP, et al. Giant basal cell carcinoma: clinicopathological analysis of 51 cases and review of the literature. Anticancer Res 2009;2013:2655–64 - PubMed
-
- Horlock N, Wilson GD, Daley FM, et al. Cellular proliferation characteristics do not account for the behaviour of horrifying basal cell carcinoma. A comparison of the growth fraction of horrifying and non-horrifying tumours. Br J Plast Surg 1998;2013:59–66 - PubMed
-
- Snow SN, Sahl W, Lo JS, et al. Metastatic basal cell carcinoma. Cancer 1994;2013:328–35 - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
