The role of the intestinal microcirculation in necrotizing enterocolitis
- PMID: 23611611
- PMCID: PMC3646103
- DOI: 10.1053/j.sempedsurg.2013.01.004
The role of the intestinal microcirculation in necrotizing enterocolitis
Abstract
Necrotizing enterocolitis (NEC) continues to be a devastating inflammatory disease of the newborn intestine. Despite advances in management, morbidity and mortality remain high. While it is clear that intestinal ischemia plays a large role in disease pathogenesis, attempts to link NEC to intestinal macrovascular derangement have been largely unsuccessful. More recently, there has been a concerted effort to characterize the pathologic changes of the intestinal microcirculation in response to intestinal injury, including NEC. This microcirculatory regulation is controlled by a balance of vasoconstrictor and vasodilator forces. Vasoconstriction is mediated primarily by endothelin-1 (ET-1), while vasodilation is mediated primarily by nitric oxide (NO). These chemical mediators have been implicated in many aspects of intestinal ischemic injury and NEC, with the balance shifting toward increased vasoconstriction associated with intestinal injury. With a proper understanding of these antagonistic forces, potential therapeutic avenues may result from improving this pathologic microcirculatory dysregulation.
Copyright © 2013 Elsevier Inc. All rights reserved.
Figures
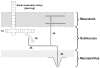
Similar articles
-
The neonatal intestinal vasculature: contributing factors to necrotizing enterocolitis.Semin Perinatol. 2008 Apr;32(2):83-91. doi: 10.1053/j.semperi.2008.01.003. Semin Perinatol. 2008. PMID: 18346531 Review.
-
Intestinal microcirculatory dysfunction and neonatal necrotizing enterocolitis.Chin Med J (Engl). 2013;126(9):1771-8. Chin Med J (Engl). 2013. PMID: 23652066 Review.
-
Ischemia and necrotizing enterocolitis: where, when, and how.Semin Pediatr Surg. 2005 Aug;14(3):152-8. doi: 10.1053/j.sempedsurg.2005.05.003. Semin Pediatr Surg. 2005. PMID: 16084402 Review.
-
Pathogenesis of NEC: Role of the innate and adaptive immune response.Semin Perinatol. 2017 Feb;41(1):15-28. doi: 10.1053/j.semperi.2016.09.014. Epub 2016 Dec 9. Semin Perinatol. 2017. PMID: 27940091 Free PMC article. Review.
-
Remote ischemic conditioning counteracts the intestinal damage of necrotizing enterocolitis by improving intestinal microcirculation.Nat Commun. 2020 Oct 2;11(1):4950. doi: 10.1038/s41467-020-18750-9. Nat Commun. 2020. PMID: 33009377 Free PMC article.
Cited by
-
The T2 Toxin Produced by Fusarium spp. Impacts Porcine Duodenal Nitric Oxide Synthase (nNOS)-Positive Nervous Structures-The Preliminary Study.Int J Mol Sci. 2020 Jul 20;21(14):5118. doi: 10.3390/ijms21145118. Int J Mol Sci. 2020. PMID: 32698434 Free PMC article.
-
Epithelial restitution defect in neonatal jejunum is rescued by juvenile mucosal homogenate in a pig model of intestinal ischemic injury and repair.PLoS One. 2018 Aug 23;13(8):e0200674. doi: 10.1371/journal.pone.0200674. eCollection 2018. PLoS One. 2018. PMID: 30138372 Free PMC article.
-
Transfusion-related Gut Injury and Necrotizing Enterocolitis.Clin Perinatol. 2020 Jun;47(2):399-412. doi: 10.1016/j.clp.2020.02.002. Epub 2020 Feb 20. Clin Perinatol. 2020. PMID: 32439119 Free PMC article. Review.
-
Risk of Necrotizing Enterocolitis Associated With the Single Nucleotide Polymorphisms VEGF C-2578A, IL-18 C-607A, and IL-4 Receptor α-Chain A-1902G: A Validation Study in a Prospective Multicenter Cohort.Front Pediatr. 2020 Feb 18;8:45. doi: 10.3389/fped.2020.00045. eCollection 2020. Front Pediatr. 2020. PMID: 32133331 Free PMC article.
-
Dietary intake and bio-activation of nitrite and nitrate in newborn infants.Pediatr Res. 2015 Jan;77(1-2):173-81. doi: 10.1038/pr.2014.168. Epub 2014 Oct 14. Pediatr Res. 2015. PMID: 25314582 Free PMC article. Review.
References
-
- Balance WA, Dahms BB, Shenker N, et al. Pathology of neonatal necrotizing enterocolitis: a ten year experience. J Pediatr. 1990;117:S6–S13. - PubMed
-
- Guthrie SO, Gordon PV, Thomas V, et al. Necrotizing enterocolitis among neonates in the United States. J Perinatol. 2003;56:278–85. - PubMed
-
- Luig M, Lui K, NSW ACT NICUS Group. Epidemiology of necrotizing enterocolitis. II. Risks and susceptibility of premature infants during the surfactant era: a regional study. J Paediatr Child Health. 2005;41(4):174–9. - PubMed
-
- Guillet R, Stoll BJ, Cotton CM, et al. Association of H2-blocker therapy and higher incidence of necrotizing enterocolitis in very low birth weight infants. Pediatrics. 2006;117(2):e137–42. - PubMed
-
- Llanos AR, Moss ME, Pinzon MC, et al. Epidemiology of neonatal necrotizing enterocolitis: a population-based study. Paediatr Perinat Epidemiol. 2002;16(4):342–9. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

