Transplantation-associated long-term immunosuppression promotes oral colonization by potentially opportunistic pathogens without impacting other members of the salivary bacteriome
- PMID: 23616410
- PMCID: PMC3675961
- DOI: 10.1128/CVI.00734-12
Transplantation-associated long-term immunosuppression promotes oral colonization by potentially opportunistic pathogens without impacting other members of the salivary bacteriome
Abstract
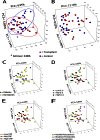
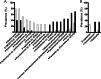
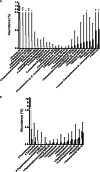
Solid-organ transplant recipients rely on pharmacological immunosuppression to prevent allograft rejection. The effect of such chronic immunosuppression on the microflora at mucosal surfaces is not known. We evaluated the salivary bacterial microbiome of 20 transplant recipients and 19 nonimmunosuppressed controls via 454 pyrosequencing of 16S rRNA gene amplicons. Alpha-diversity and global community structure did not differ between transplant and control subjects. However, principal coordinate analysis showed differences in community membership. Taxa more prevalent in transplant subjects included operational taxonomic units (OTUs) of potentially opportunistic Gammaproteobacteria such as Klebsiella pneumoniae, Pseudomonas fluorescens, Acinetobacter species, Vibrio species, Enterobacteriaceae species, and the genera Acinetobacter and Klebsiella. Transplant subjects also had increased proportions of Pseudomonas aeruginosa, Acinetobacter species, Enterobacteriaceae species, and Enterococcus faecalis, among other OTUs, while genera with increased proportions included Klebsiella, Acinetobacter, Staphylococcus, and Enterococcus. Furthermore, in transplant subjects, the dose of the immunosuppressant prednisone positively correlated with bacterial richness, while prednisone and mycophenolate mofetil doses positively correlated with the prevalence and proportions of transplant-associated taxa. Correlation network analysis of OTU relative abundance revealed a cluster containing potentially opportunistic pathogens as transplant associated. This cluster positively correlated with serum levels of C-reactive protein, suggesting a link between the resident flora at mucosal compartments and systemic inflammation. Network connectivity analysis revealed opportunistic pathogens as highly connected to each other and to common oral commensals, pointing to bacterial interactions that may influence colonization. This work demonstrates that immunosuppression aimed at limiting T-cell-mediated responses creates a more permissive oral environment for potentially opportunistic pathogens without affecting other members of the salivary bacteriome.
Figures

References
-
- Lechler RI, Sykes M, Thomson AW, Turka LA. 2005. Organ transplantation—how much of the promise has been realized? Nat. Med. 11:605–613 - PubMed
-
- Hlava N, Niemann CU, Gropper MA, Melcher ML. 2009. Postoperative infectious complications of abdominal solid organ transplantation. J. Intensive Care Med. 24:3–17 - PubMed
-
- Winters HA, Parbhoo RK, Schafer JJ, Goff DA. 2011. Extended-spectrum beta-lactamase-producing bacterial infections in adult solid organ transplant recipients. Ann. Pharmacother. 45:309–316 - PubMed
-
- Brown LR, Mackler BF, Levy BM, Wright TE, Handler SF, Moylan JS, Perkins DH, Keene HJ. 1979. Comparison of the plaque microflora in immunodeficient and immunocompetent dental patients. J. Dent. Res. 58:2344–2352 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

