Implementing and integrating a clinically driven electronic medical record for radiation oncology in a large medical enterprise
- PMID: 23616946
- PMCID: PMC3629369
- DOI: 10.3389/fonc.2013.00069
Implementing and integrating a clinically driven electronic medical record for radiation oncology in a large medical enterprise
Abstract
Purpose/objective: While our department is heavily invested in computer-based treatment planning, we historically relied on paper-based charts for management of Radiation Oncology patients. In early 2009, we initiated the process of conversion to an electronic medical record (EMR) eliminating the need for paper charts. Key goals included the ability to readily access information wherever and whenever needed, without compromising safety, treatment quality, confidentiality, or productivity.
Methodology: In February, 2009, we formed a multi-disciplinary team of Radiation Oncology physicians, nurses, therapists, administrators, physicists/dosimetrists, and information technology (IT) specialists, along with staff from the Duke Health System IT department. The team identified all existing processes and associated information/reports, established the framework for the EMR system and generated, tested and implemented specific EMR processes.
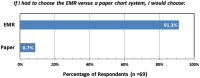
Results: Two broad classes of information were identified: information which must be readily accessed by anyone in the health system versus that used solely within the Radiation Oncology department. Examples of the former are consultation reports, weekly treatment check notes, and treatment summaries; the latter includes treatment plans, daily therapy records, and quality assurance reports. To manage the former, we utilized the enterprise-wide system, which required an intensive effort to design and implement procedures to export information from Radiation Oncology into that system. To manage "Radiation Oncology" data, we used our existing system (ARIA, Varian Medical Systems.) The ability to access both systems simultaneously from a single workstation (WS) was essential, requiring new WS and modified software. As of January, 2010, all new treatments were managed solely with an EMR. We find that an EMR makes information more widely accessible and does not compromise patient safety, treatment quality, or confidentiality. However, compared to paper charts, time required by clinicians to access/enter patient information has substantially increased. While productivity is improving with experience, substantial growth will require better integration of the system components, decreased access times, and improved user interfaces. $127K was spent on new hardware and software; elimination of paper yields projected savings of $21K/year. One year after conversion to an EMR, more than 90% of department staff favored the EMR over the previous paper charts.
Conclusion: Successful implementation of a Radiation Oncology EMR required not only the effort and commitment of all functions of the department, but support from senior health system management, corporate IT, and vendors. Realization of the full benefits of an EMR will require experience, faster/better integrated software, and continual improvement in underlying clinical processes.
Keywords: charts; electronic health record; electronic medical record; information technology; patient safety; quality assurance; radiation oncology practice.
Figures
References
-
- American Society for Radiation Oncology. (2012). Safety is No Accident: A Framework for Quality Radiation Oncology and Care. Fairfax: ASTRO
-
- Centers for Medicare & Medicaid Services, and HHS (2012). Medicare and medicaid programs; electronic health record incentive program – stage 2. Final rule. Fed. Regist. 77, 53967–54162 - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources