Risk of late-onset adhesions and incisional hernia repairs after surgery
- PMID: 23623220
- PMCID: PMC3769641
- DOI: 10.1016/j.jamcollsurg.2013.01.060
Risk of late-onset adhesions and incisional hernia repairs after surgery
Abstract
Background: Long-term adhesion-related complications and incisional hernias after abdominal surgery are common and costly. There are few data on the risk of these complications after different abdominal operations.
Study design: We identified Medicare beneficiaries who underwent endovascular repair of an abdominal aortic aneurysm from 2001-2008 who presumably are not at risk for laparotomy-related complications. We identified all laparoscopic and open operations involving the abdomen, pelvis, or retroperitoneum and categorized them into 5 groups according to invasiveness. We then identified laparotomy-related complications for up to 5 years after the index operation and compared these with the baseline rate of complications in a control group of patients who did not undergo an abdominal operation.
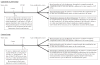
Results: We studied 85,663 patients, 7,513 (8.8%) of which underwent a laparotomy, including 2,783 major abdominal operations, 709 minor abdominal operations, 963 ventral hernia repairs, 493 retroperitoneal/pelvic operations, and 2,565 laparoscopic operations. Mean age was 76.7 years and 82.0% were male. Major abdominal operations carried the highest risk for adhesion-related complications (14.3% and 25.0% at 2 and 5 years compared with 4.0% and 7.8% for the control group; p < 0.001) and incisional hernias (7.8% and 12.0% compared with 0.6% and 1.2% for the control group; p < 0.001). Laparoscopic operations (4.6% and 10.7% for adhesions, 1.9% and 3.2% for incisional hernias) carried the lowest risk.
Conclusions: Late-onset laparotomy-related complications are frequent and their risk extends through 5 years beyond the perioperative period. With the advancement and expansion of laparoscopic techniques and its attendant lower risk for long-term complications, these results can alter the risk-to-benefit profile of various types of abdominal operations and can also strengthen the rationale for additional development of laparoscopic approaches to abdominal operations.
Copyright © 2013 American College of Surgeons. Published by Elsevier Inc. All rights reserved.
Figures

References
-
- Van Der Krabben AA, Dijkstra FR, Nieuwenhuijzen M, et al. Morbidity and mortality of inadvertent enterotomy during adhesiotomy. Br J Surg. 2000;87:467–471. - PubMed
-
- Mudge M, Hughes LE. Incisional hernia: a 10 year prospective study of incidence and attitudes. Br J Surg. 1985;72:70–71. - PubMed
-
- Sugerman HJ, Kellum JM, Reines HD, et al. Greater risk of incisional hernia with morbidly obese than steroid-dependent patients and low recurrence with prefascial polypropylene mesh. Am J Surg. 1996;171:80–84. - PubMed
-
- Anthony T, Bergen PC, Kim LT, et al. Factors affecting recurrence following incisional herniorrhaphy. World J Surg. 2000;24:95–100. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

