Nuclear imaging of the breast: translating achievements in instrumentation into clinical use
- PMID: 23635248
- PMCID: PMC3656956
- DOI: 10.1118/1.4802733
Nuclear imaging of the breast: translating achievements in instrumentation into clinical use
Abstract
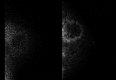
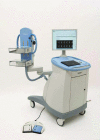
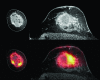
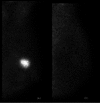
Approaches to imaging the breast with nuclear medicine and∕or molecular imaging methods have been under investigation since the late 1980s when a technique called scintimammography was first introduced. This review charts the progress of nuclear imaging of the breast over the last 20 years, covering the development of newer techniques such as breast specific gamma imaging, molecular breast imaging, and positron emission mammography. Key issues critical to the adoption of these technologies in the clinical environment are discussed, including the current status of clinical studies, the efforts at reducing the radiation dose from procedures associated with these technologies, and the relevant radiopharmaceuticals that are available or under development. The necessary steps required to move these technologies from bench to bedside are also discussed.
Figures





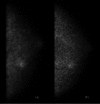
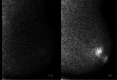
References
-
- Berg W. A., Madsen K. S., Schilling K., Tartar M., Pisano E. D., Larsen L. H., Narayanan D., Ozonoff A., Miller J. P., and Kalinyak J. E., “Breast cancer: Comparative effectiveness of positron emission mammo- graphy and MR imaging in presurgical planning for the ipsilateral breast,” Radiology 258, 59–72 (2011). 10.1148/radiol.10100454 - DOI - PMC - PubMed
-
- Berg W. A., Madsen K. S., Schilling K., Tartar M., Pisano E. D., Larsen L. H., Narayanan D., and Kalinyak J. E., “Comparative effectiveness of positron emission mammography and MRI in the contralateral breast of women with newly diagnosed breast cancer,” AJR, Am. J. Roentgenol. 198, 219–232 (2012). 10.2214/AJR.10.6342 - DOI - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

